What's new at SimplePractice
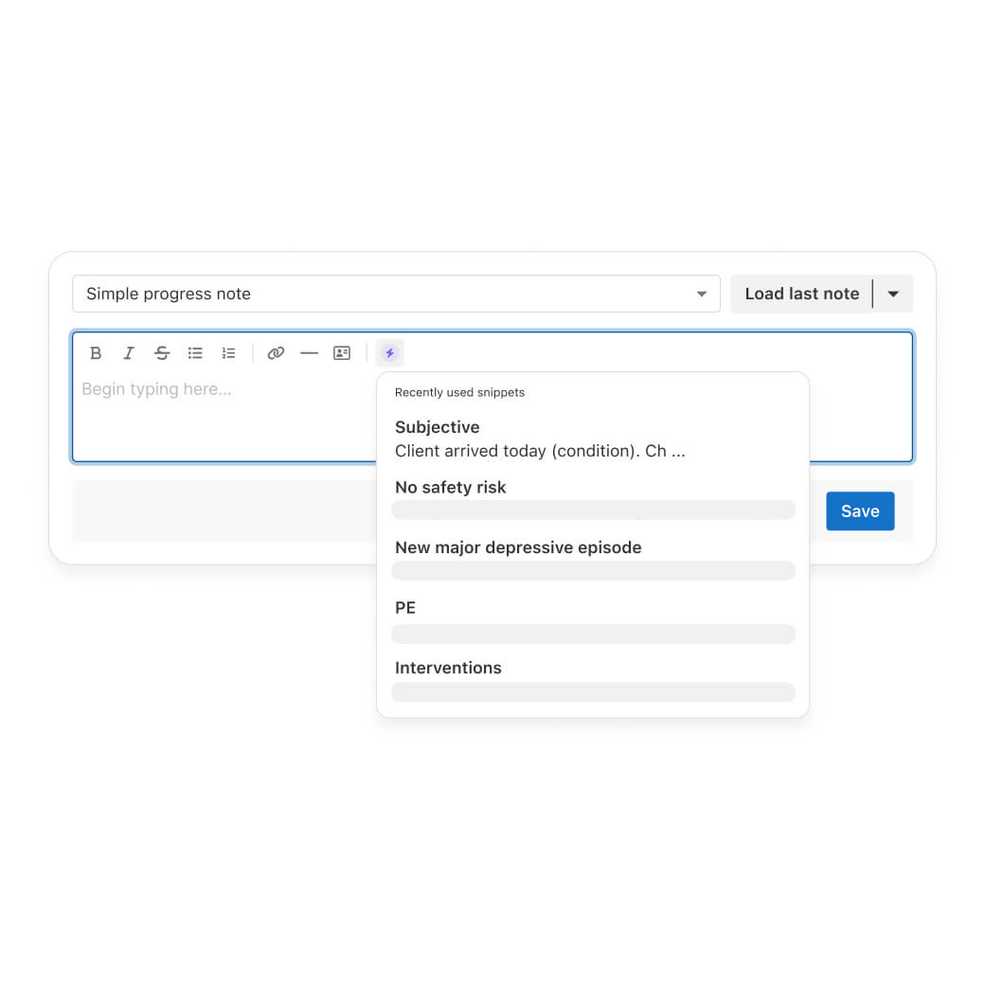
Save time on documentation with snippets
Create snippets for your go-to phrases, organize snippets into folders, and effortlessly use them while documenting in a client's chart. Make snippets available to your entire practice by adding them to your shared library.
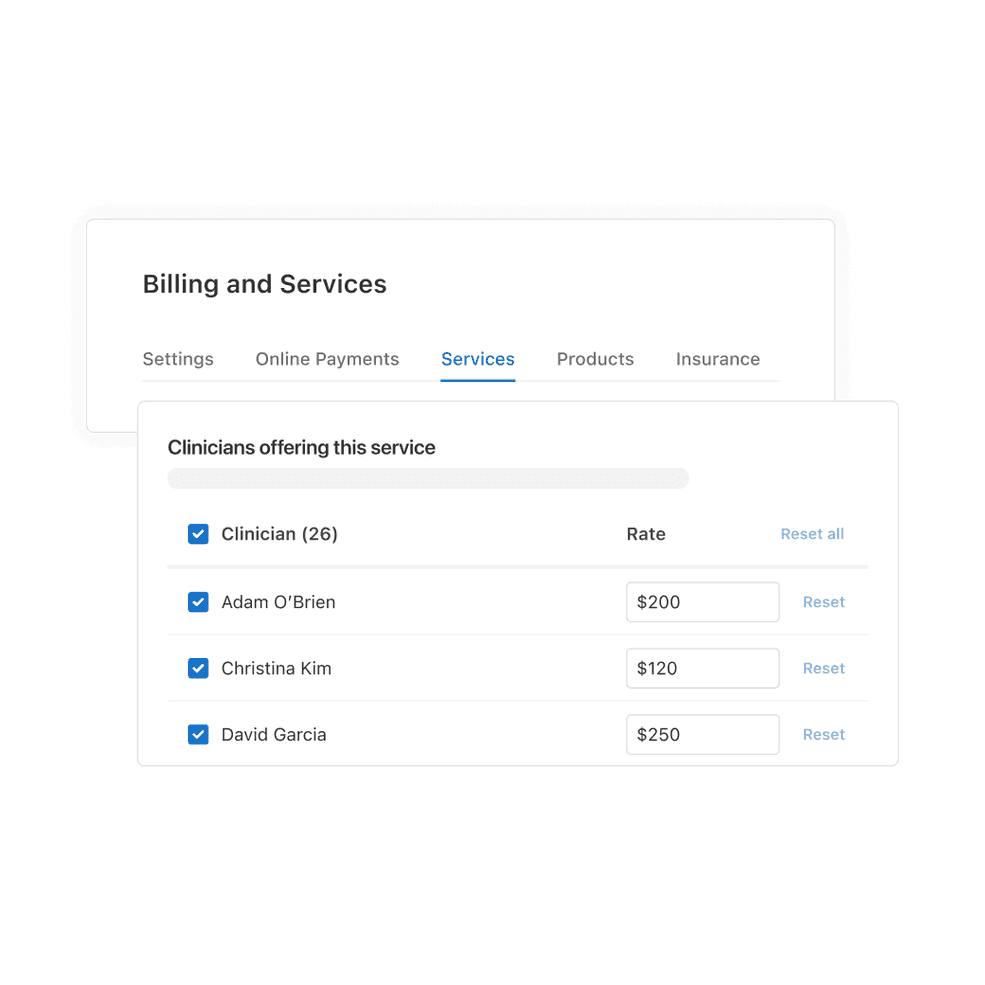
Reduce manual changes with rate tables
Ideal for practices with multiple clinicians billing the same CPT code, this new feature allows you to set individual rates, ensuring a customized approach to scheduling and billing.
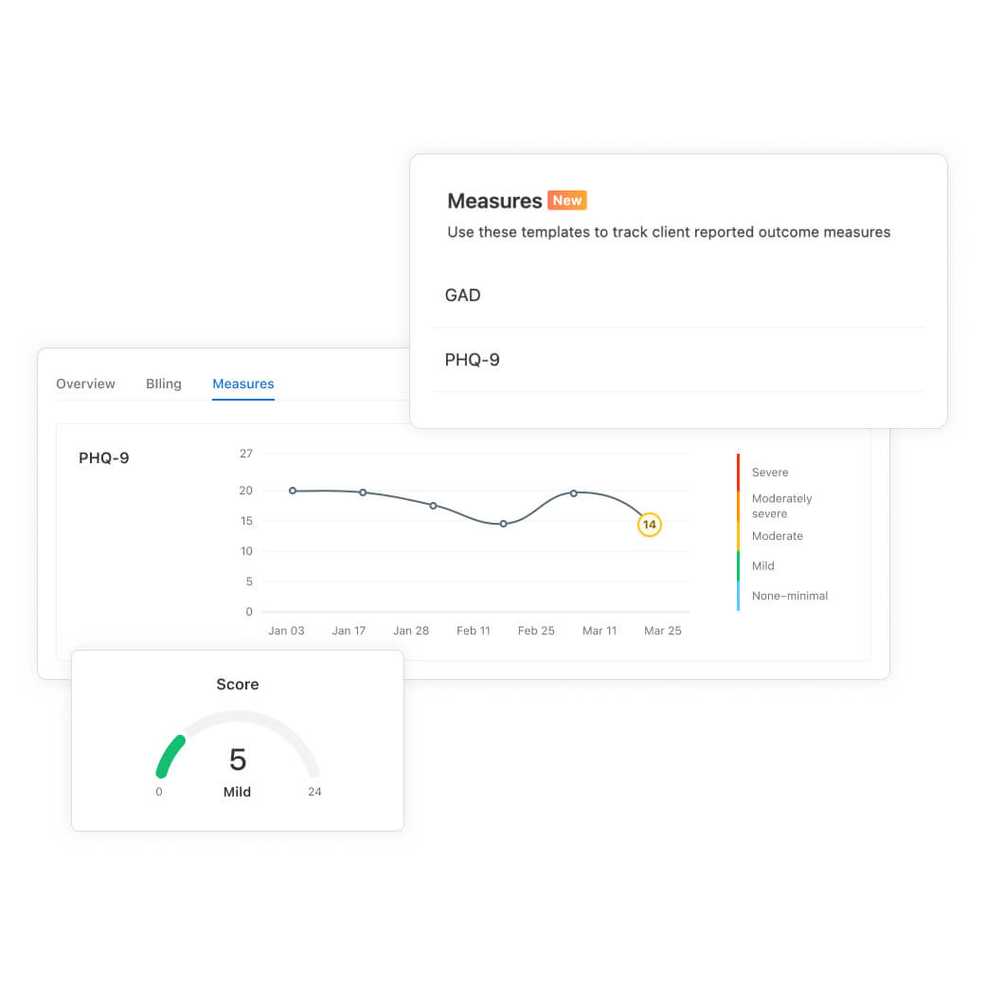
Improve client outcomes with measurement-based care tools
Help clients reach their goals with more confidence than ever. Keep track of measures, calculate scores, interpret results, and visualize your clients’ progress.
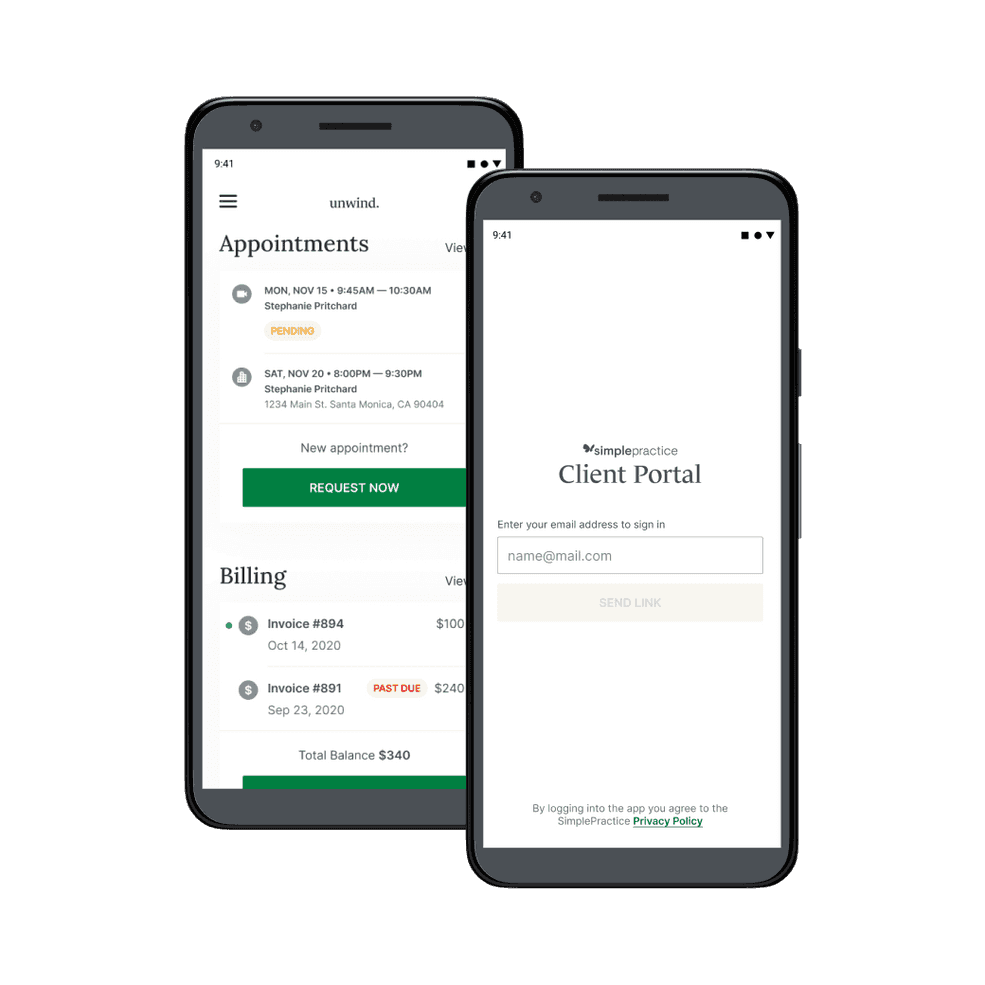
Introducing the Client Portal mobile app on Android!
All of the features your clients love on our iPhone Client Portal mobile app are now at their fingertips on Android! Offer your clients effortless and secure access to their appointments, secure messages, and much more.
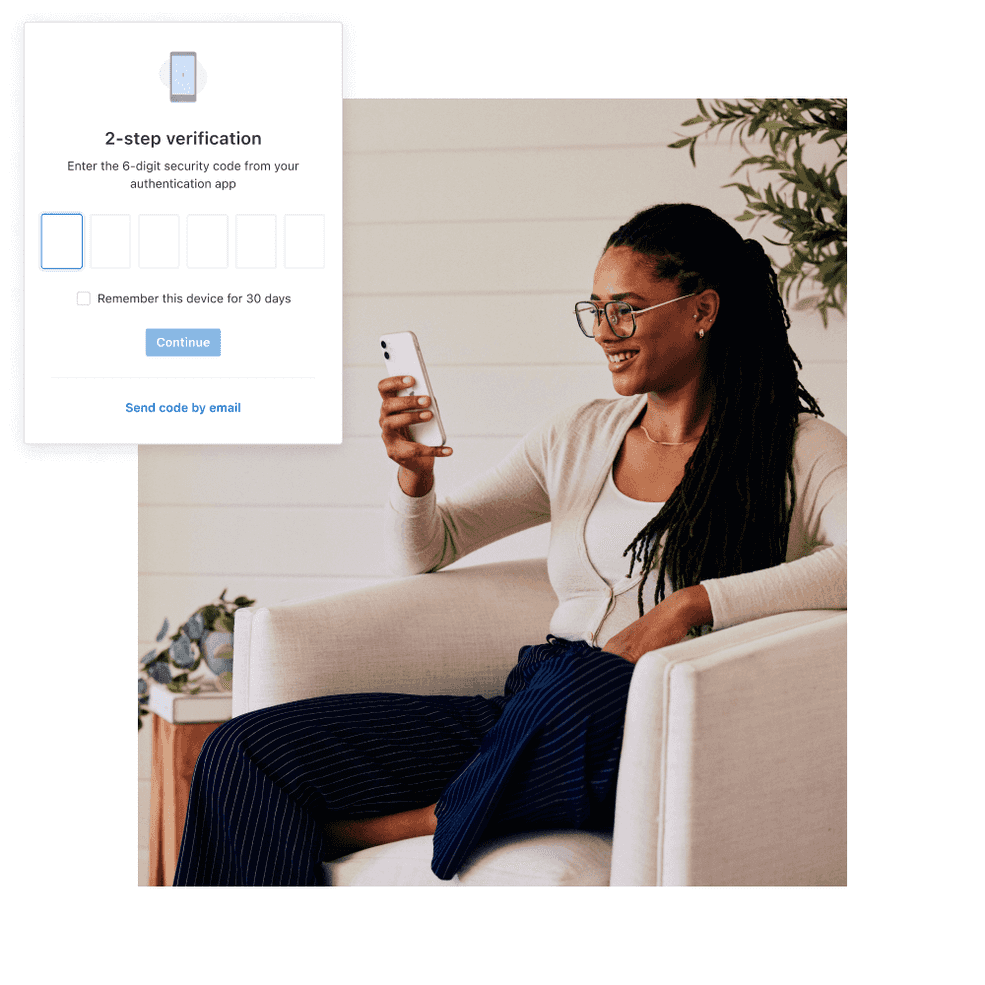
Easily update information and stay secure
Easily update your contact information and password on a new security page. Keep your data even more secure by enabling 2-step verification when signing into your account.
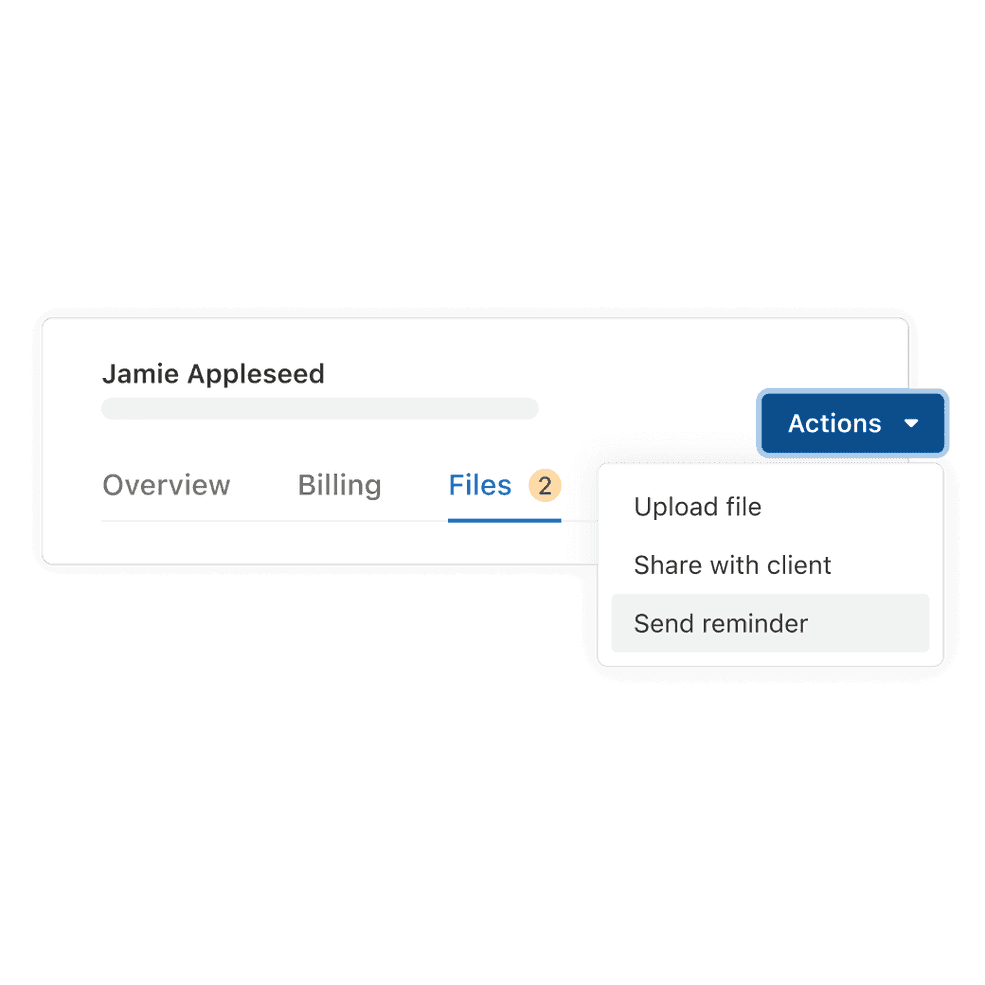
Use the Files tab to stay on top of client documentation
Keep track of client files in one place, see what’s been shared, and get updates when forms are completed with a new Files tab in each client profile.
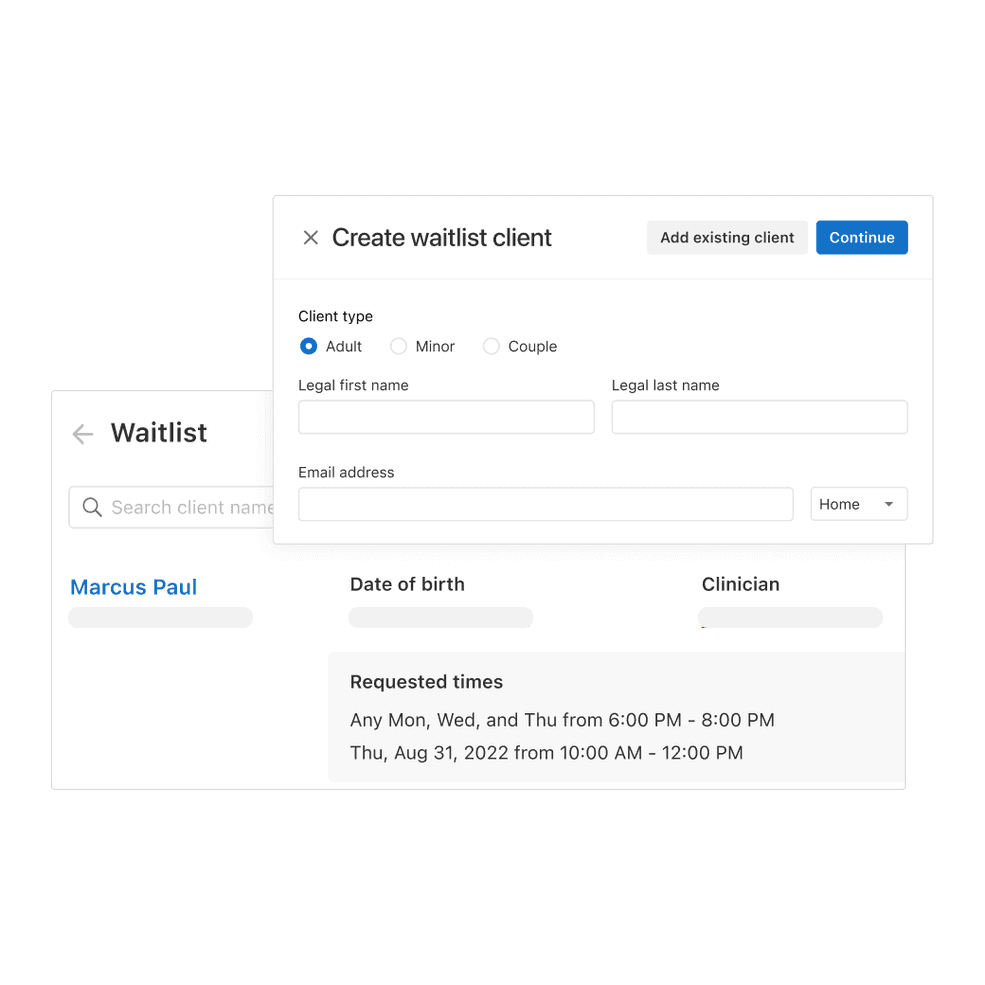
Simplify new client management
Use a new client waitlist that makes it easy to add clients, track appointment request details, schedule appointments directly from the calendar or waitlist, plus so much more. Available on the Plus plan only.
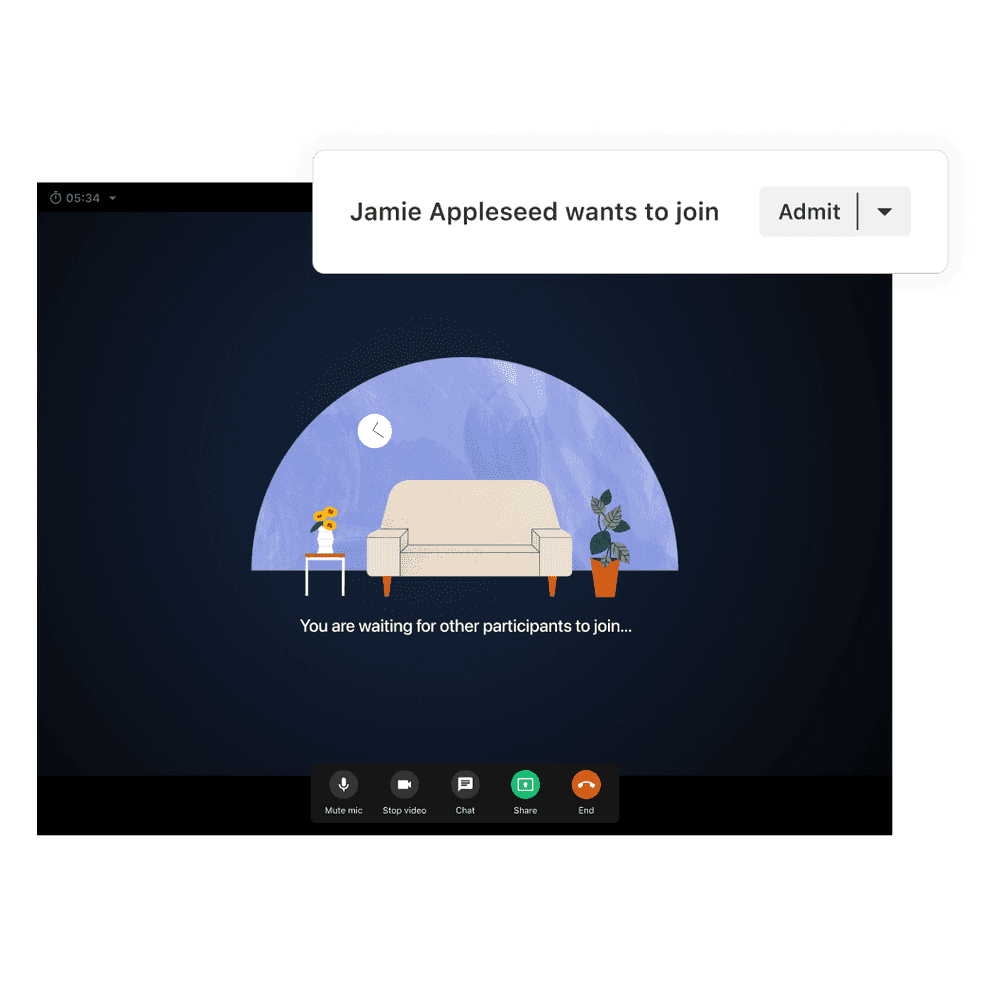
Run smoother telehealth sessions
Have more control over your telehealth sessions with a virtual waiting room that lets you admit clients and start sessions when you’re ready.
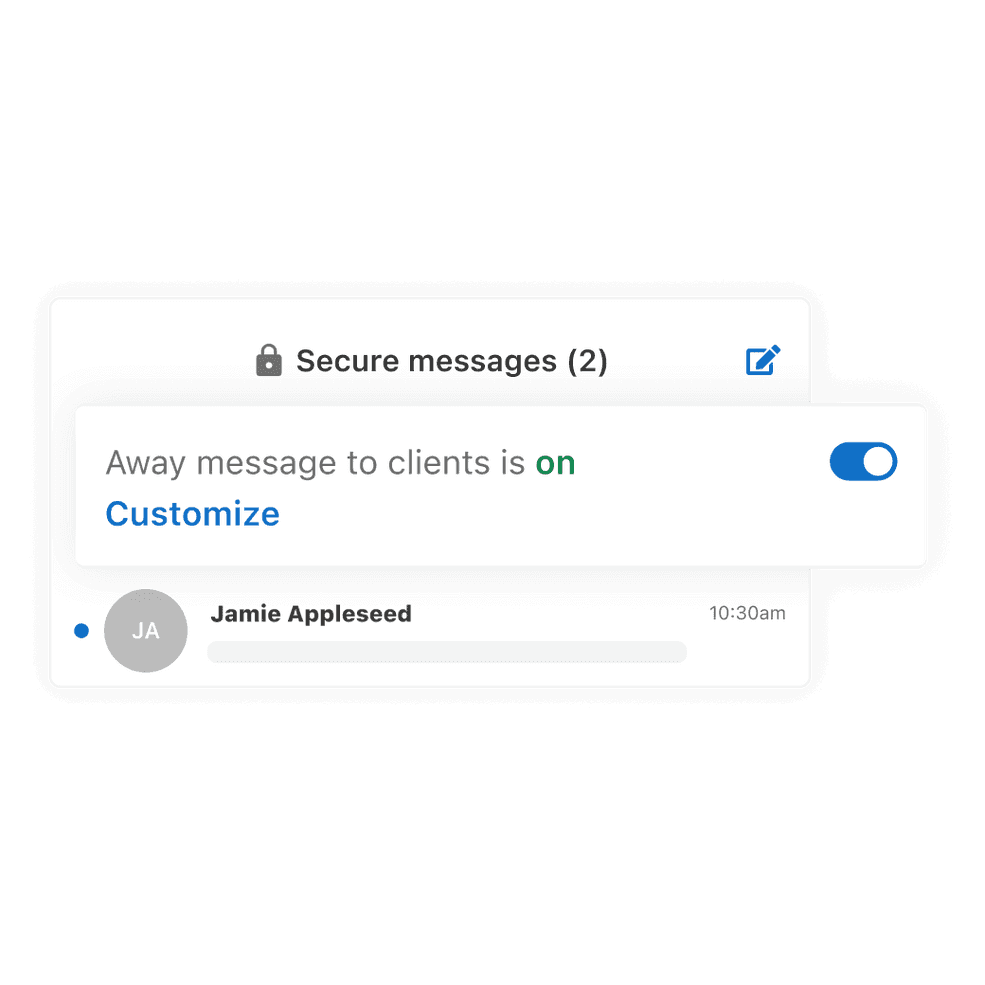
Let clients know when you’re away
Set up an auto-reply away message that’ll inform your clients when you’re out of office and unable to answer their messages. Available for all roles with access to secure messaging on the Essential and Plus plans only.
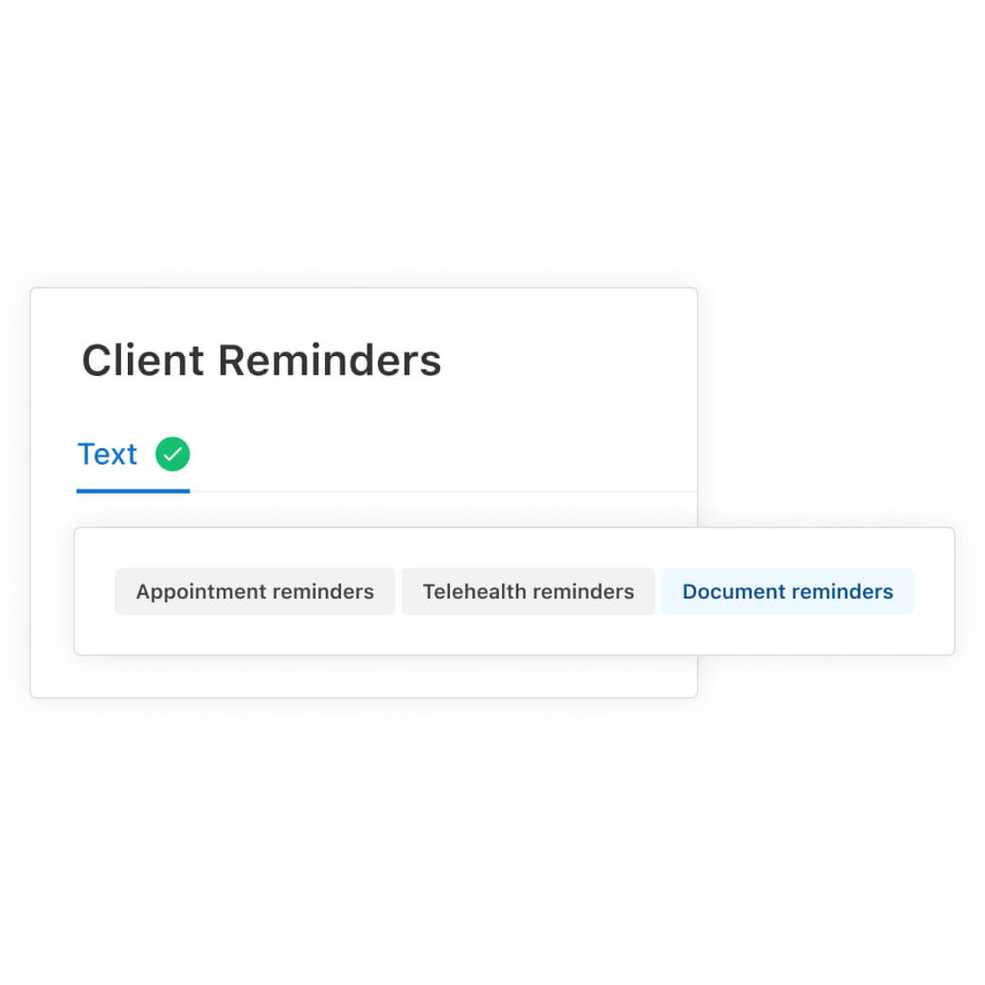
Remind clients to complete documents via text
Ensuring client paperwork is completed before appointments is easier than ever with our updated client text reminders. Simply enable text reminders for your client and the documentation reminder with a link to their client portal will automatically be sent to them.
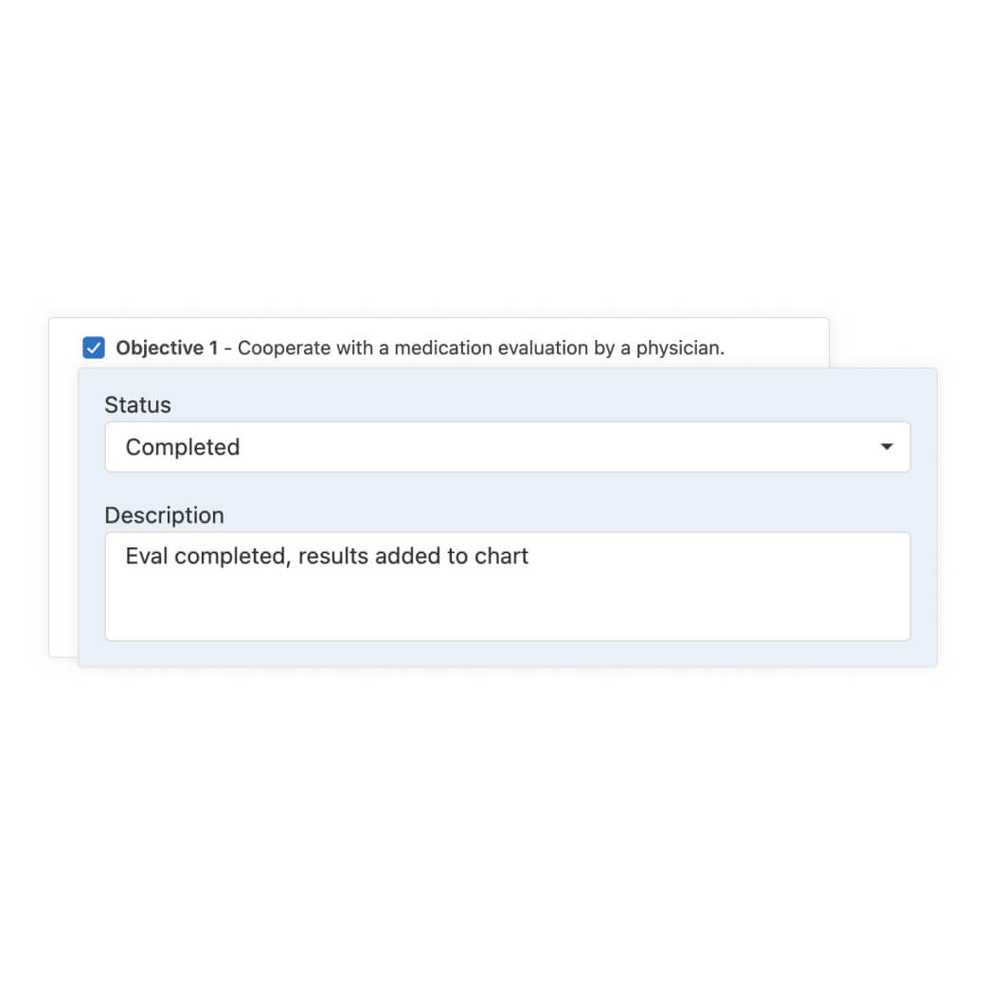
Track treatment plan progress
Add statuses for your client’s goals and objectives into your progress notes, exclusively for Wiley.
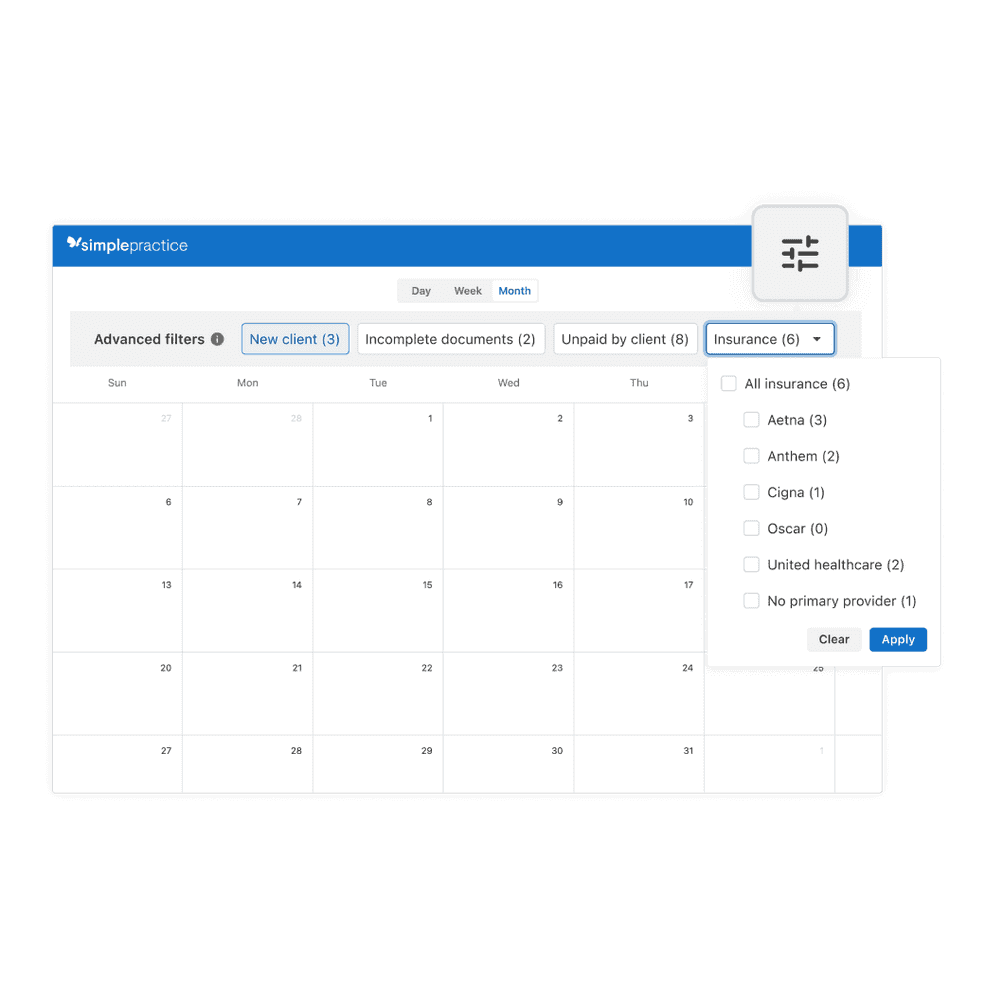
Save time with advanced calendar filters
Quickly filter appointments based on new client status, incomplete documents, unpaid balances, and insurance type—available for all roles on the Plus plan only.
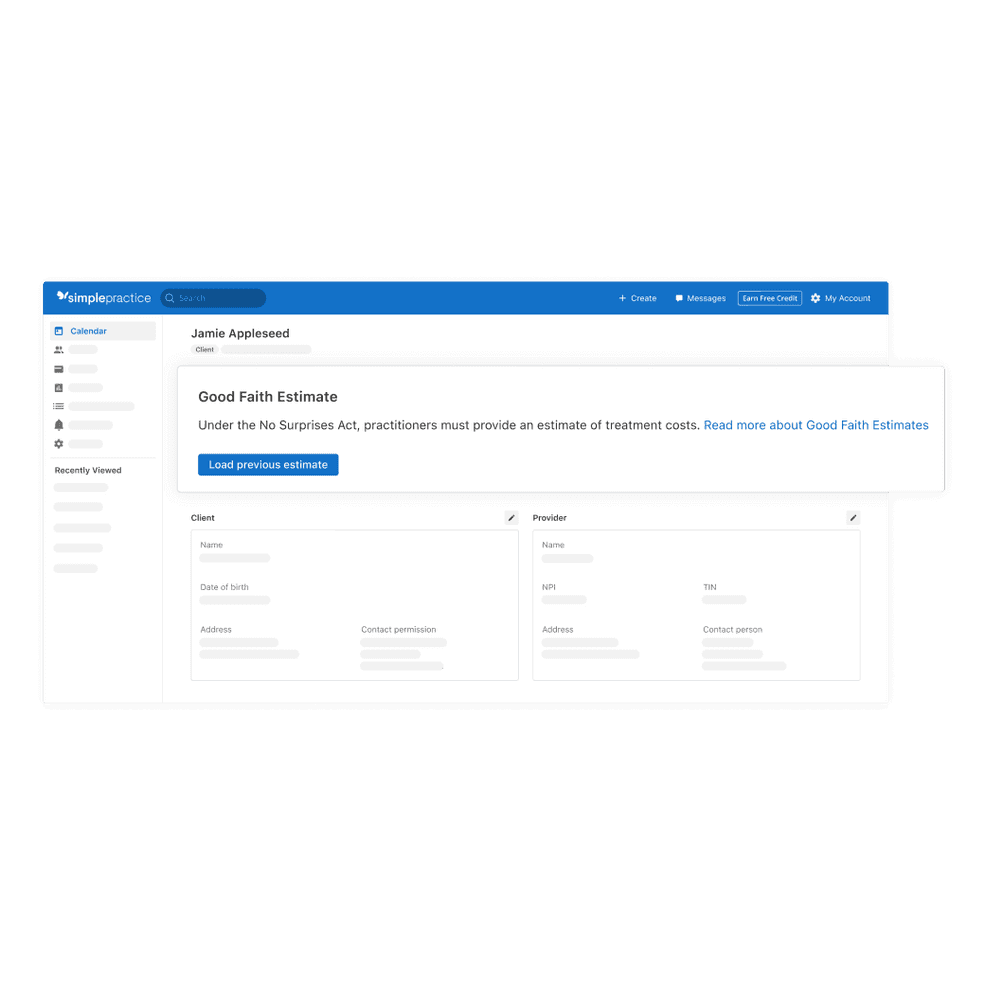
Easier ‘Good Faith Estimates’ for clients
Now you can quickly and easily generate your Good Faith Estimates. With just the click of a button, your forms will auto populate with the necessary client information from their chart, so you can spend less time manually creating them.
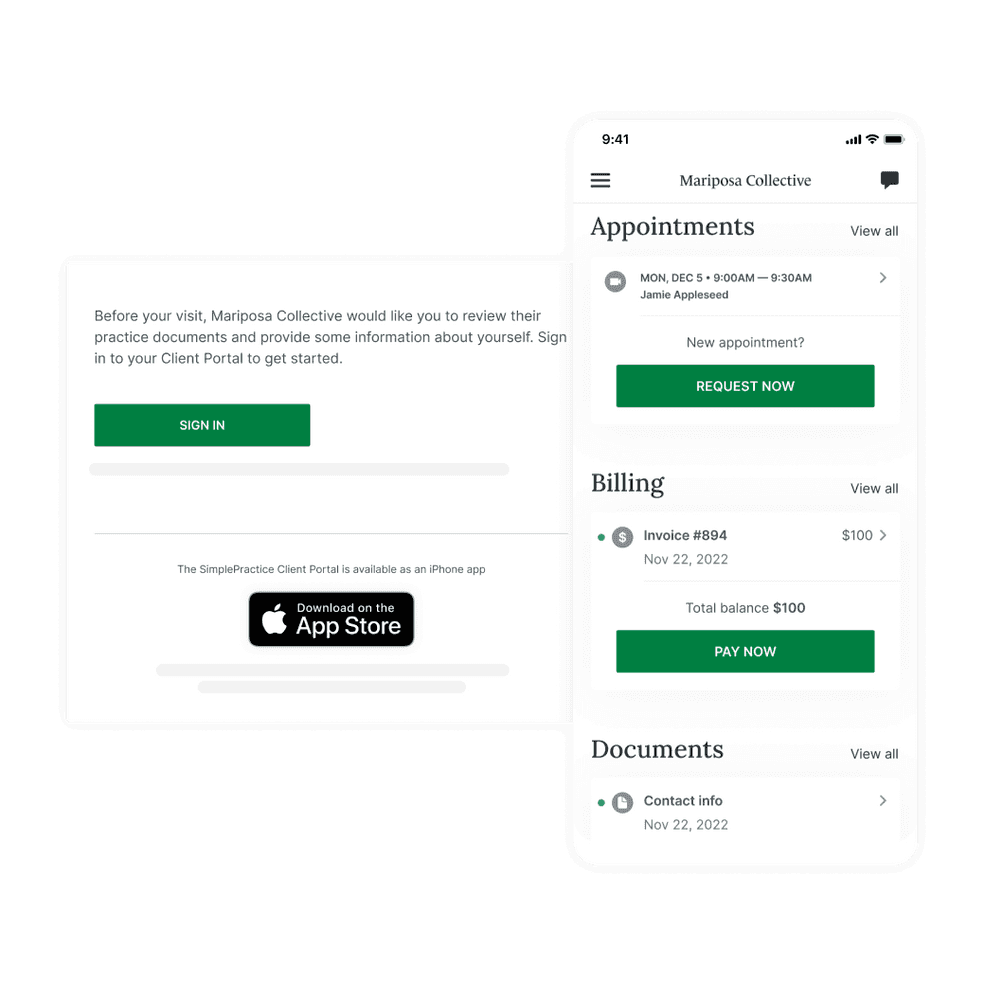
The Client Portal mobile app for iOS is here!
The SimplePractice Client Portal mobile app for iOS is available on the App Store! The link to download the app will be added to your Client Portal emails in phases. You’ll be notified when it has been added to the emails for your account.
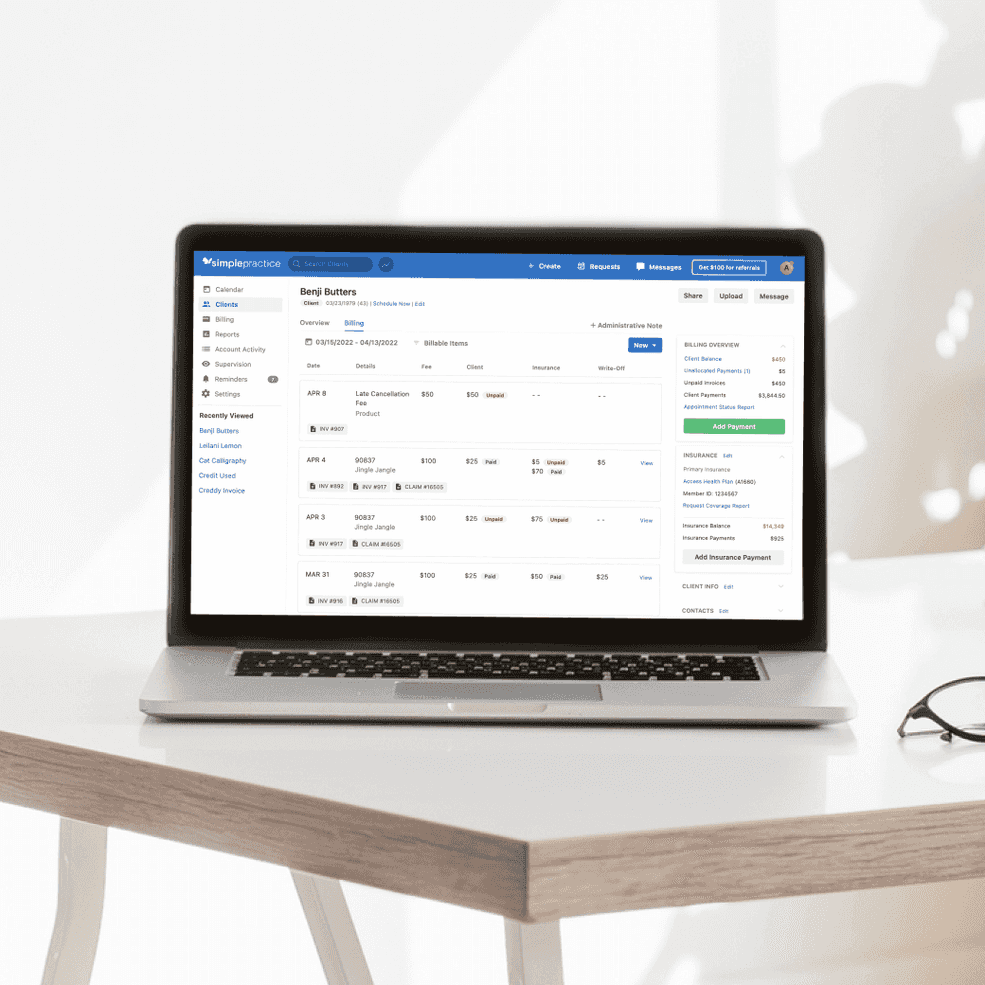
Do more with an updated billing experience
Get more control, transparency, and flexibility over your client payments. These updates allow you to easily apply client payments to specific invoices and to add partial payments to newly created invoices.
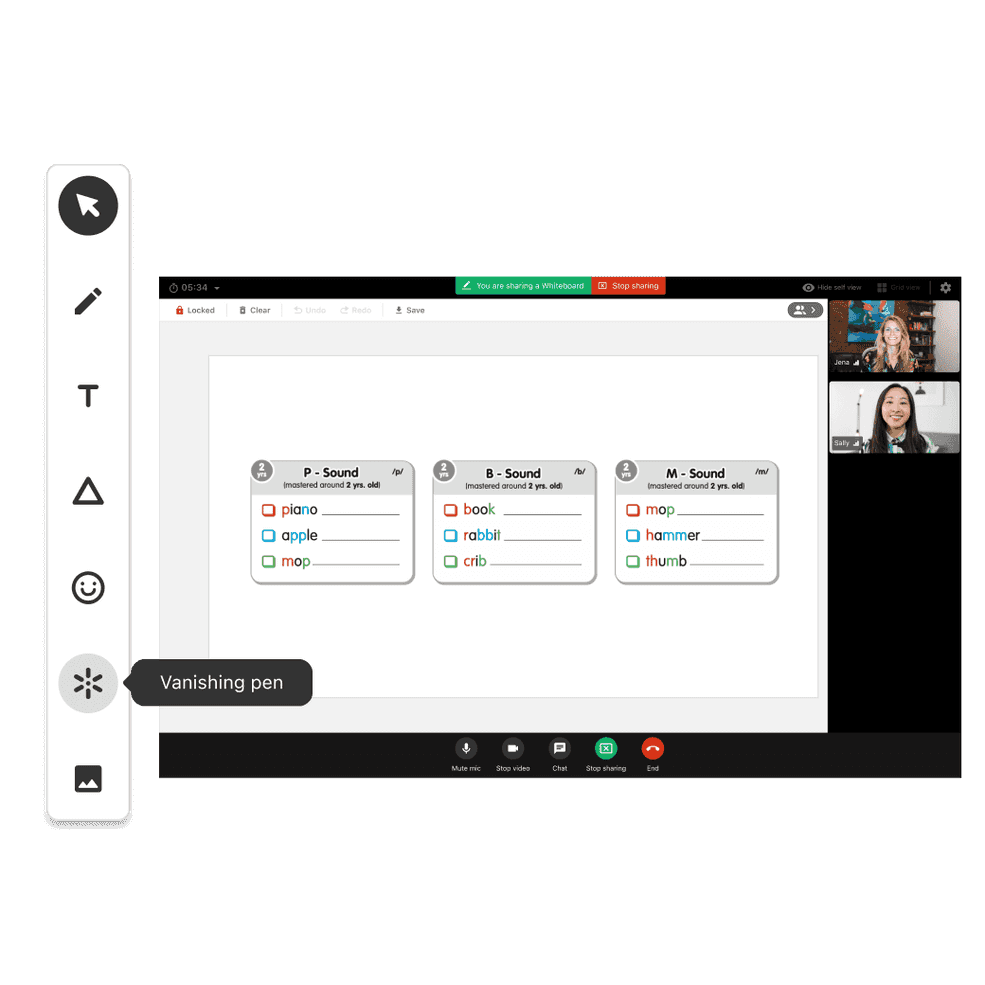
Whiteboard just became more interactive
Now you can use different draw tools, shapes, stickers, bullets, and more to improve client interaction during sessions with the latest enhancement for the telehealth whiteboard. You can even undo and redo!
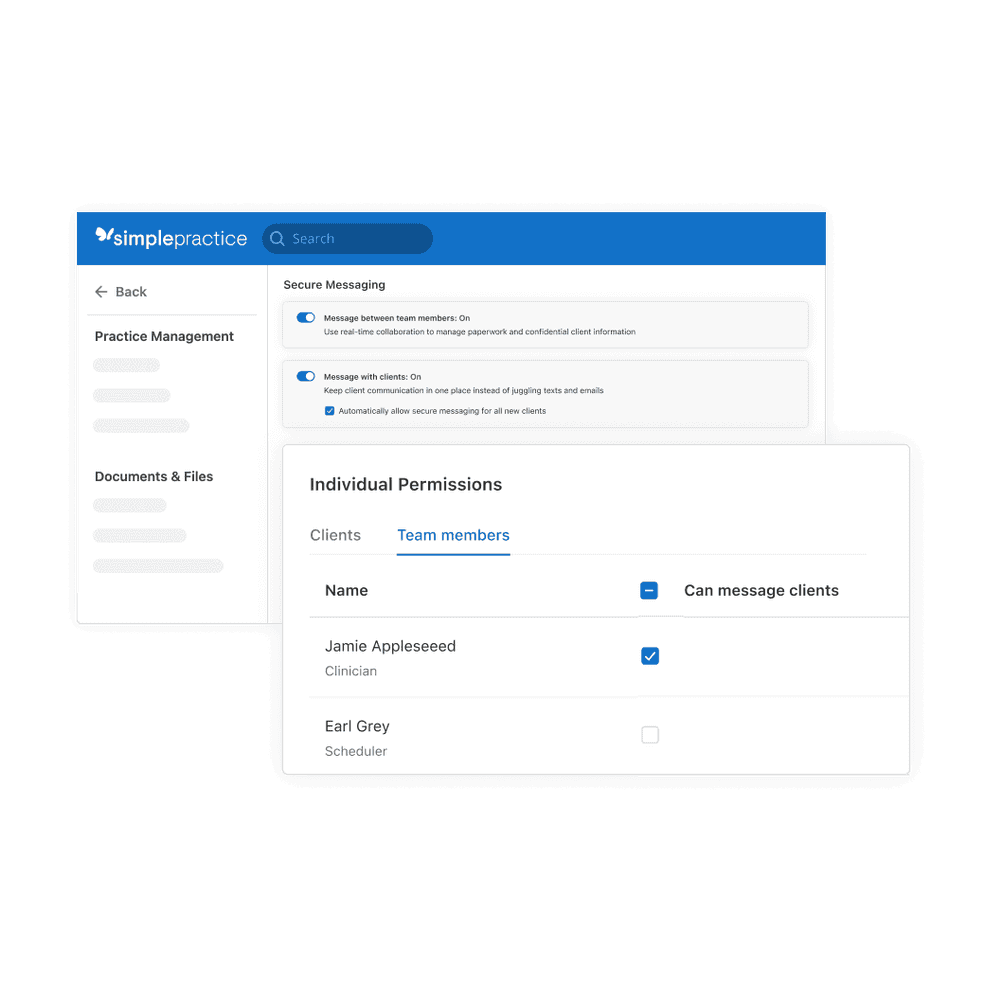
Allow billers and schedulers to send secure messages
Billers and schedulers can now send secure messages to clients from their SimplePractice account if the account owner grants them permission.
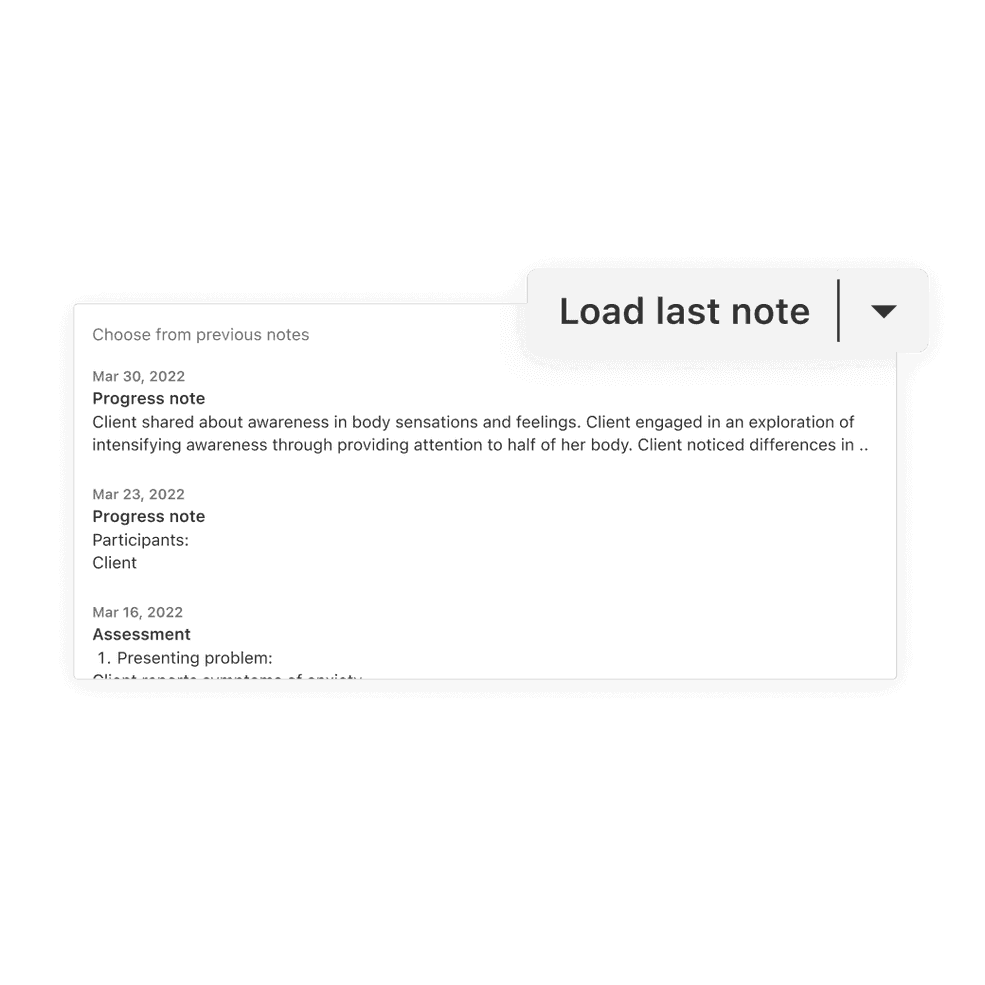
Choose which note to load
There’s now an option on the “Load Last Note” button that shows all of a client’s past progress notes. This allows you to choose which note you want to load—even if you wrote it months ago or if their last appointment was canceled.
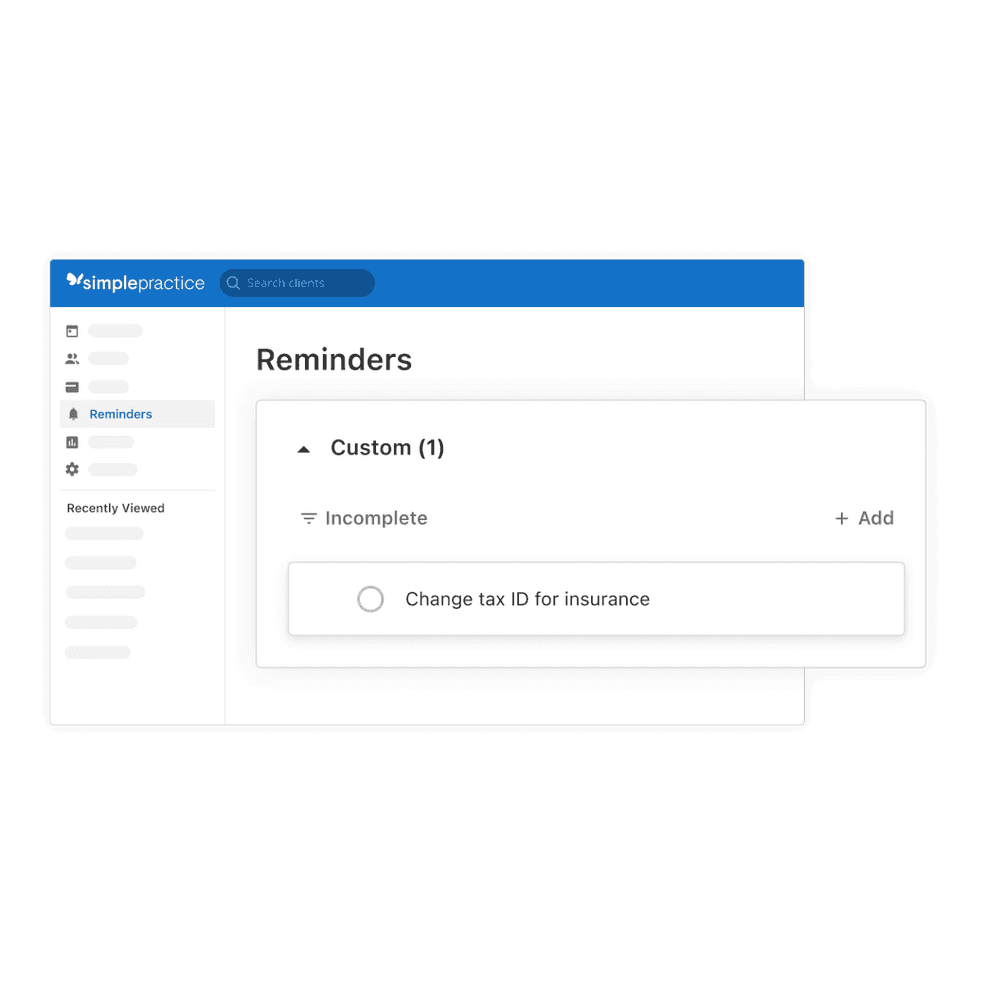
Create your own to-do list
You can now create your own HIPAA-compliant to-do lists directly in your SimplePractice account, so it’s easier to manage and remember your important tasks.
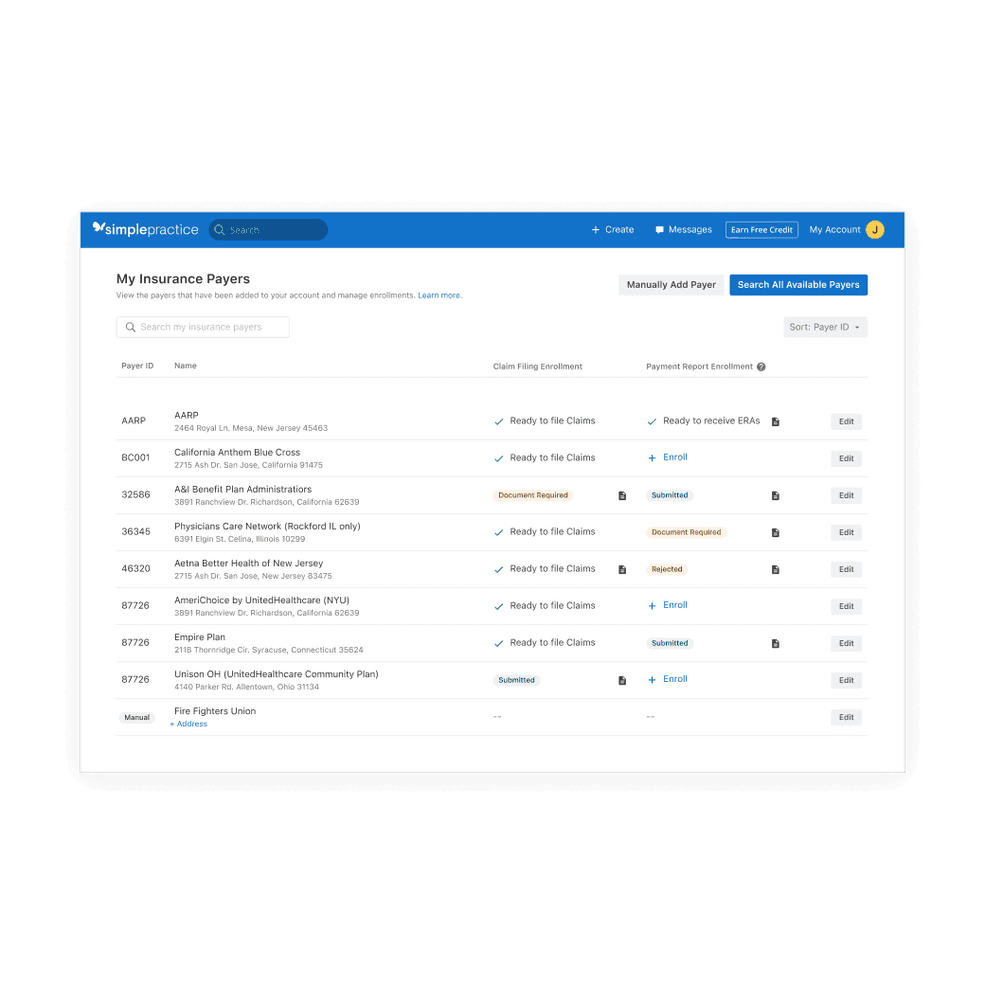
Reviewing enrollments just got simpler
The insurance page in Settings has a clean new look to make it easier for you to review your enrollments. Now you can quickly review and manage your insurance payers.
View full documentation history while writing notes
The new documentation history panel lets you see a client’s full clinical history without leaving your note. You can filter for past questionnaires, appointment notes, treatment plans, and more.
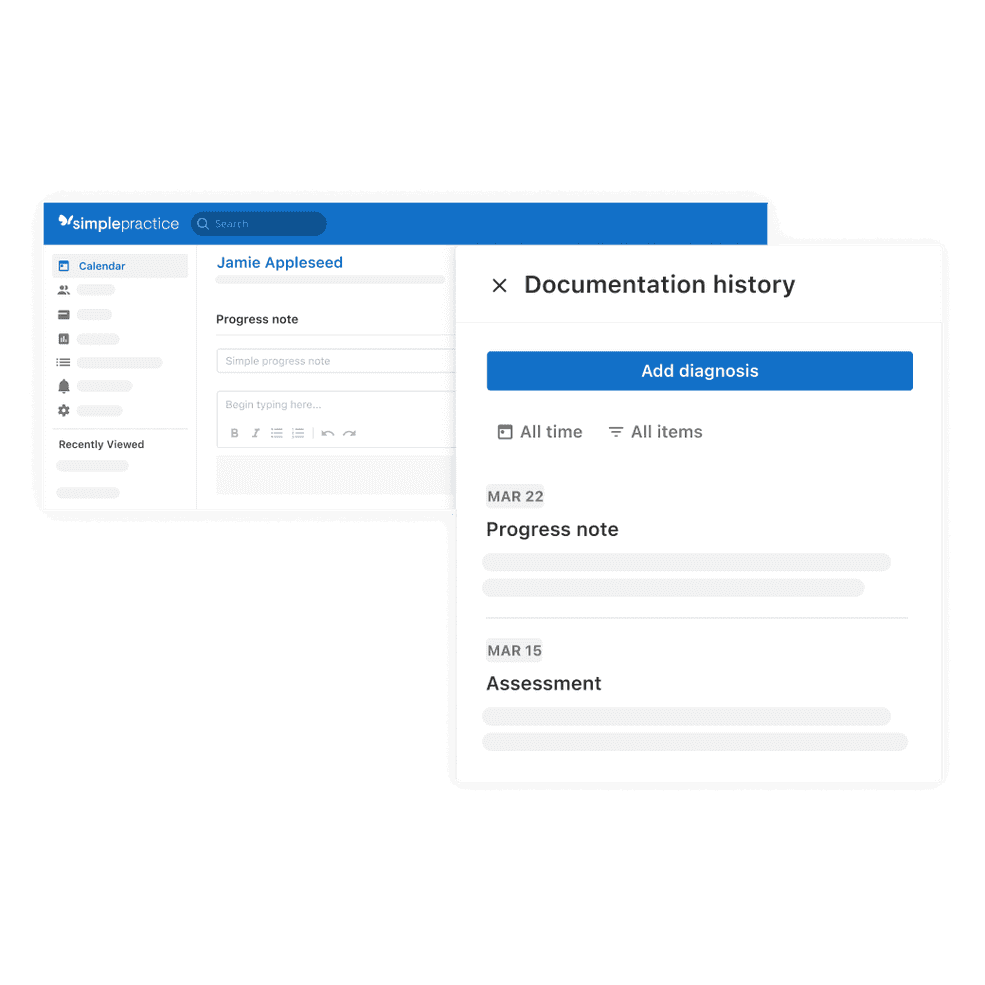
Multi-task with the new telehealth feature on iPad
Practitioners can now multi-task with telehealth and another app open at the same time.
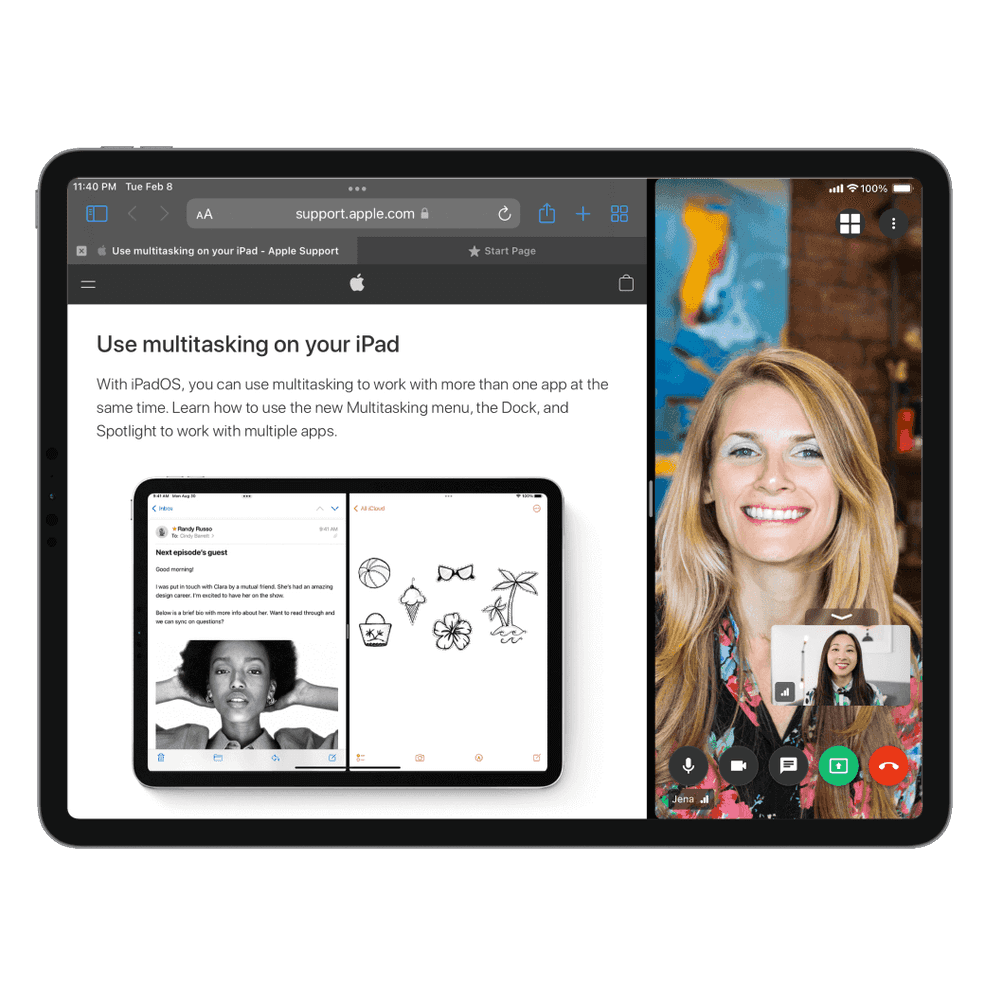
Turn secure messaging on for all new clients
You can now enable secure messaging by default for all new clients by selecting the checkbox under Settings > Secure Messaging page.
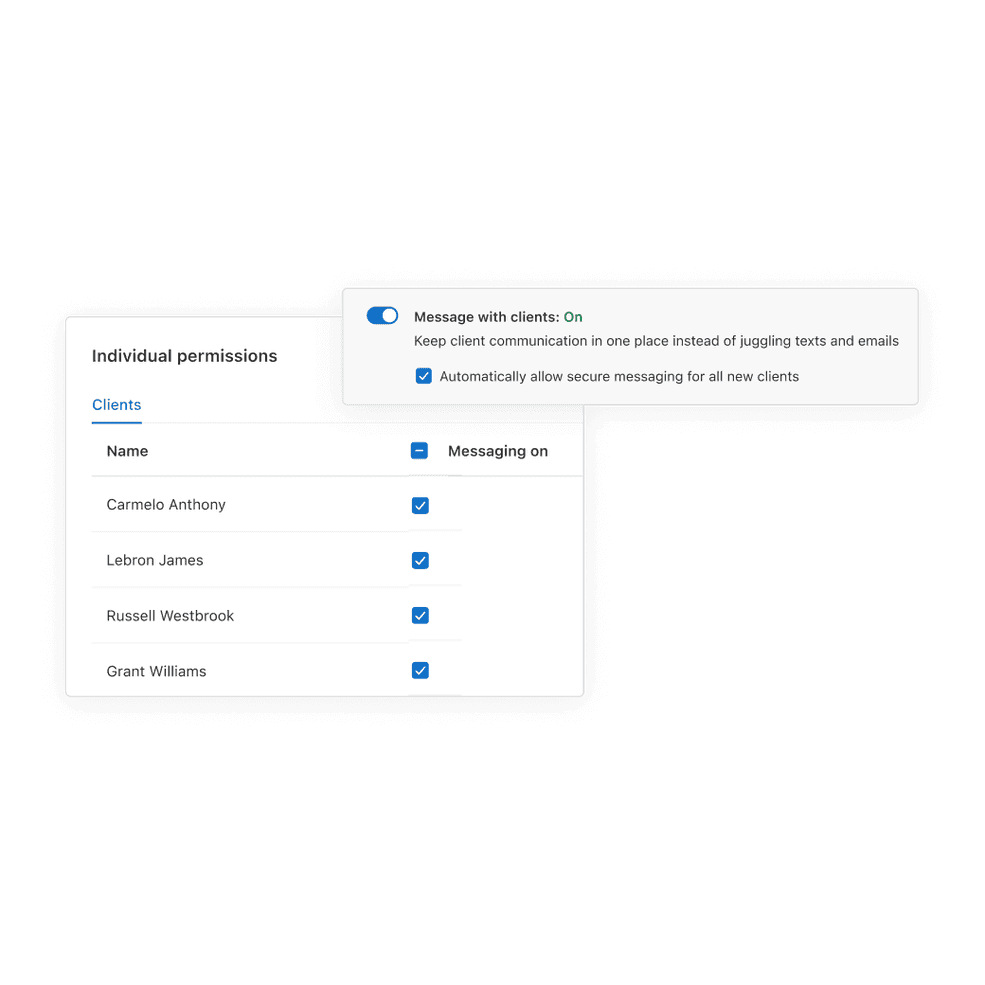
Know how your business is performing
You can now view the financial status and performance health of your practice under Analytics > Dashboard. At a glance, the dashboard shows your income, outstanding balances, appointments, notes, and claims for a selected time period.
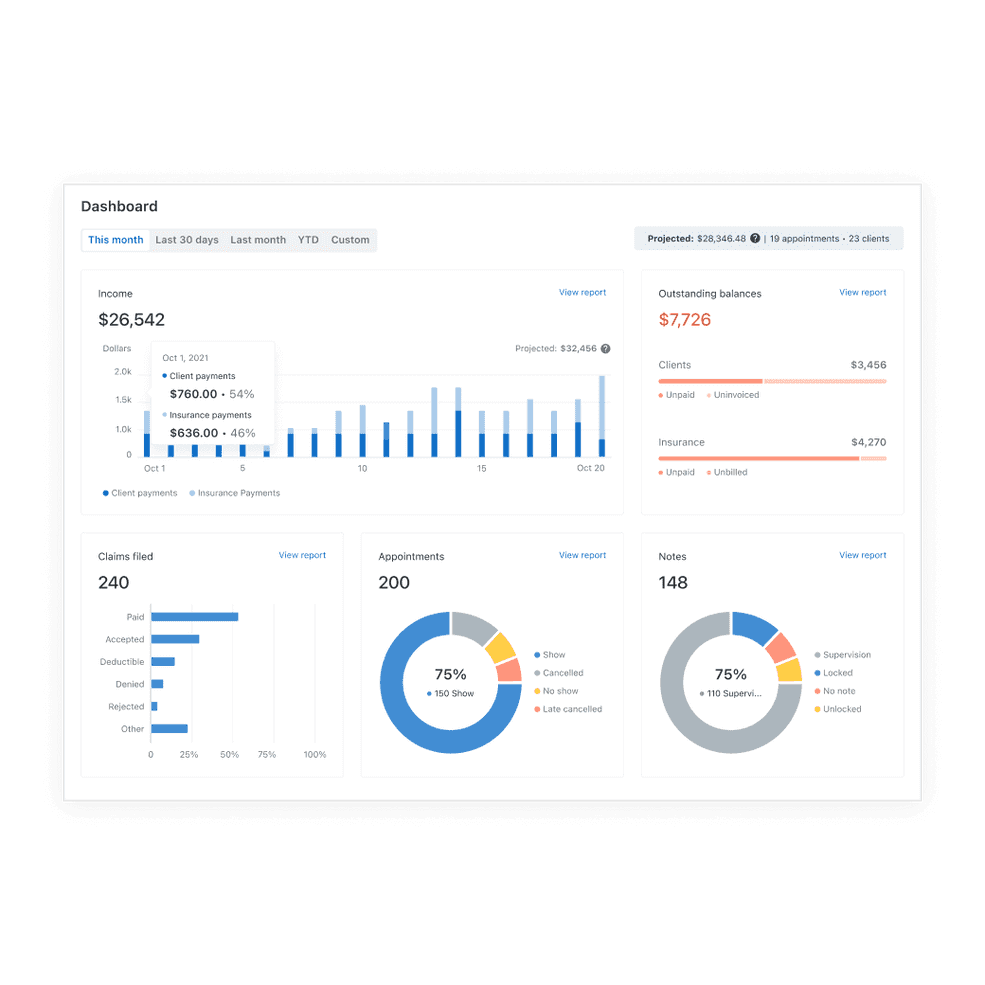
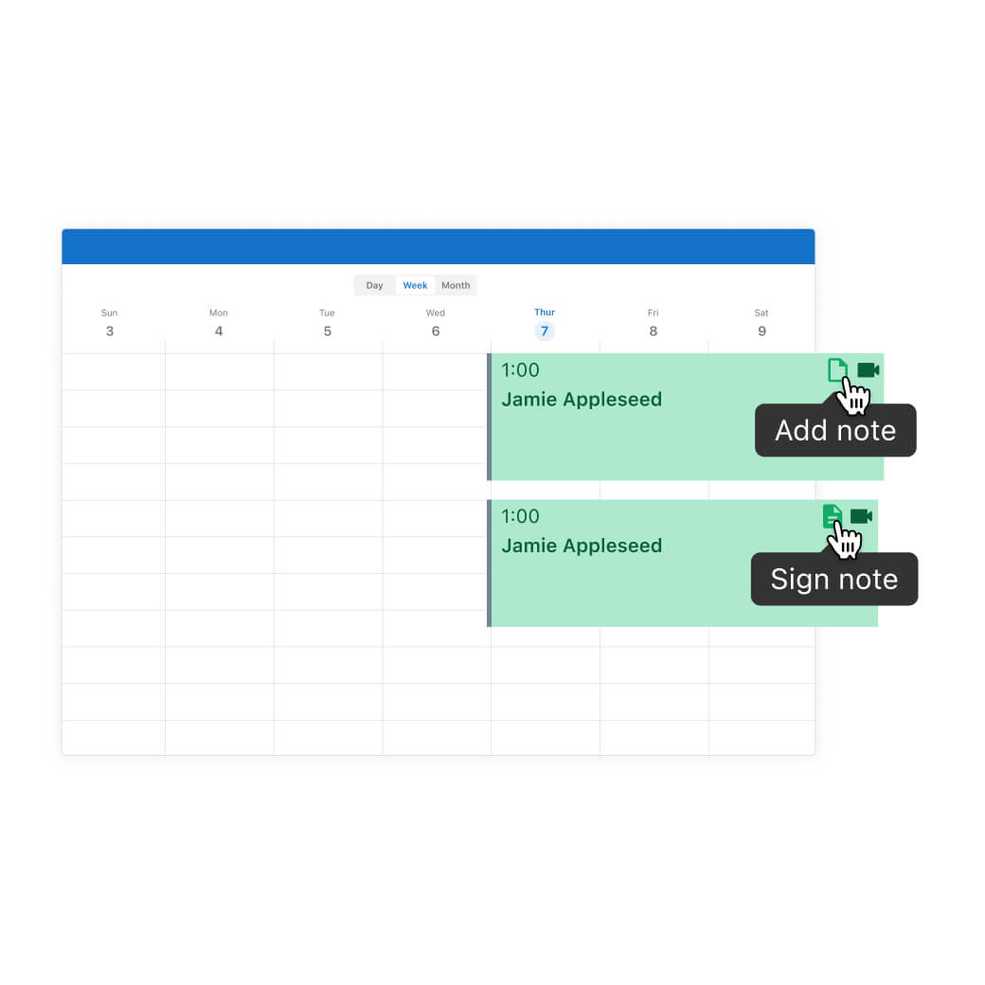
See the status of your progress note at a glance
New icons on your appointments will make it easy for you to identify which clients still have documentation that needs to be completed, locked, and signed. Now you can clearly see if you’re missing notes or signatures.
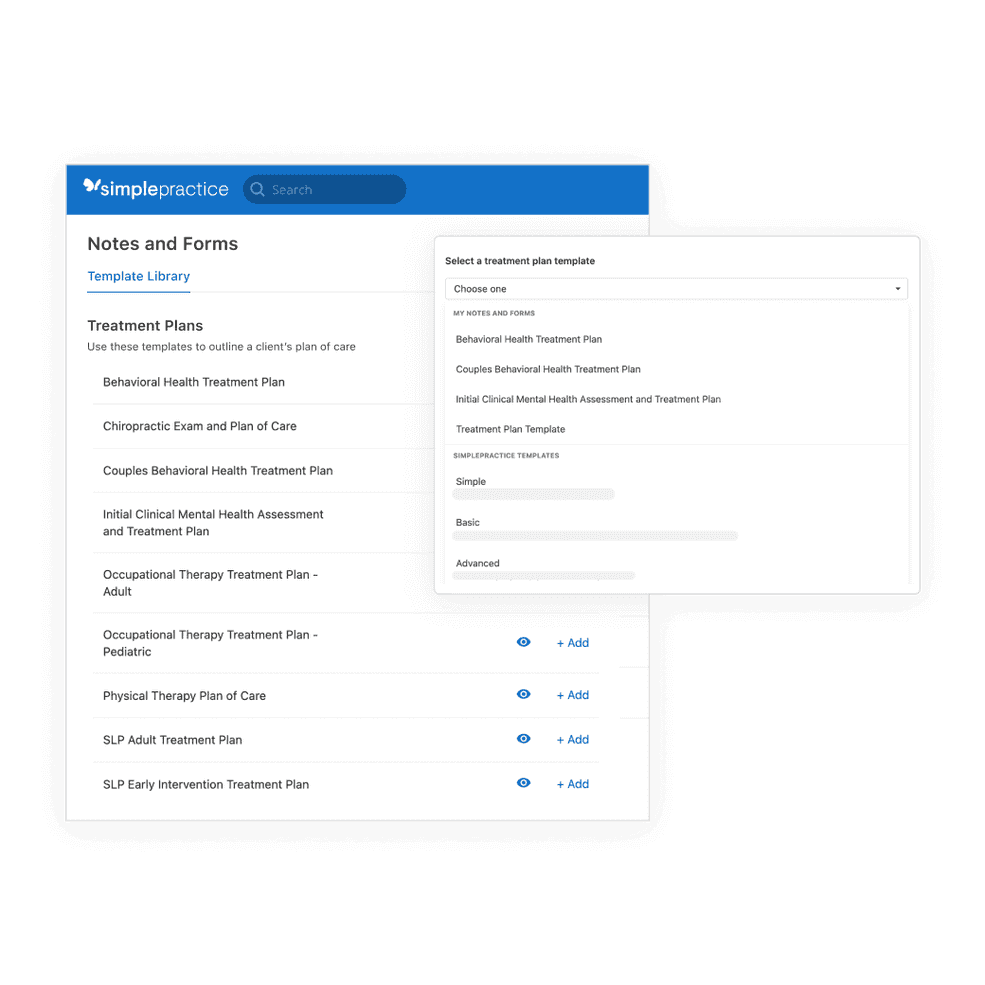
An easier way to do treatment plans
You can now create custom templates for all your treatment plans. Easily edit to meet insurance payer requirements and compliance standards. Create unique templates to use with specific presenting problems or treatment modalities.
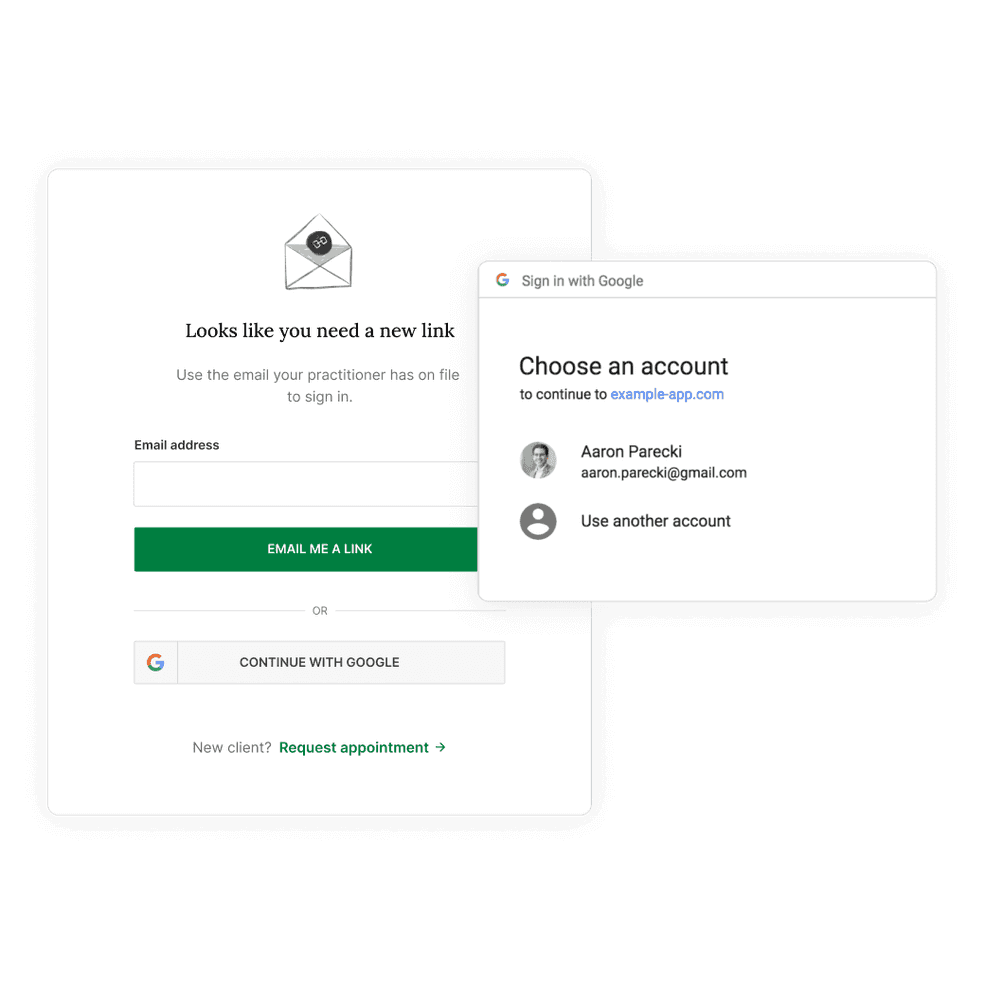
Clients will have option to securely sign in with Google
Clients and contacts who have a Gmail address linked to their Client Portal will have the option to securely sign in with their Google account.
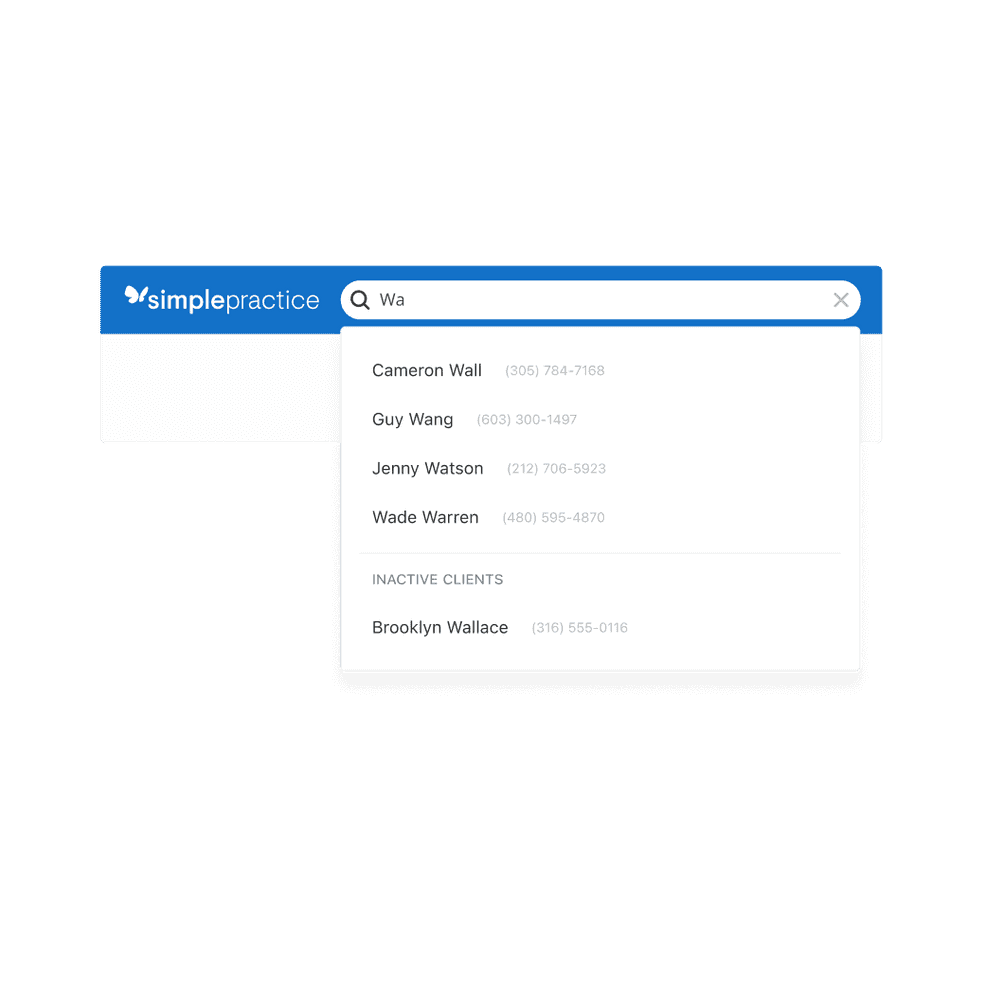
An easier way to find clients
You can now search for clients and contacts by phone number. Search results will display phone numbers for both active and inactive clients, couples, and contacts of minors.
View all your clients’ details in one place
You can now view a report of all your clients’ details, as well as filter and export the report. Details include their current contact information, if the client is active or inactive, insurance provider, if relevant, and more.
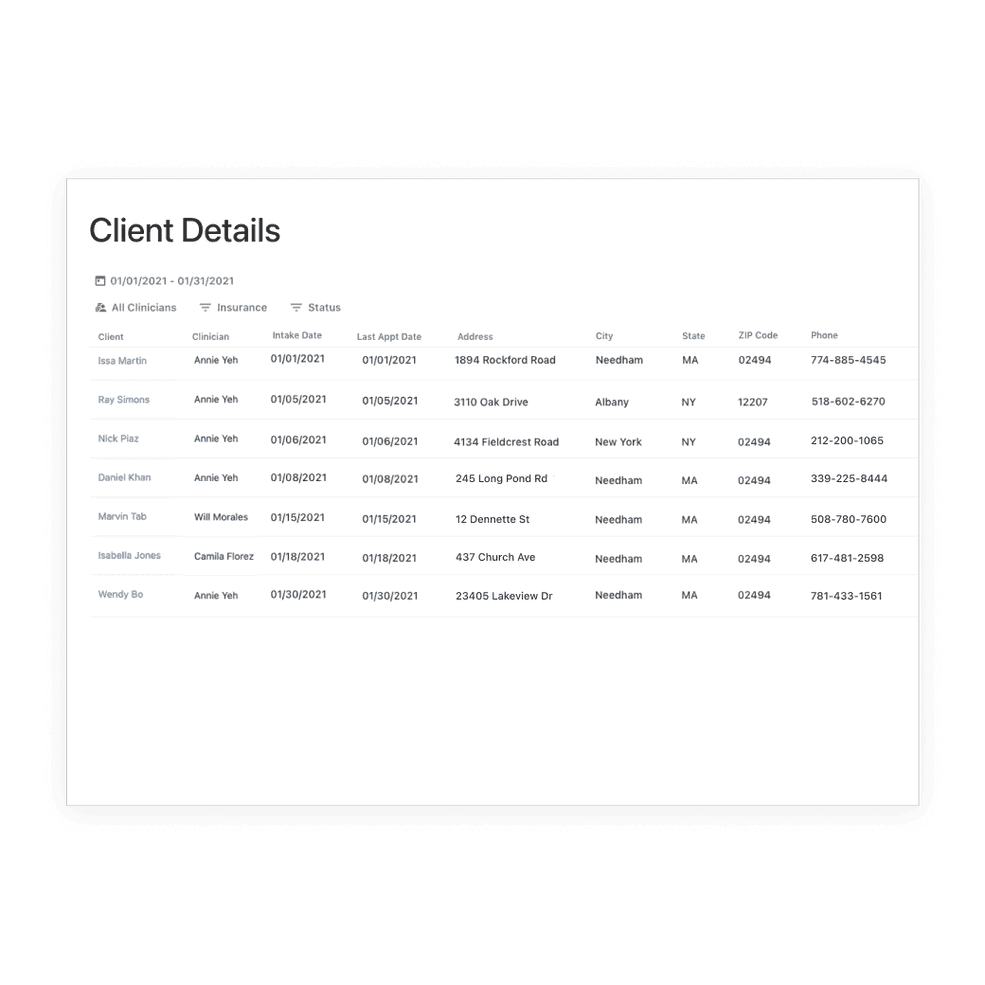
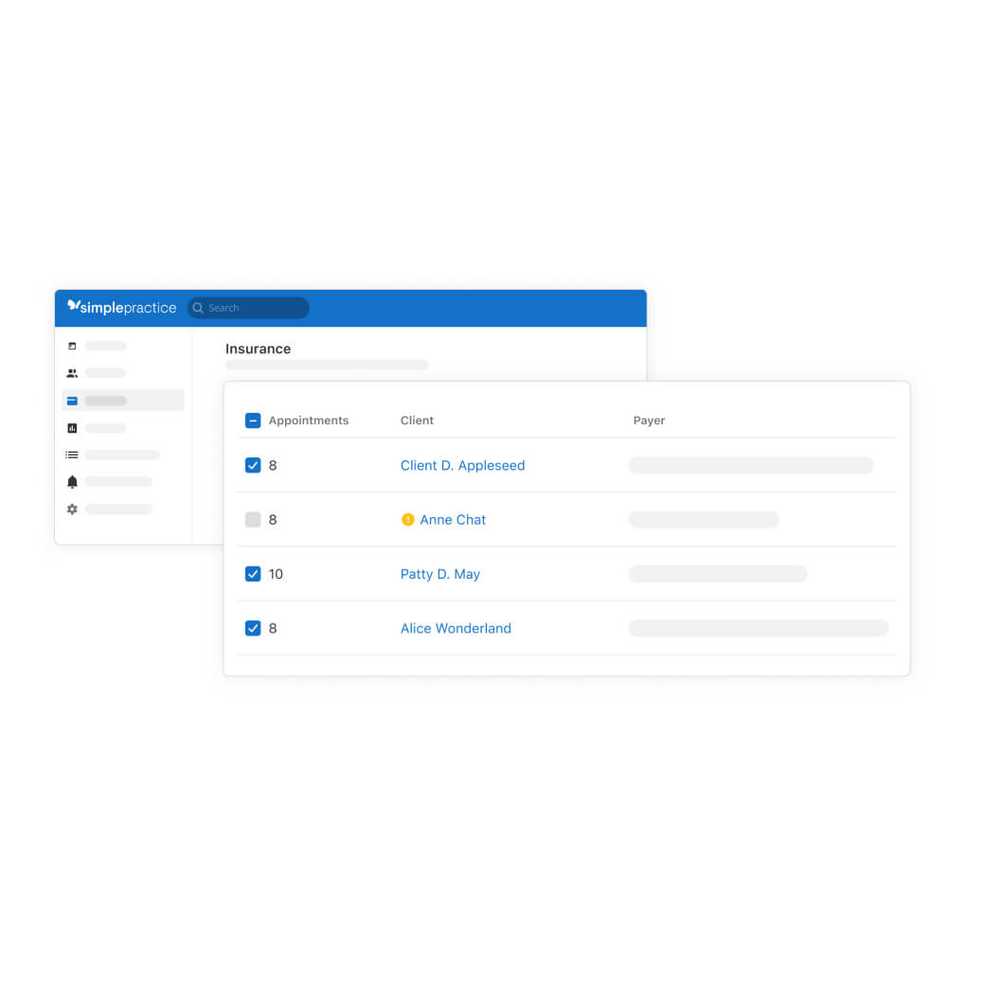
Easily access everything you need for batch claims
You can now see the status of your notes, modifiers, and place of service before you create batch claims.
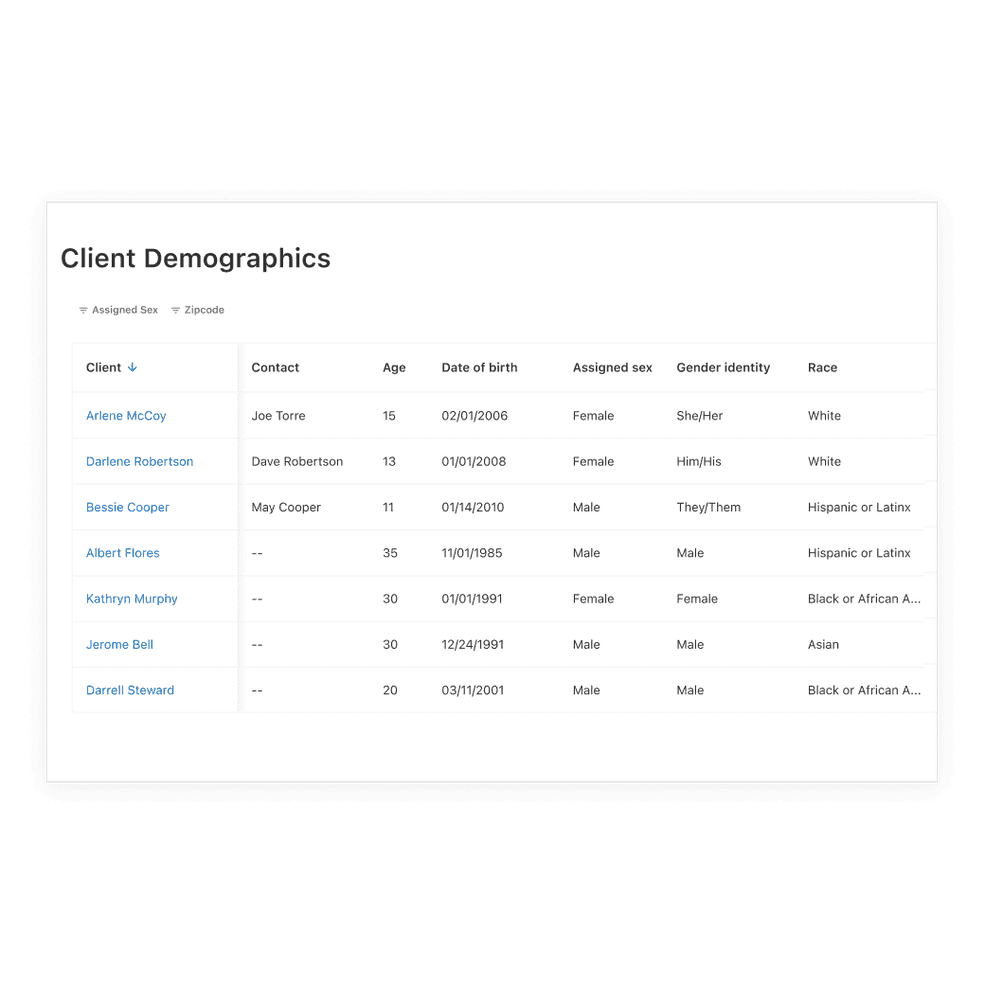
View your client demographics
You can now view your client demographics in a clear, easy-to-read table. Simply head to Analytics, select Reports, and view or export your client demographic details.
Limit your total number of appointments each day
Have full control over your schedule by setting a max number of appointments each day. After the limit has been reached, clients will not be able to request an appointment for that day.
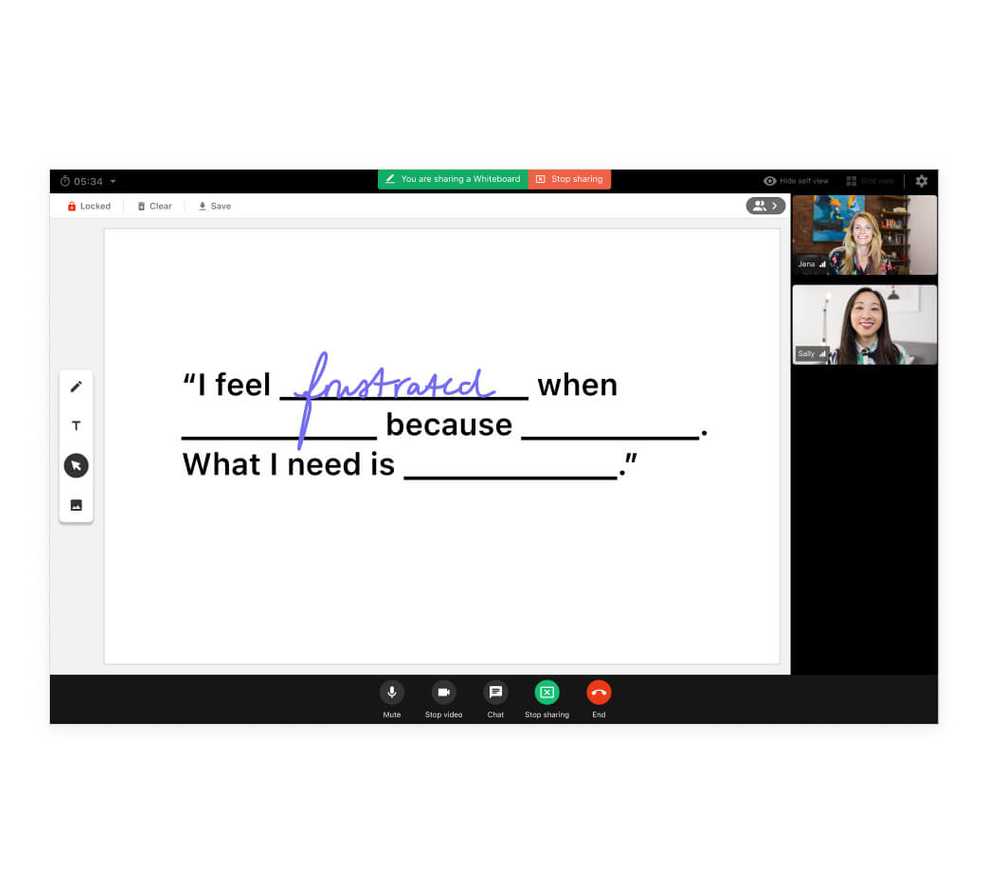
Introducing the whiteboard feature
The whiteboard feature makes it easy for you and your clients to interact and collaborate. Draw, type, and insert images in real-time. Plus, you can start or stop the whiteboard at any time right from your telehealth calls.
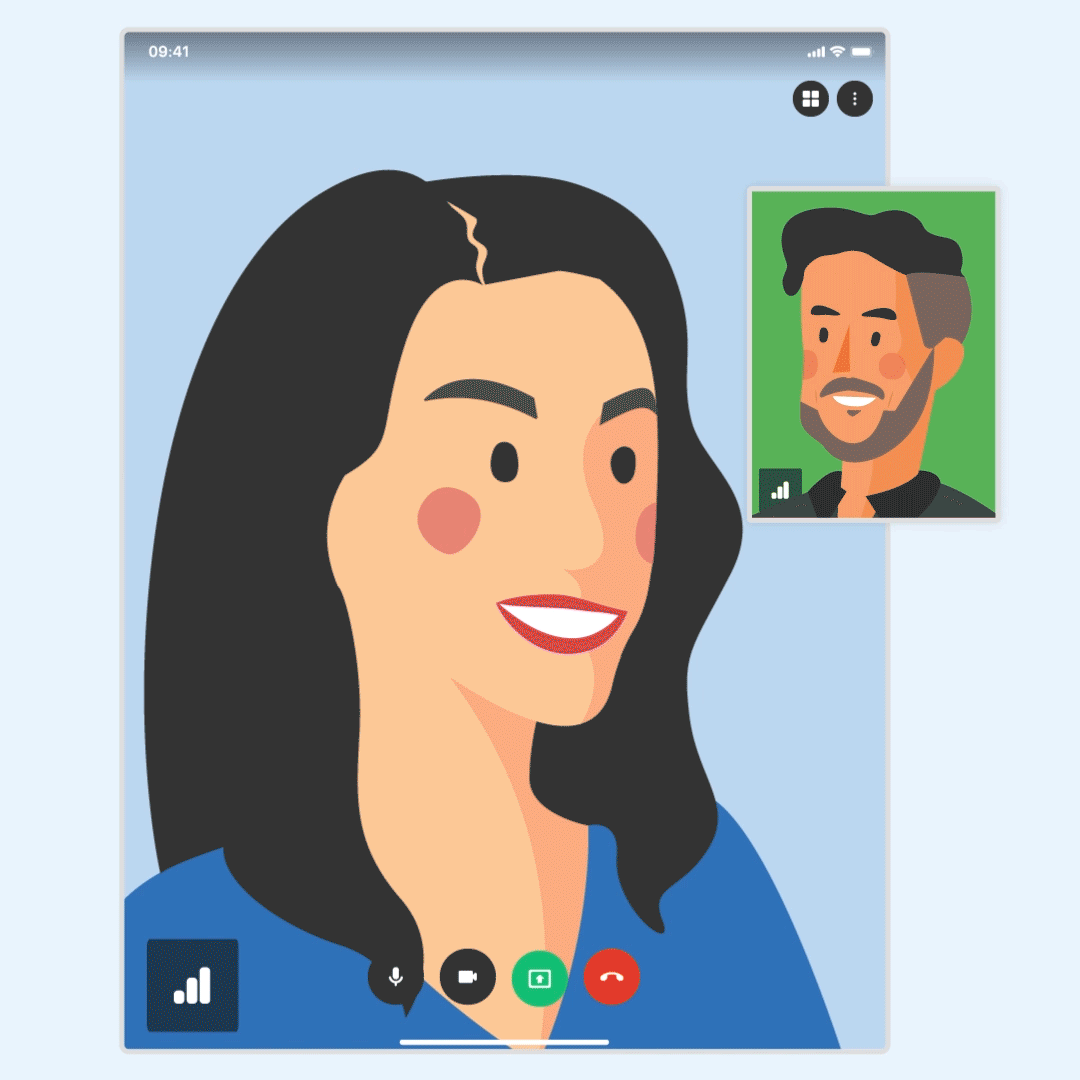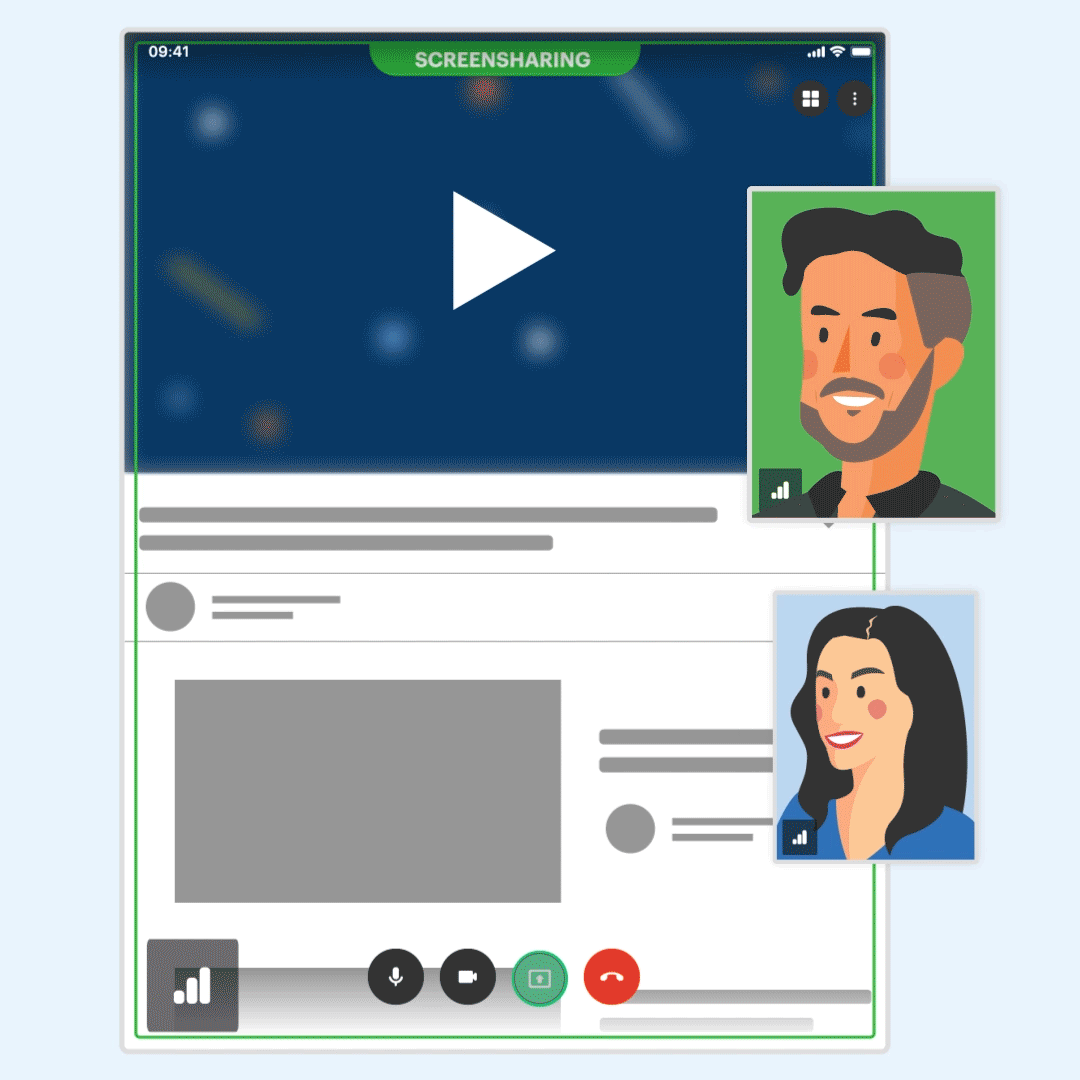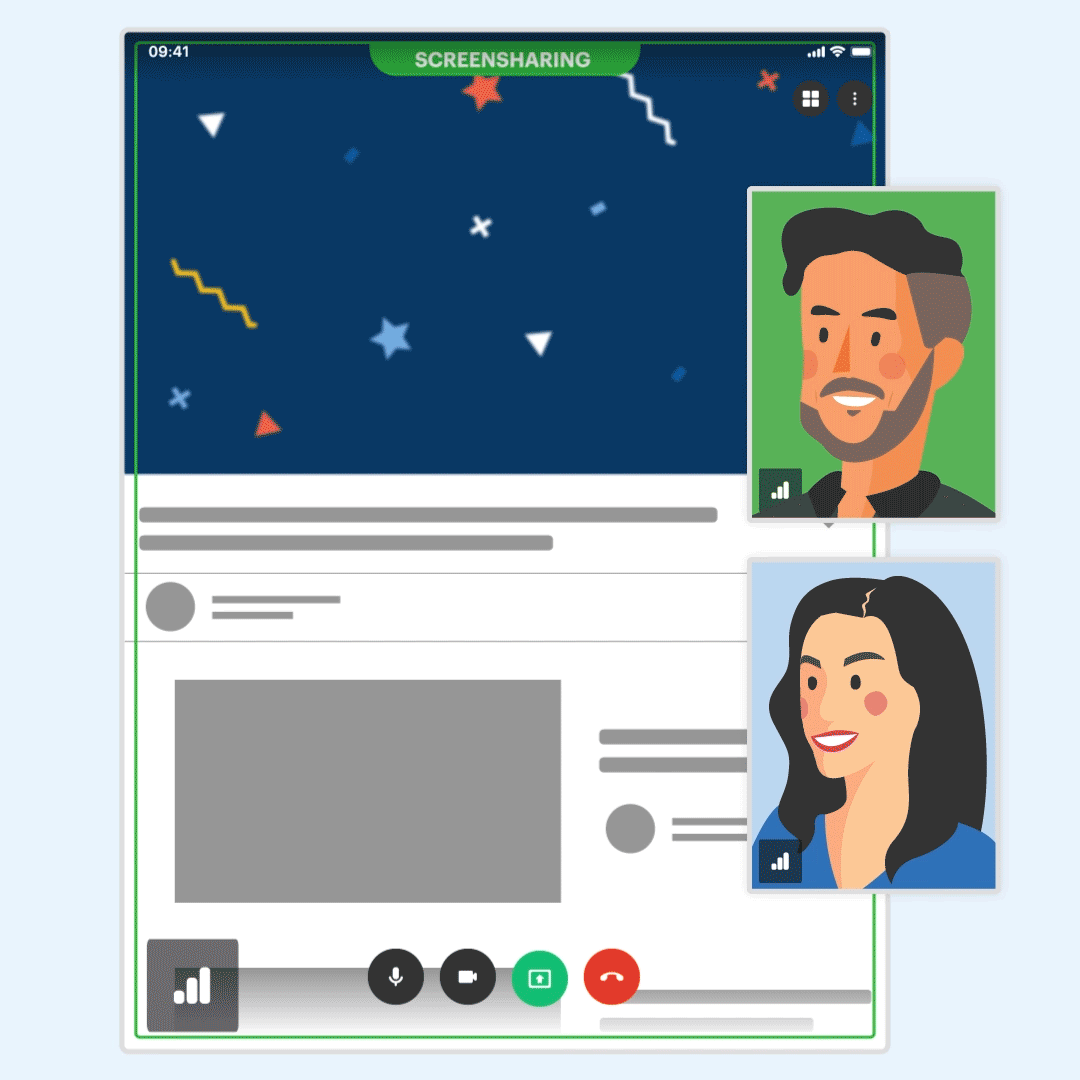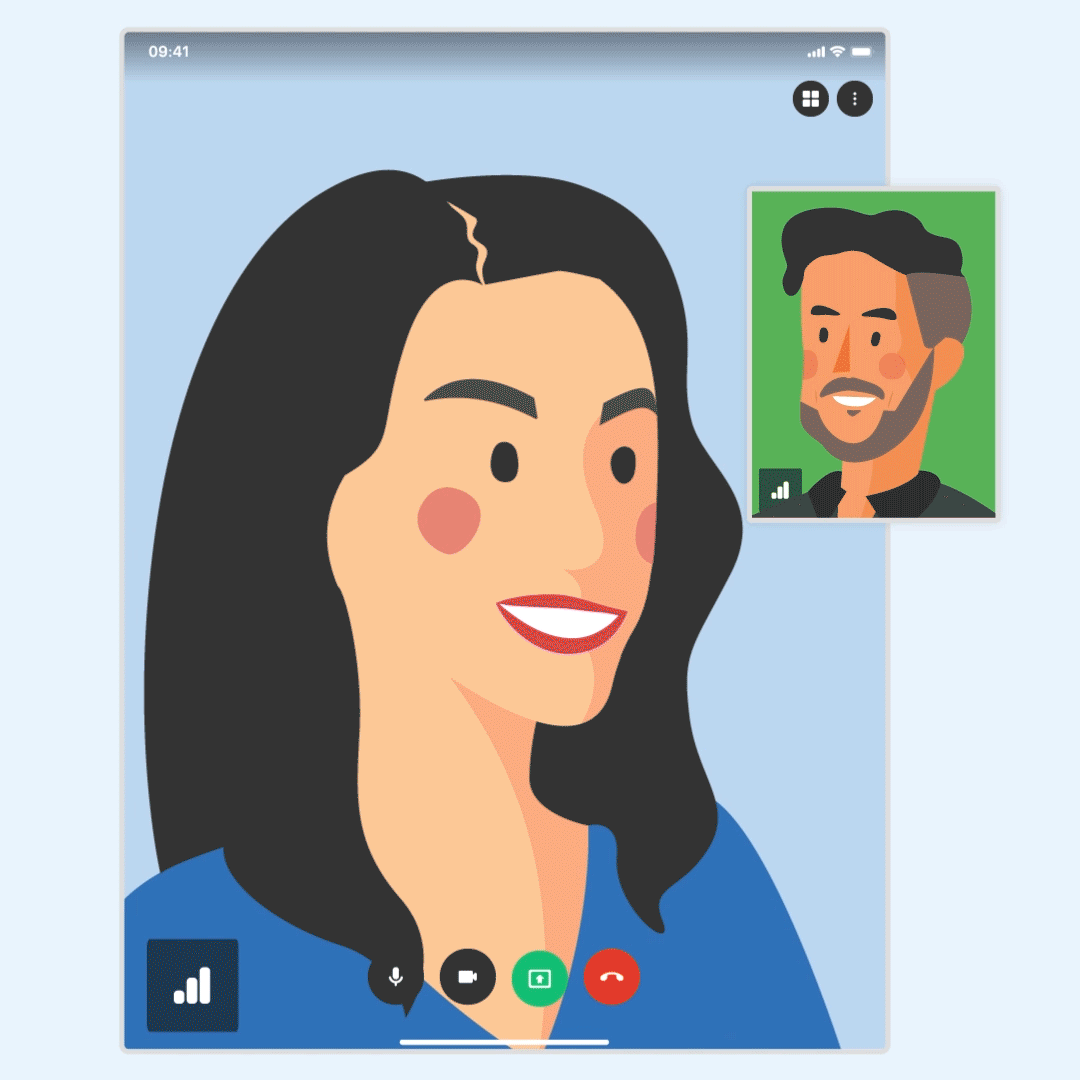
New! Screen-share on iPad
You can now share your screen with audio when conducting telehealth appointments from your iPad. Easily access this feature during your sessions and increase client engagement by sharing games, worksheets, and more.
Improved communication for pending appointment requests
New appointment requests are now part of the daily morning agenda email so you can view, accept, or decline them all without opening your SimplePractice account.
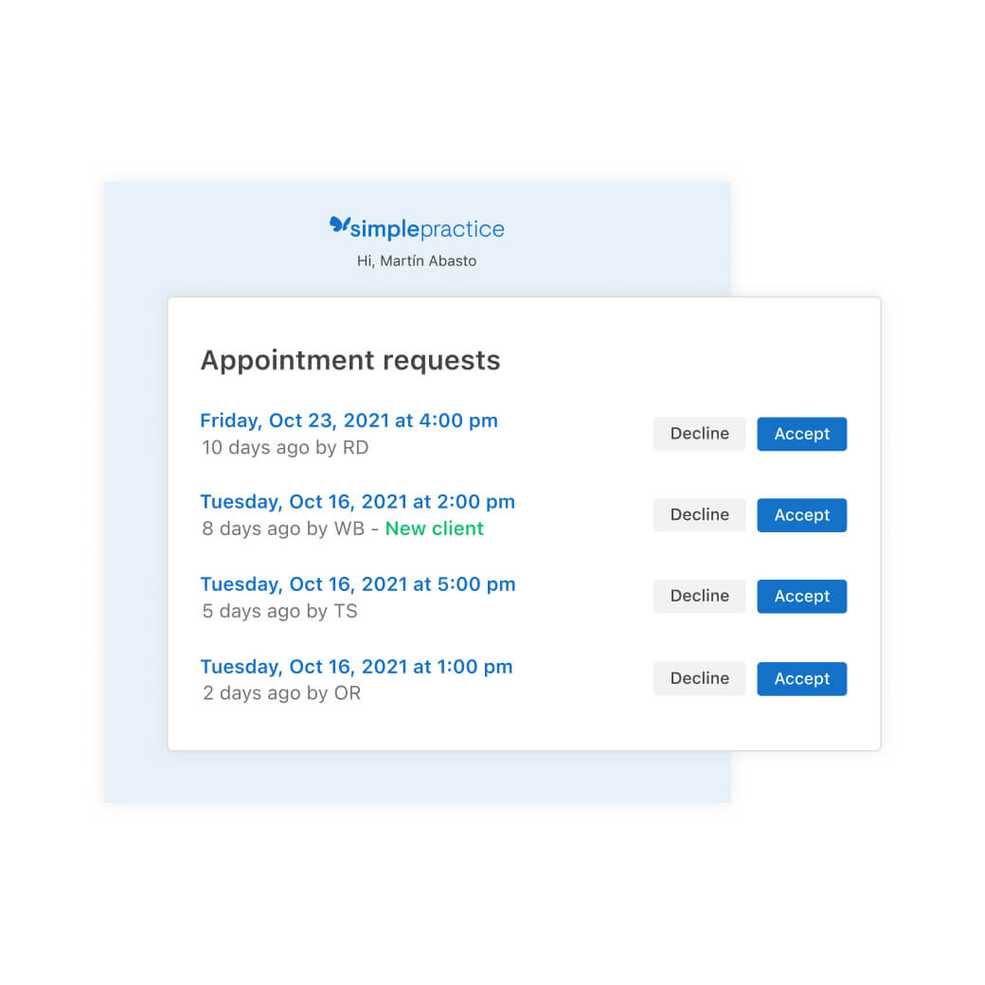
Clients can update their credit card in the Client Portal
Clients can now view saved credit cards, add new ones, and choose which card they want as the default payment method in the Client Portal. All you have to do is enable access billing documents in each of their Client Portal settings.
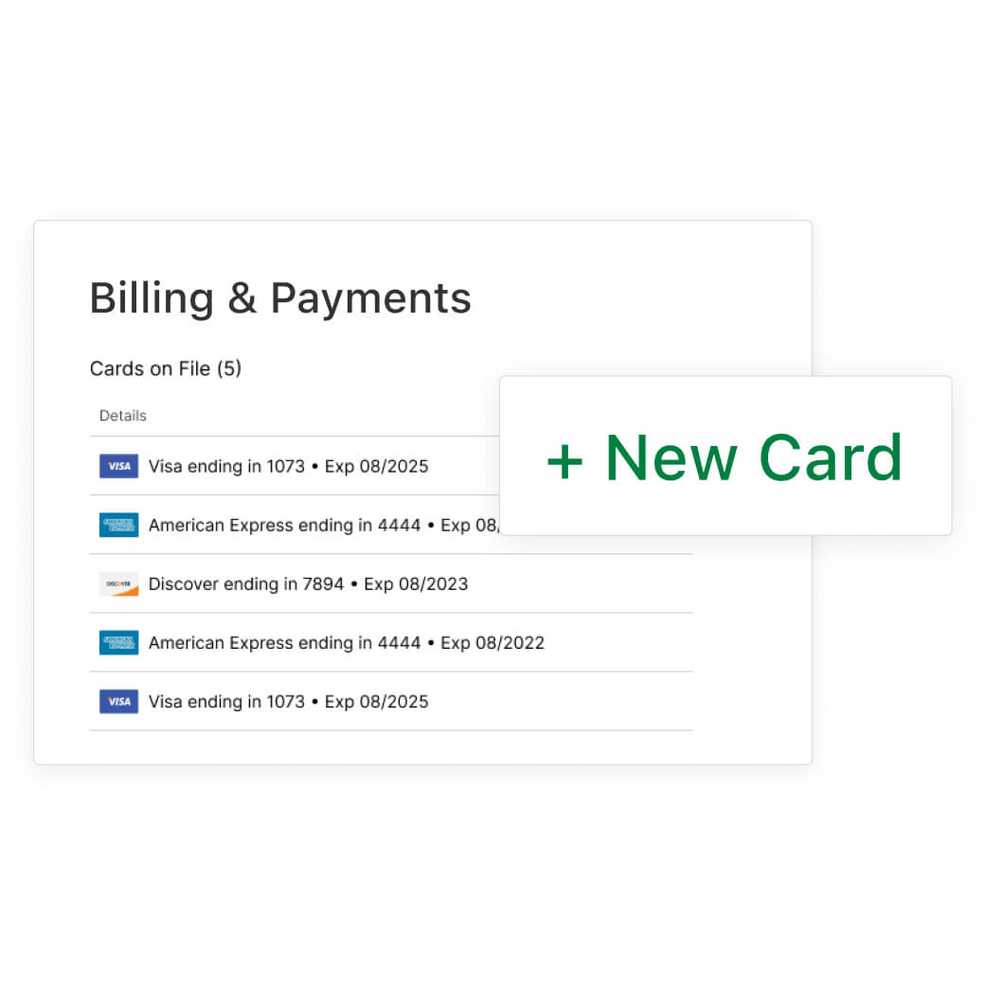
Signing made simple
Collecting client signatures just got easier. Now you can request them directly in the Client Portal so clients (or guardians or contacts) can review and sign shared documents like progress notes and treatment plans.
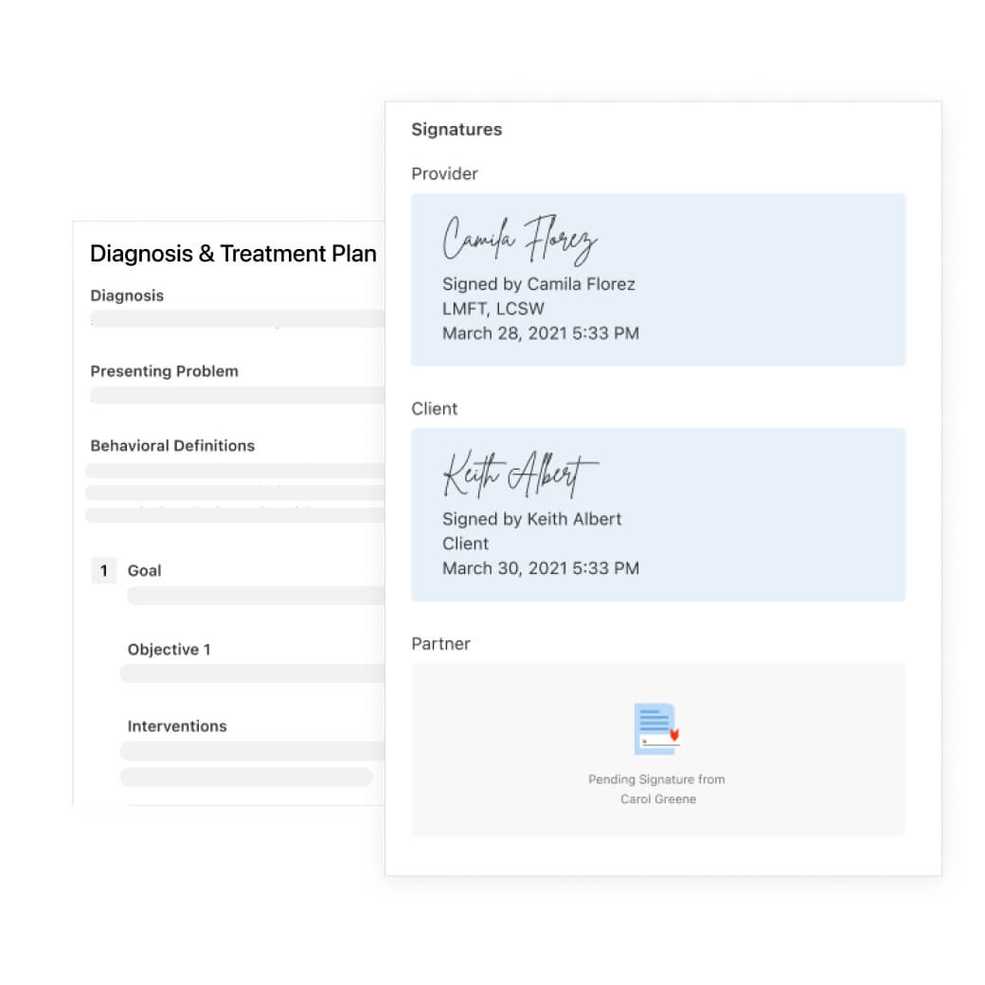
Your 2021 tax report is now available
You can now download your 2021 tax report. Head to Reports, then Income and find your 2021 Tax Report. Once it’s ready to download, you can find it in the Data Export section of your account settings.
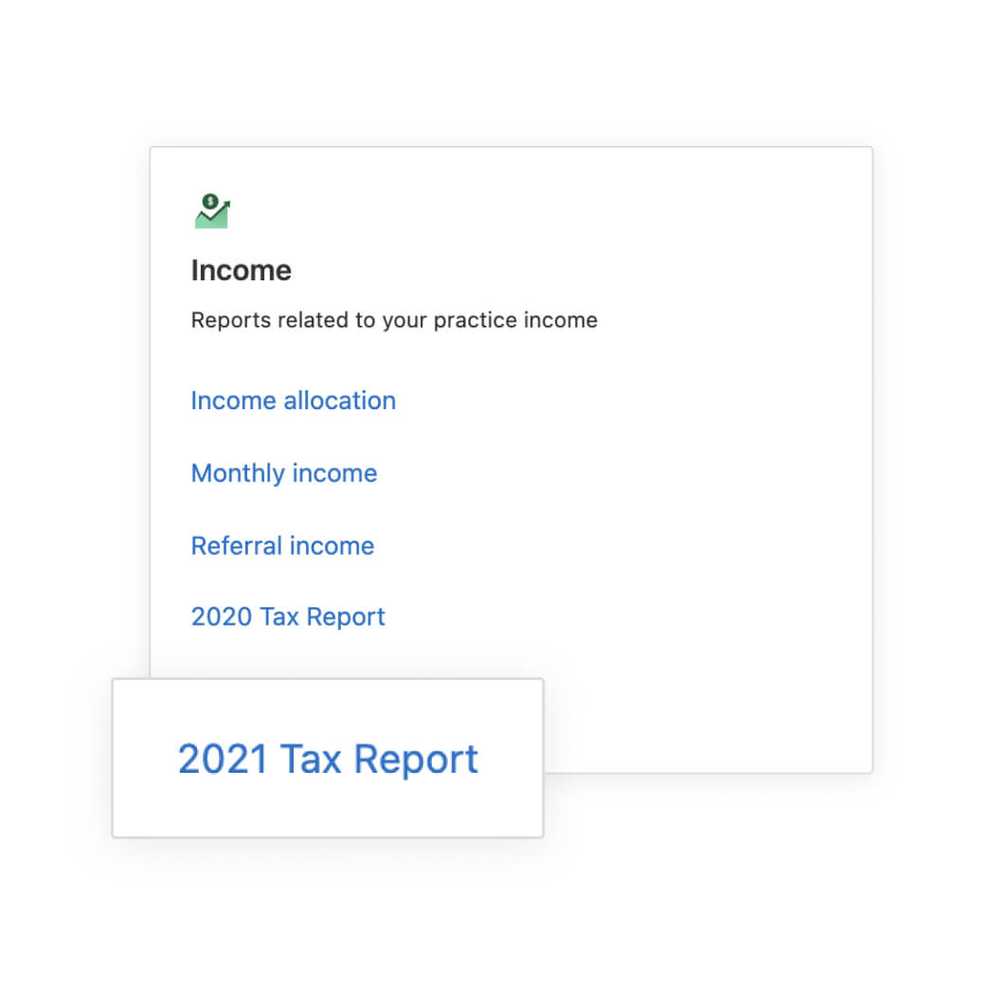
Virtual backgrounds for telehealth
You—or your clients—can now choose from 9 different virtual telehealth backgrounds. Currently available via the web browser.
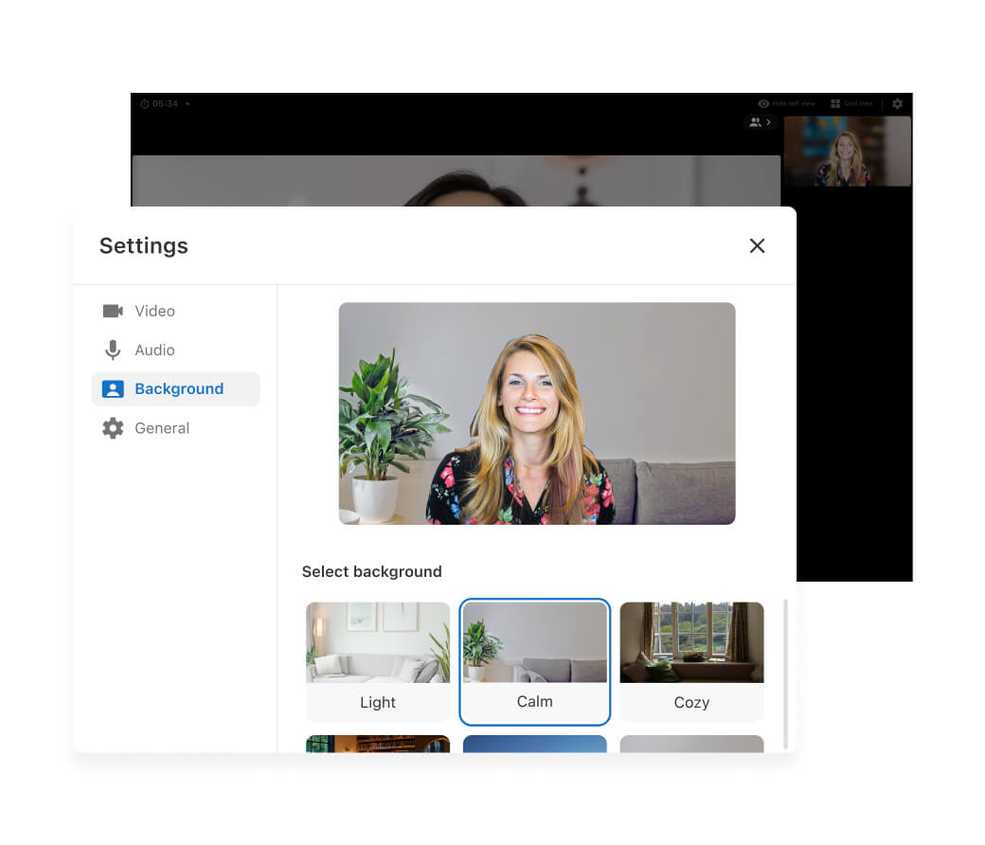
Blurred background for telehealth
You can now blur your background during telehealth calls. It’s available for all participants on the telehealth call and is currently supported via your web browser*. (May be limited on certain browsers.)
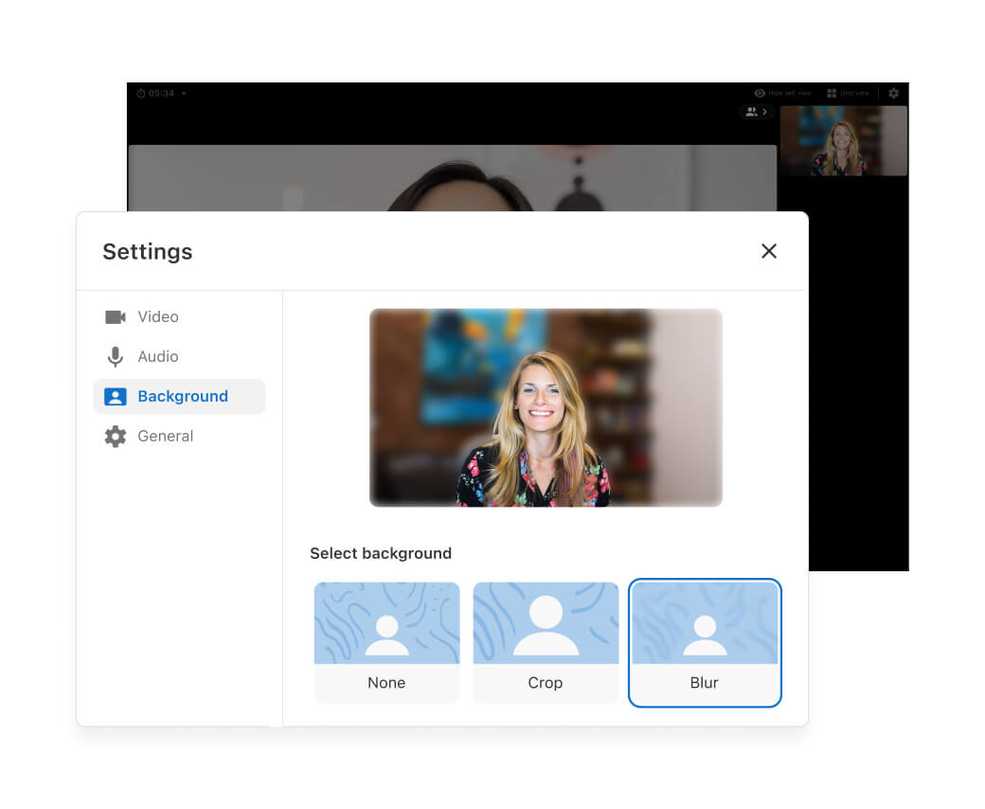
Telehealth now has a chat feature
Practitioners can now send a chat message to all participants during a Telehealth appointment for added convenience, real-time troubleshooting, as well as sharing materials with their clients.
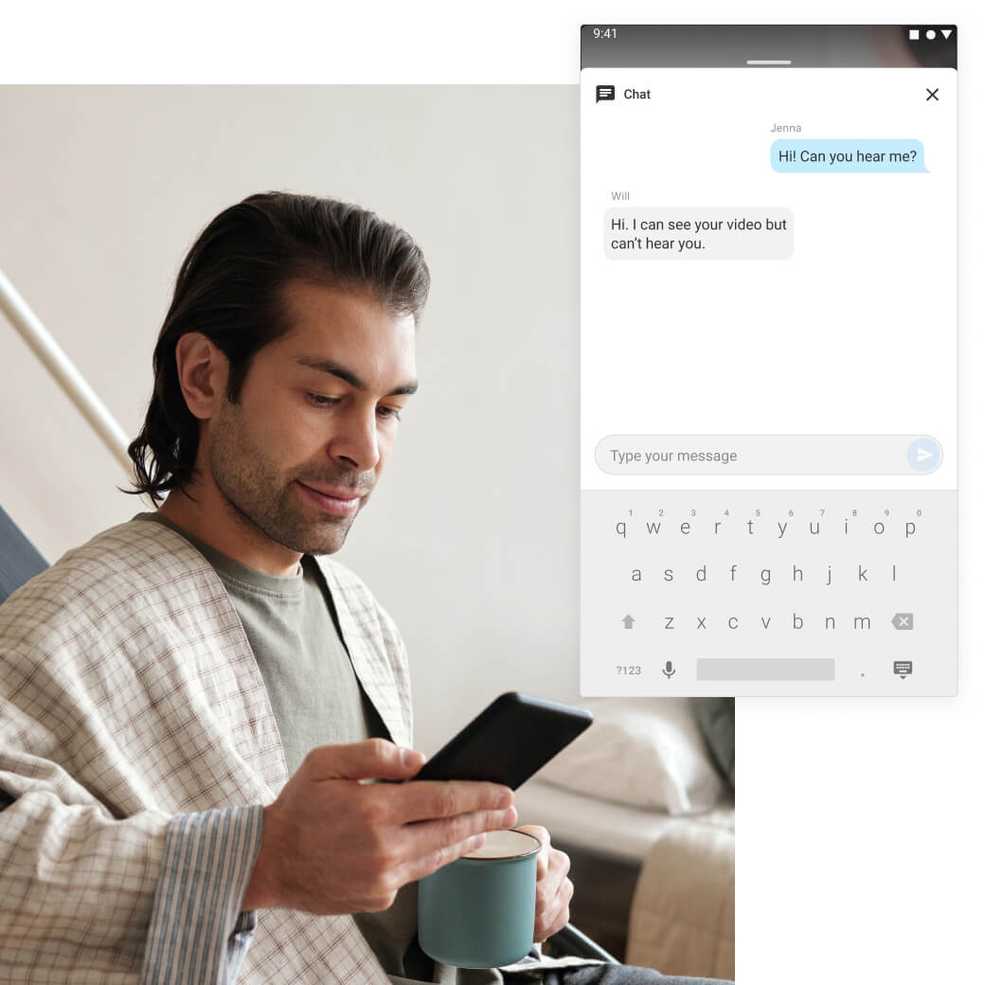
A new way to remind clients to complete paperwork
Save time by turning on automatic email reminders for clients and contacts to complete their paperwork before their appointments.
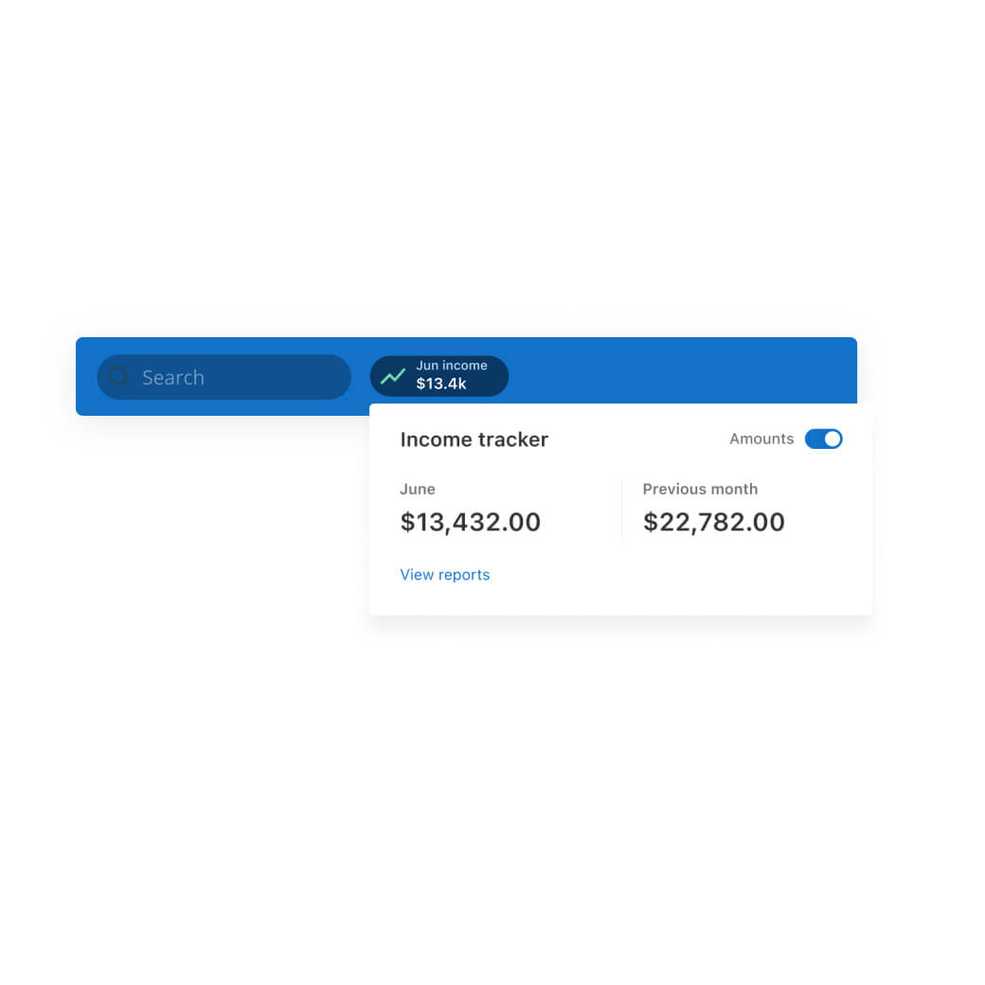
Introducing an income tracker
The new income tracker on the top navigation bar makes it easy to view your current and previous month’s income, and it links to the reports page for more detail. You can also choose whether to display or hide this feature.
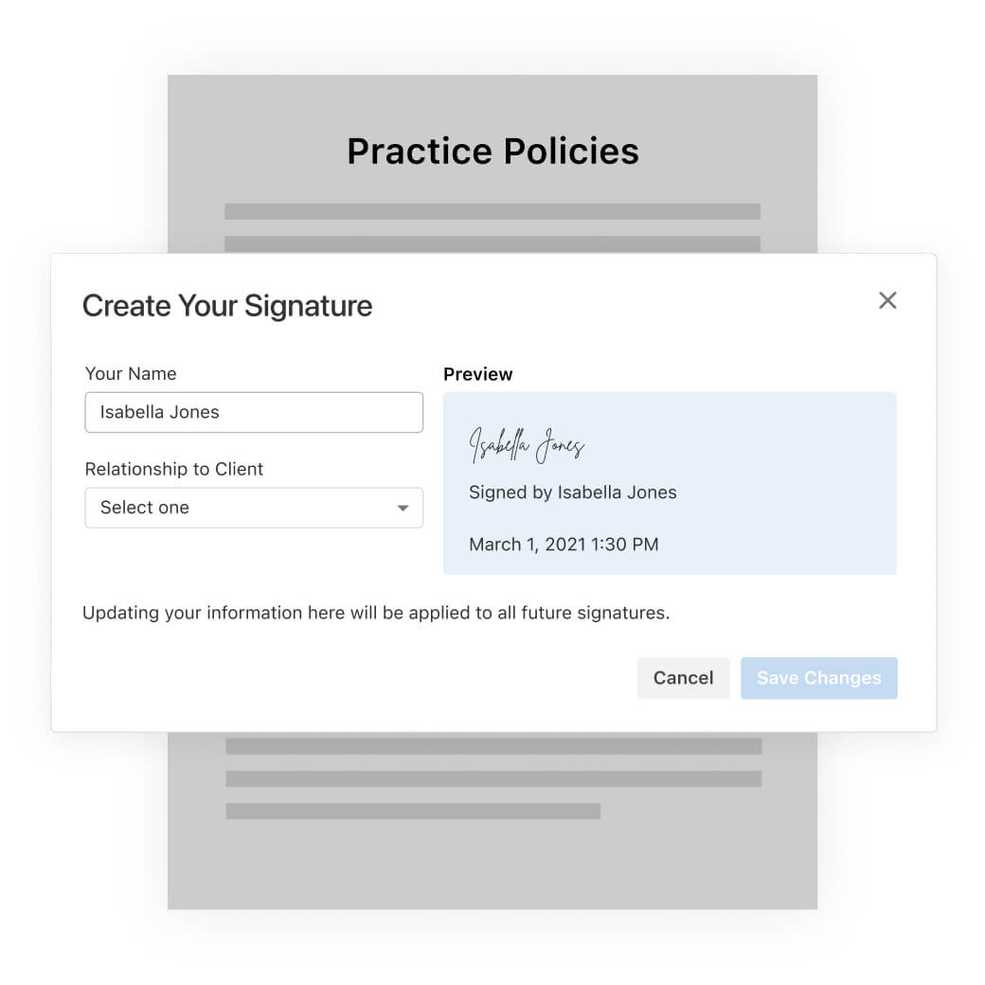
Update to client signatures in the Client Portal
Clients can now type their name to sign documentation—which will be remembered and auto-populated for subsequent signatures. The client’s signature will look the same every time and signers can choose their relationship to the client.
A fresh new look for clients
Your client’s experience now has a fresh, more modern appearance. Everything will have a cohesive look and feel—from the client portal to the emails they receive. No functionality has changed, and no action is required.
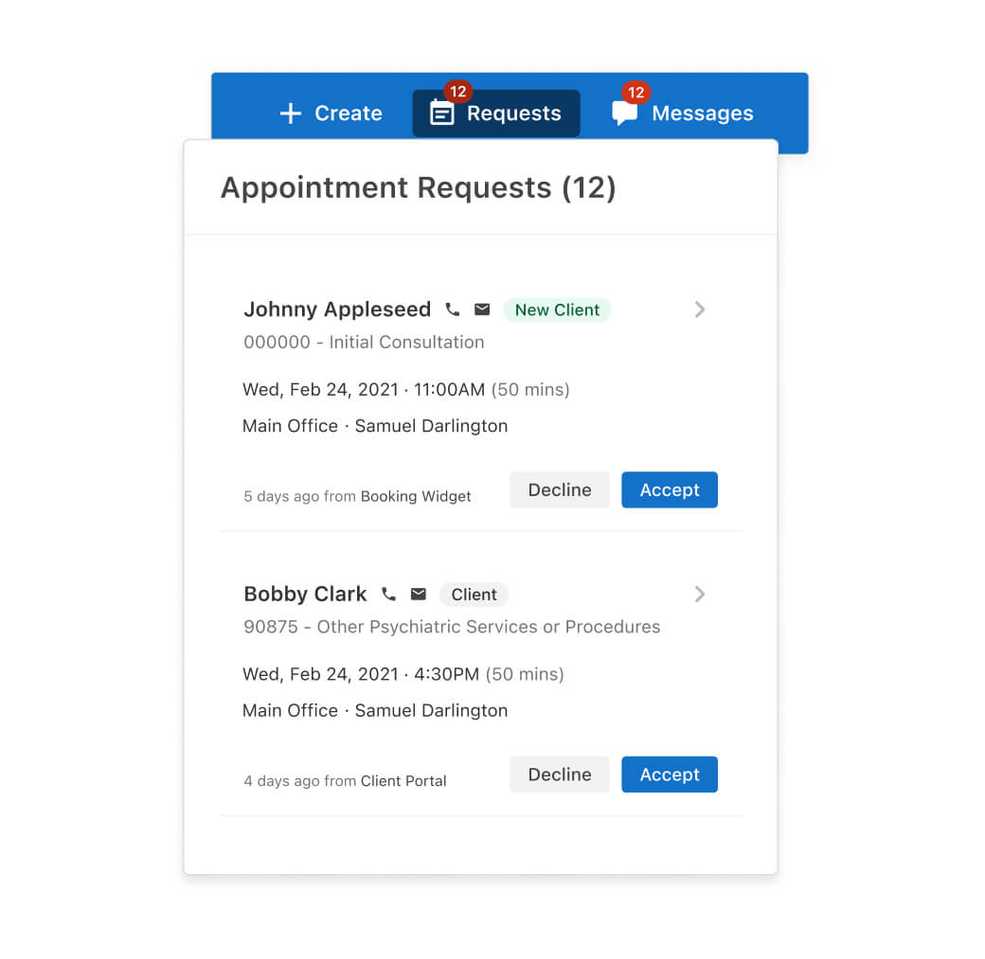
An easier way to review appointment requests
You can easily review new appointment requests at the top of the navigation bar. You can accept, deny, and see appointment requests from new or existing clients.
Unanswered questions are automatically removed
Questions that are left unanswered on assessment forms and progress notes are automatically removed. So when you save, print, or view them as PDFs, you won’t see the “No answer given” response.

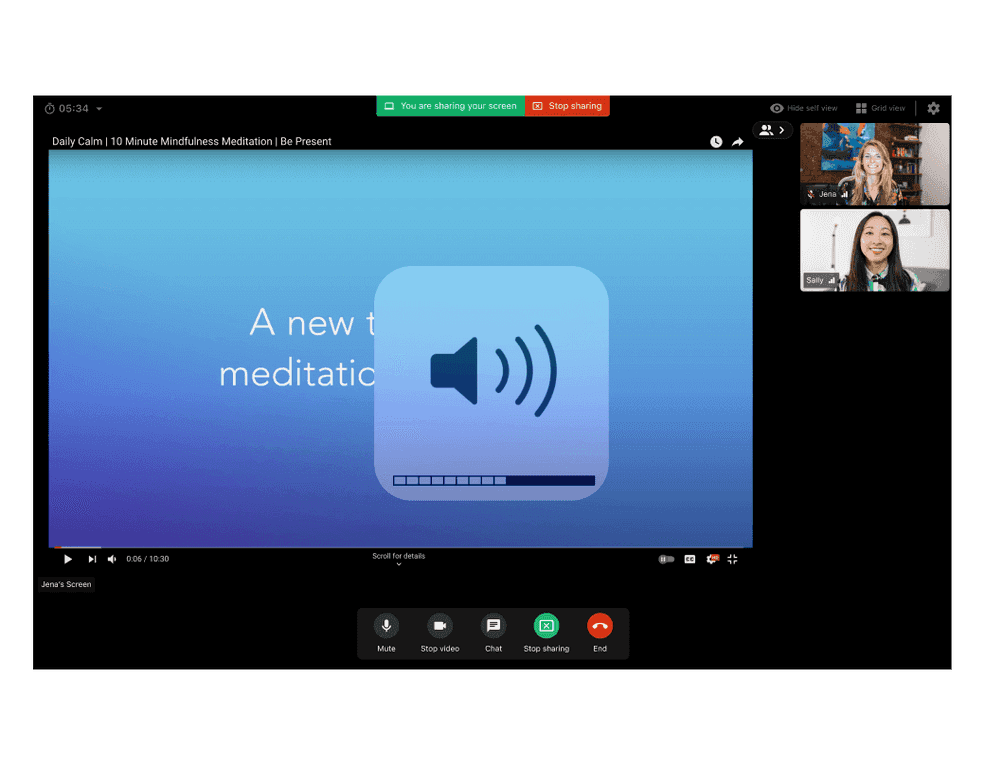
New! Screen-share with sound
You can now share your screen with audio during telehealth sessions. It’s currently available via your web browser*, and supported on mobile and iPad. (*May be limited on certain browsers/devices)
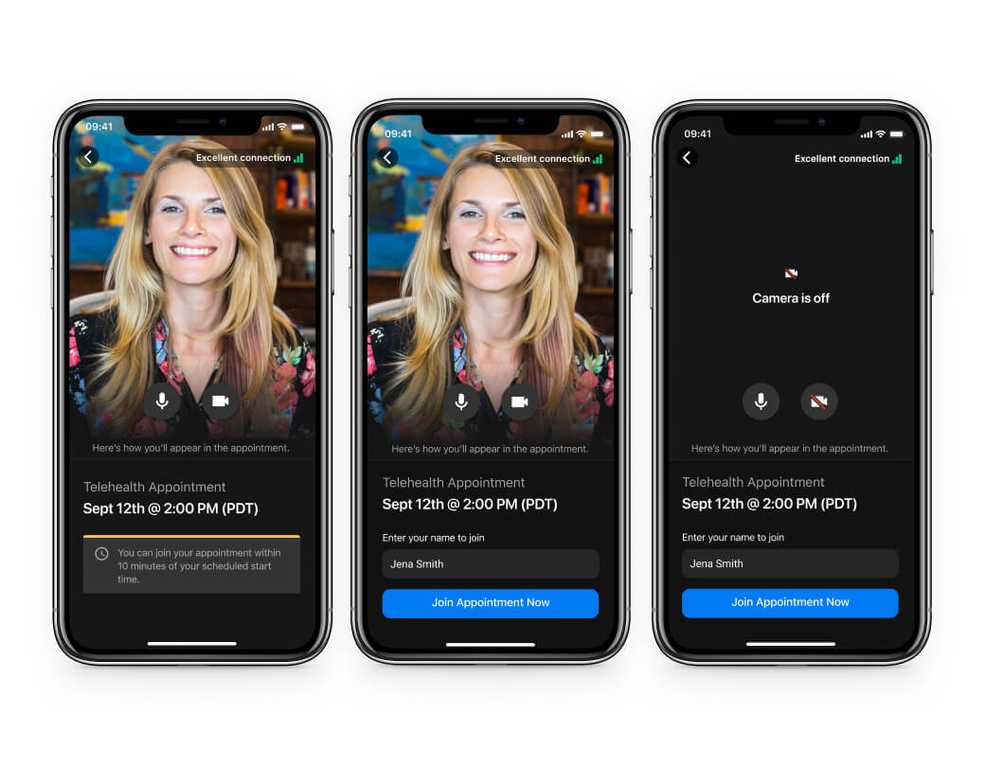
New and improved Telehealth experience on mobile
The Telehealth by SimplePractice mobile app has undergone extensive improvements. We’ve improved everything from the functionality and design to onboarding workflows and the overall experience for both you and your clients.
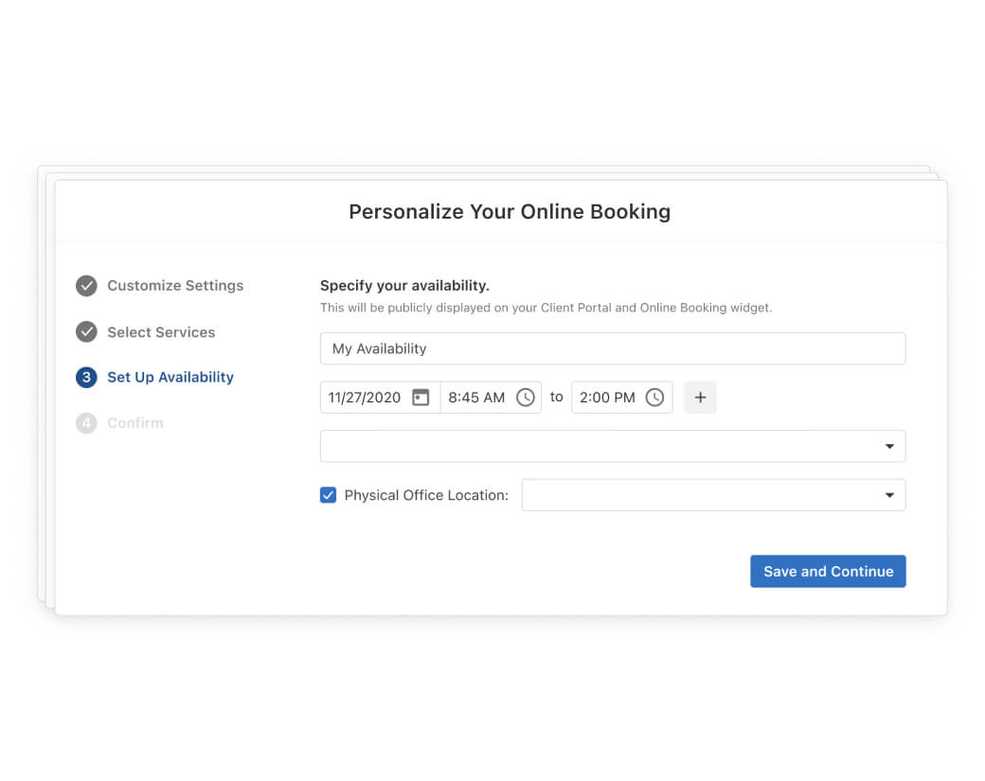
Setting your availability just got easier
Instead of having settings in multiple places, our new simplified workflow makes it easy for customers to adjust their Online Booking settings, add/edit/select services, add availability time blocks, and more.
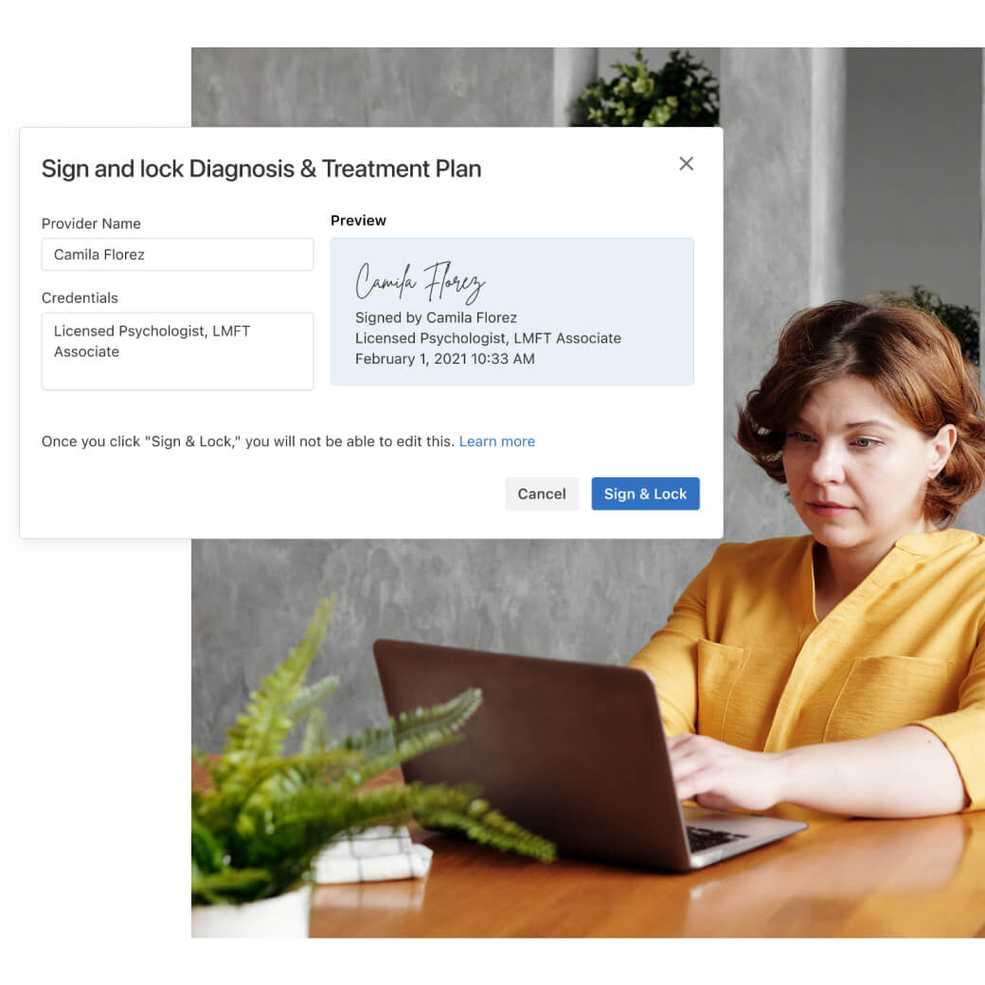
Clinicians can now sign diagnosis and treatment plans
Clinicians and supervisors can electronically sign and lock diagnosis and treatment plans. This means SimplePractice treatment plans will be compliant with various states and payers that require a clinician’s signature—like Medicare, Medicaid, and more.
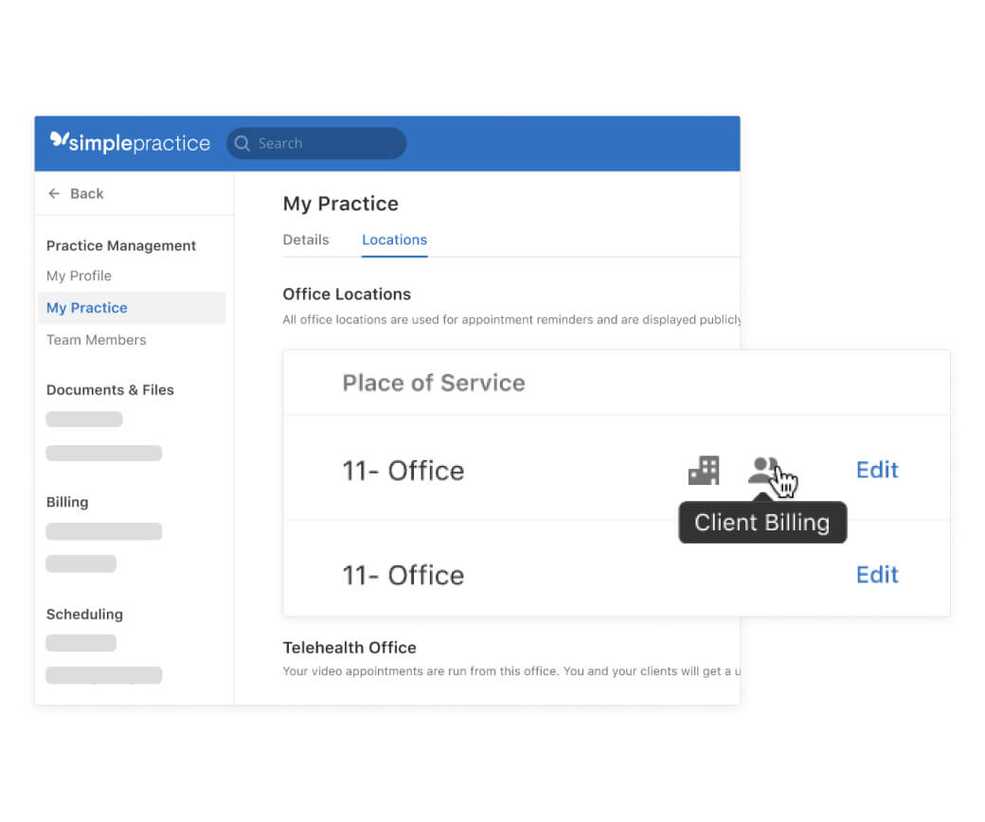
Keep your client and practice billing addresses separate
Now all customers—regardless of whether they have Telehealth enabled—can add a separate billing address for clients to use and/or a business billing address for their practice.
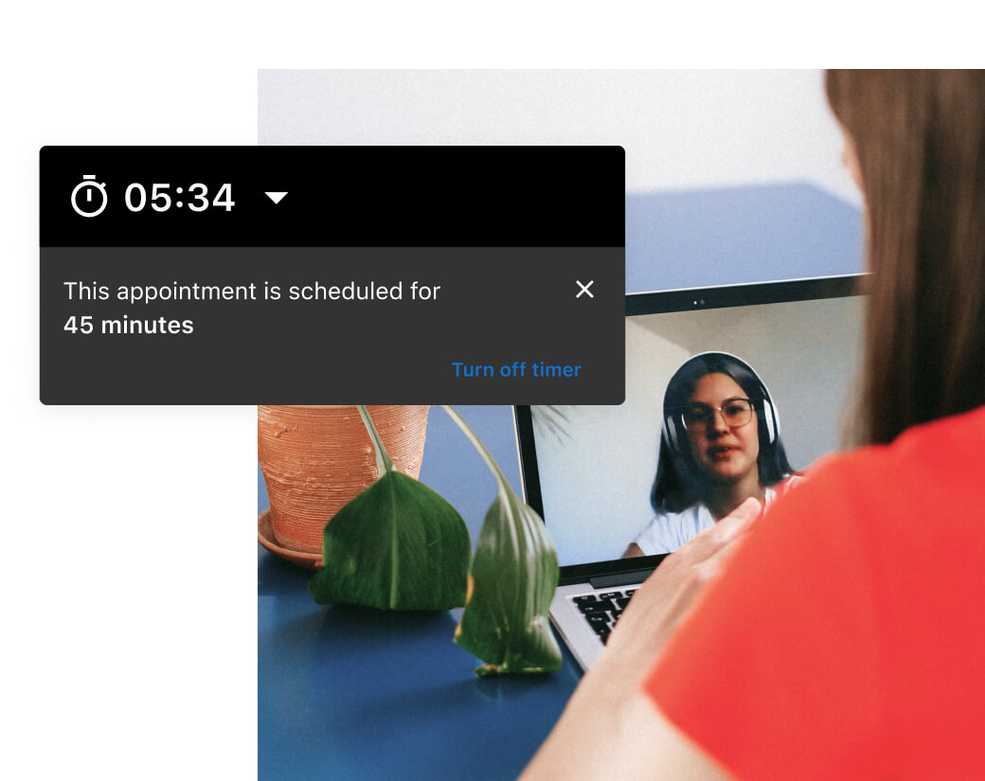
Manage your time better on Telehealth
You no longer need to try to steal a look at your watch or wall clock during virtual sessions. Now you can easily keep an eye on the time with the new Telehealth Timer.
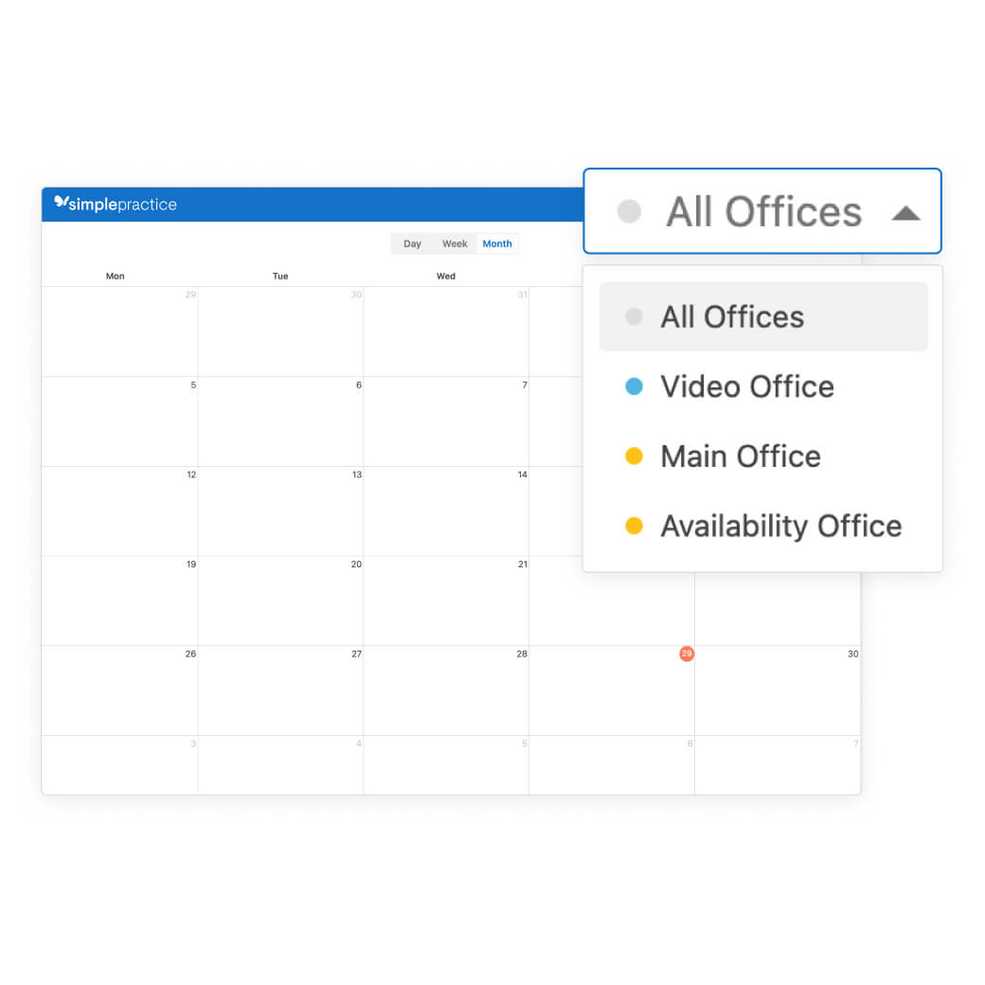
The calendar is getting a fresh new look
We’re making updates to the calendar navigation. Now, all your office locations will have a corresponding color so you can identify them at a glance. Plus, it’ll be easier to see and set the availability for each location and clinician.
Get quick answers through the iOS mobile app
The SimplePractice mobile app makes it easy to run your business from anywhere. Now, you can easily get the support you need from anywhere, too. View Help Center guides and send support requests—right from your iOS mobile device.
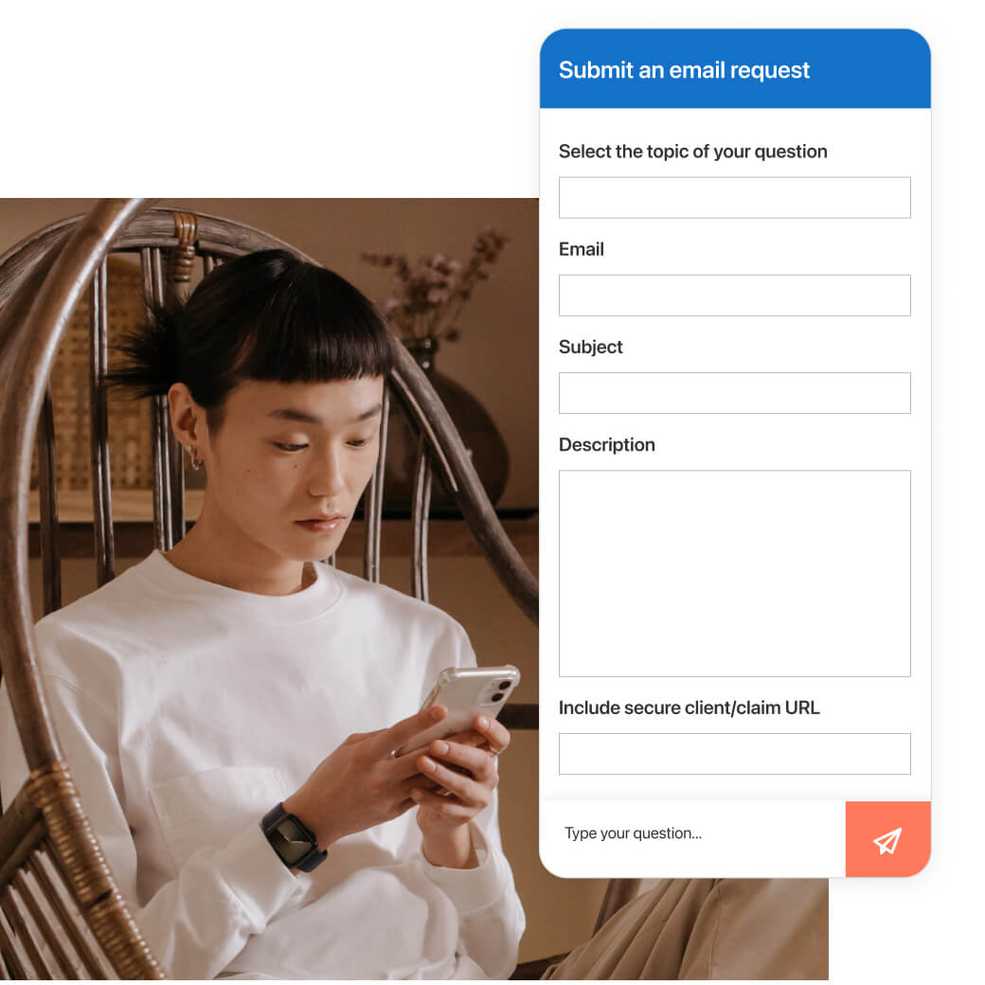
A smarter way to organize your group practice
Group practice owners now have greater control and flexibility when it comes to how their clinicians are displayed in their SimplePractice account—they can choose to order them alphabetically or keep them in the order they were added.
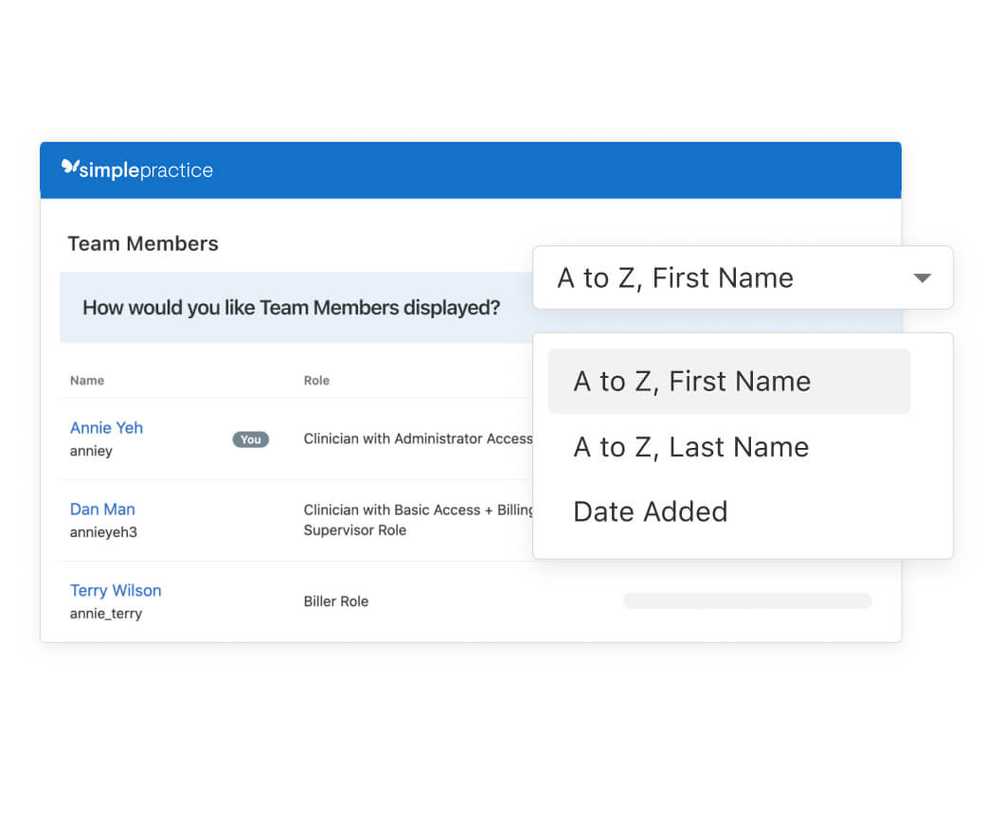
Online appointment request enhancements
Now when clients request an appointment online, they can easily see which time slots they can request online versus which ones they have to call to request.
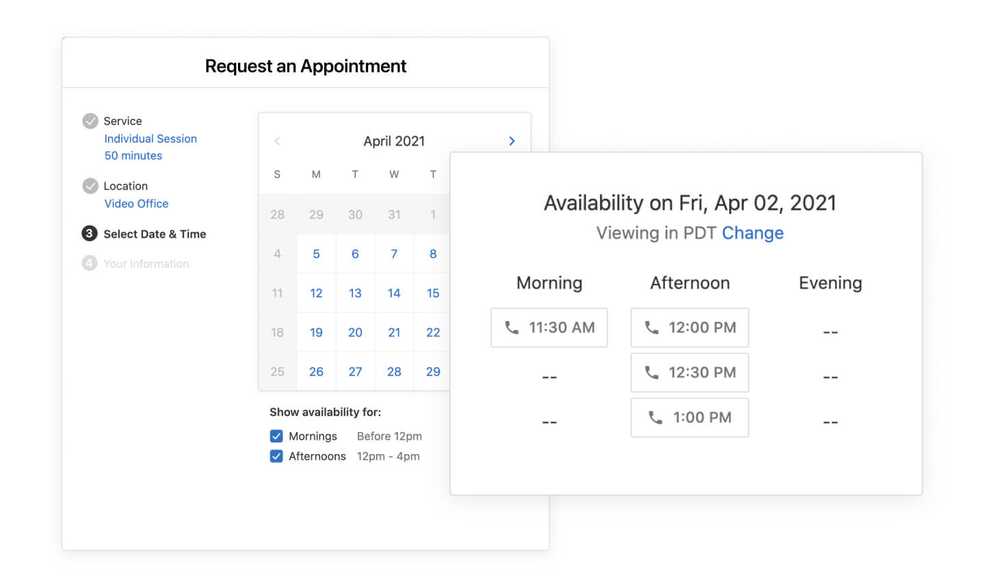
eSignature on progress notes and assessments
Clinicians can now sign progress notes and assessments with the new cursive esignature functionality that includes your credentials.
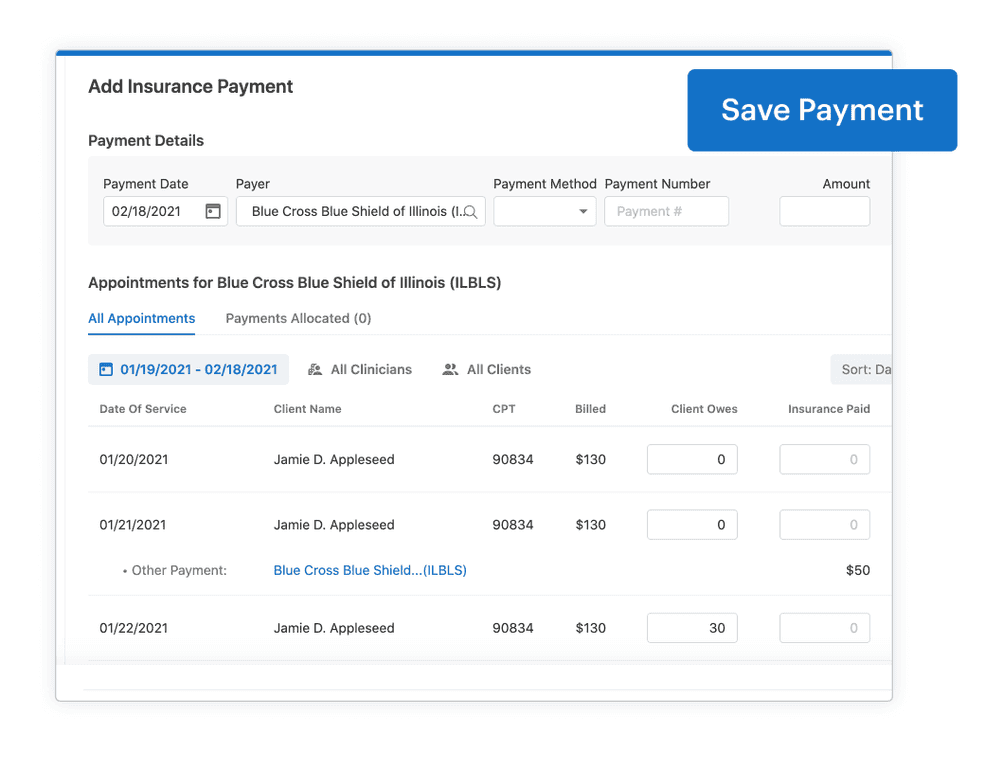
Your Add Insurance Payments page has a new look
It includes a new Payments Allocated tab, the ability to add a new payment quickly, an enhanced write off feature that calculates both primary and secondary insurance payments, and more.
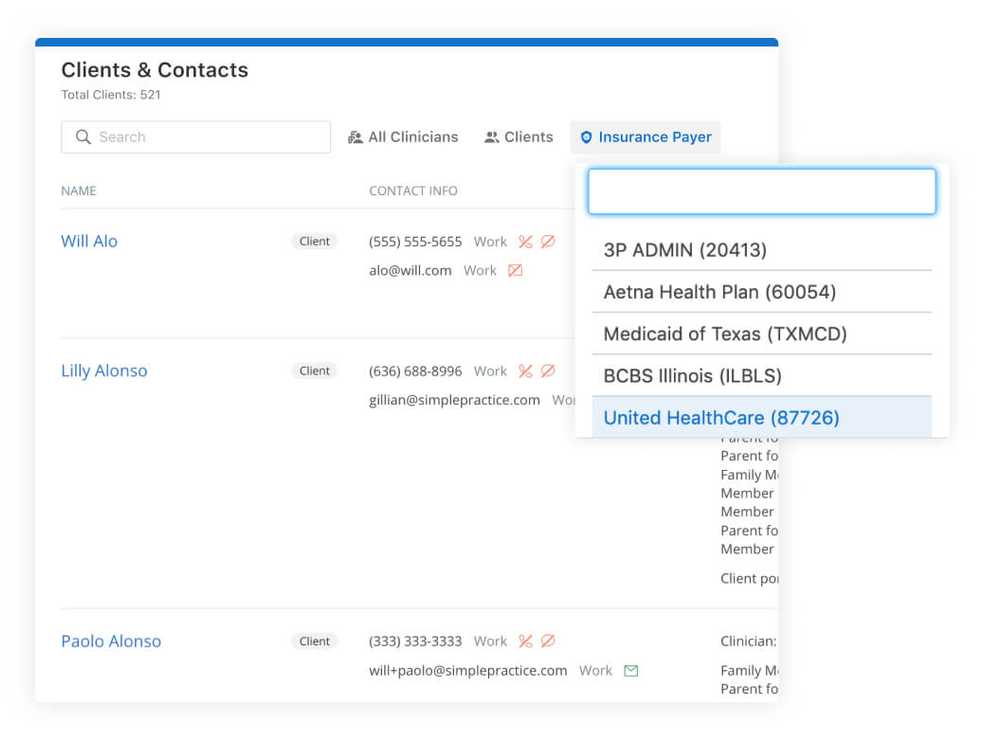
Filter your clients by insurance payer
Practice Owners, Clinicians, Billers, and Schedulers now have an easy way to search for clients by insurance payer. Go to the Clients & Contacts page to check it out.
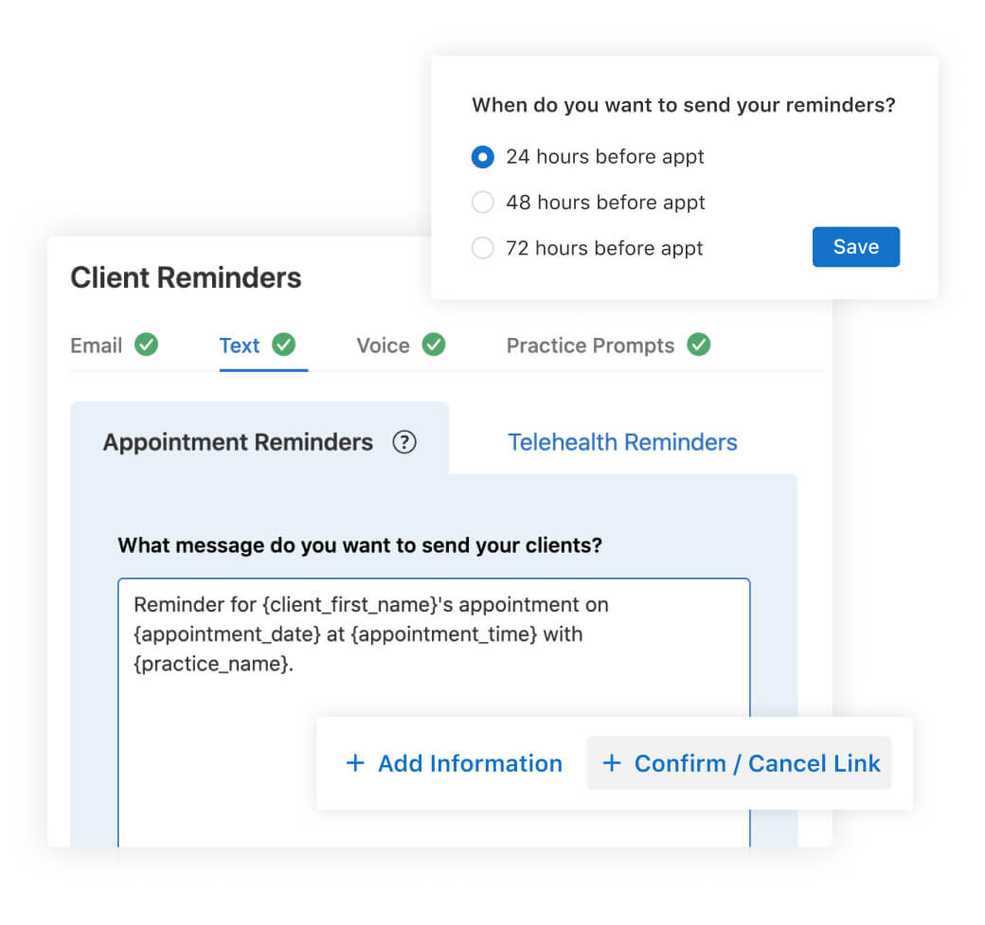
Improved text reminders, including confirm or cancel via text message
Text reminders are now easier to customize with simplified language and improved deliverability. And you can opt-in to allow clients to confirm and/or cancel their upcoming appointment via text message.
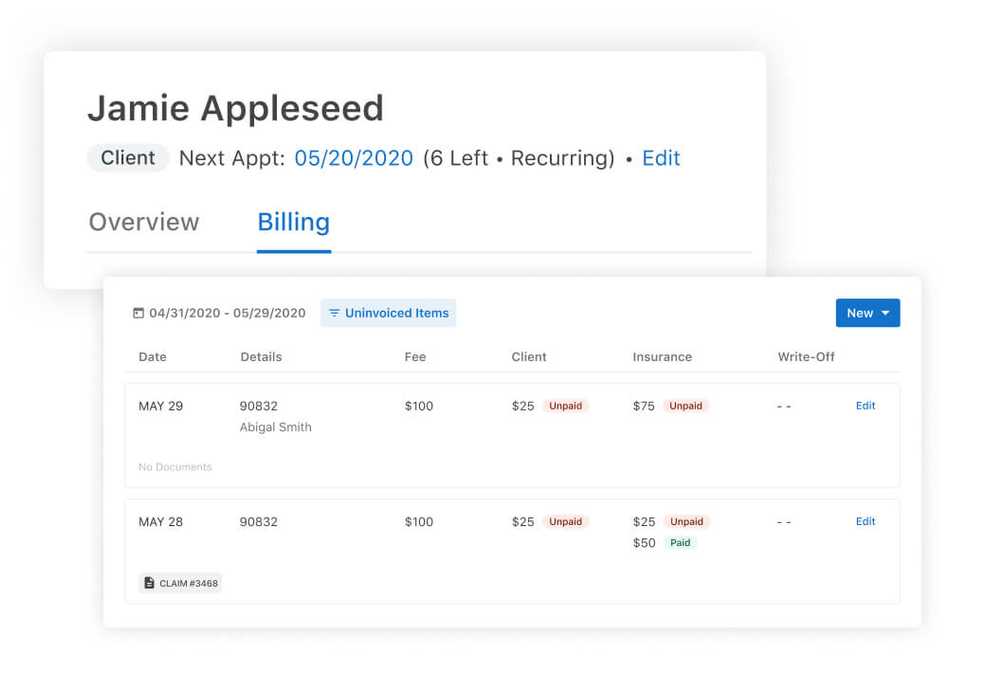
New and improved client billing overview page
You now have greater flexibility, transparency, and control over your billing. To make sure you’re comfortable with the Client Billing system’s new and improved functionality, you’ll still have access to the ‘Classic View’ until the end of March 2021.
iOS mobile app has been updated to v9.0.0
In this update, the iOS mobile app has an improved navigation bar and new features to simplify your workflow—like the “Today” button to easily navigate back to your current schedule.
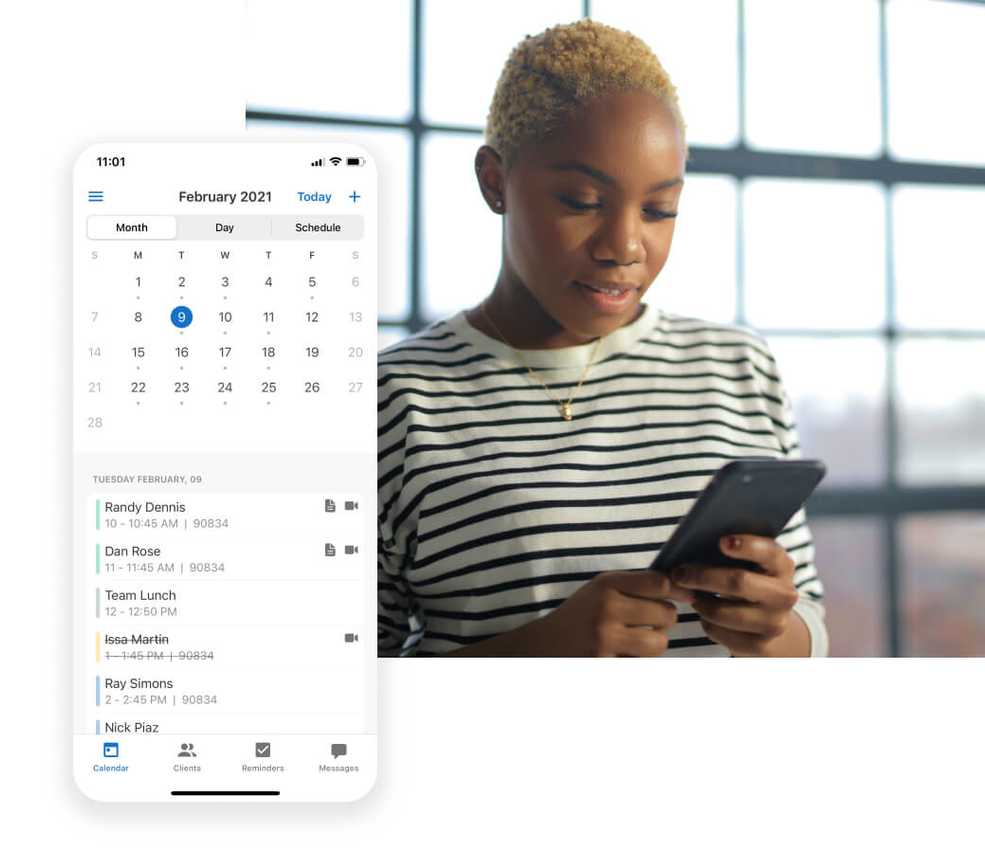
Automate your closing pay periods
We’ve just automated the cycle for locking pay periods. To enable this feature, go to your Team Members > Payroll settings. Under Pay Periods, use the dropdown menu to select the Close Pay Periods option that aligns with your practice’s payroll schedule, whether that’s manually (default), weekly, biweekly, semi-monthly, or monthly.
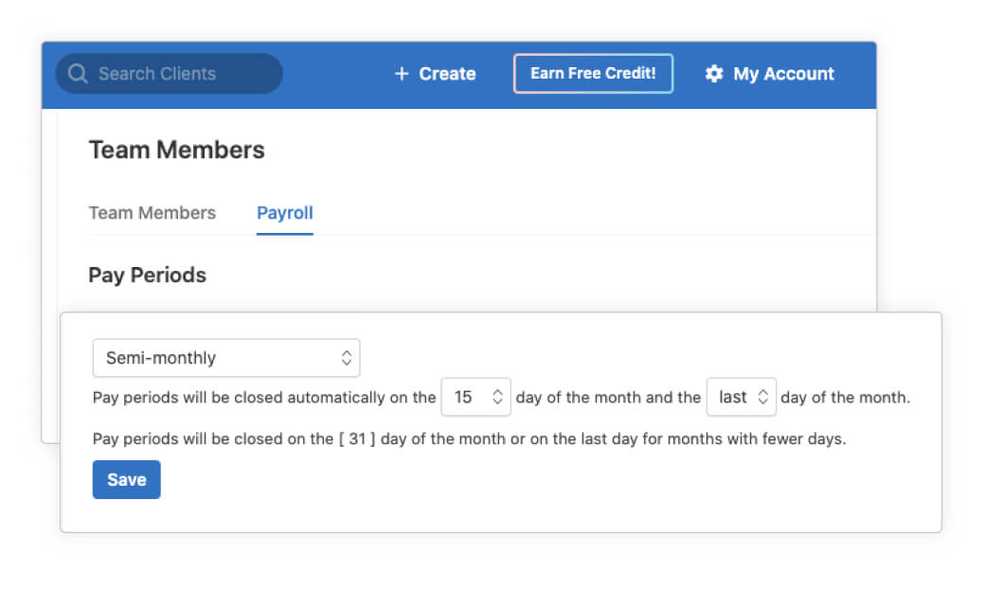
A simpler way to check if a client is active
Easily identify a client’s status with an Active or Inactive badge. Change their status at any time.
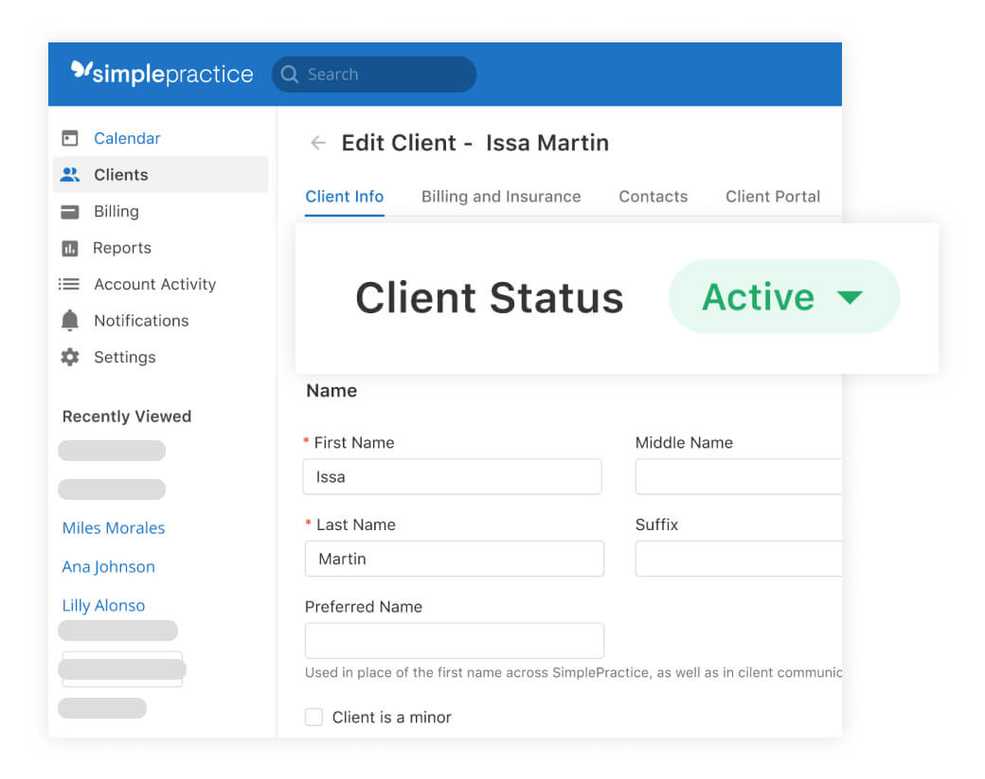
Ability to upload insurance cards on the demographic form
The demographic form now includes an intuitive “upload section.” If Insurance is selected in your Client Portal settings, clients can easily upload their insurance cards along with the rest of their demographic information. Clients also have the option to snap a picture of their insurance card and upload it directly from mobile.
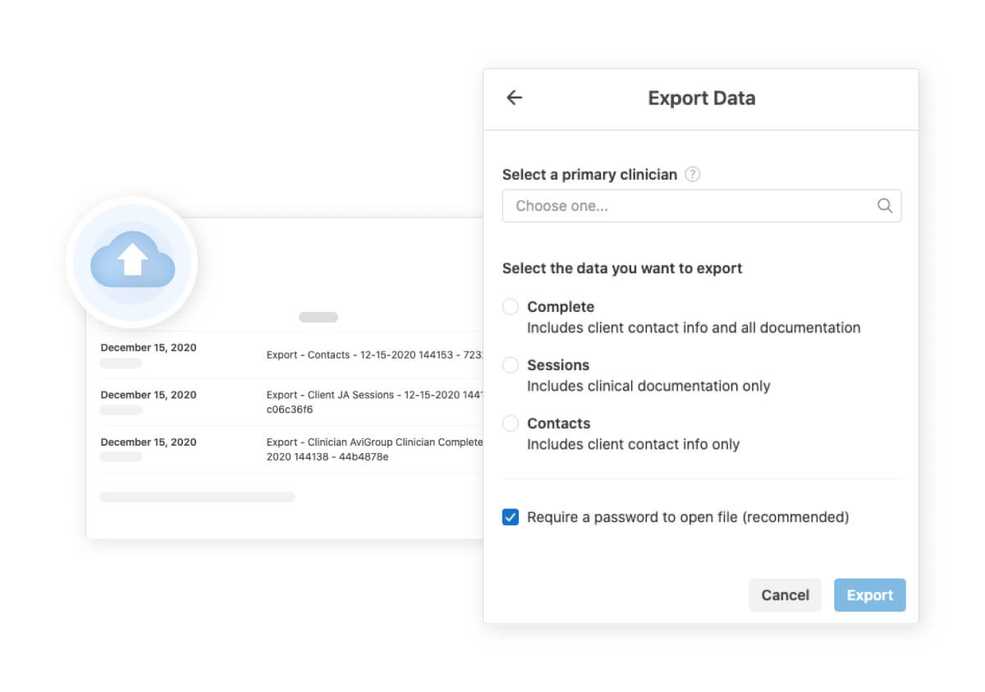
A new data export experience for group practices
In addition to exporting data for just one client, you can export data for just one clinician. This allows the account owner to easily create an export file for all the clients that belong to a single primary clinician.
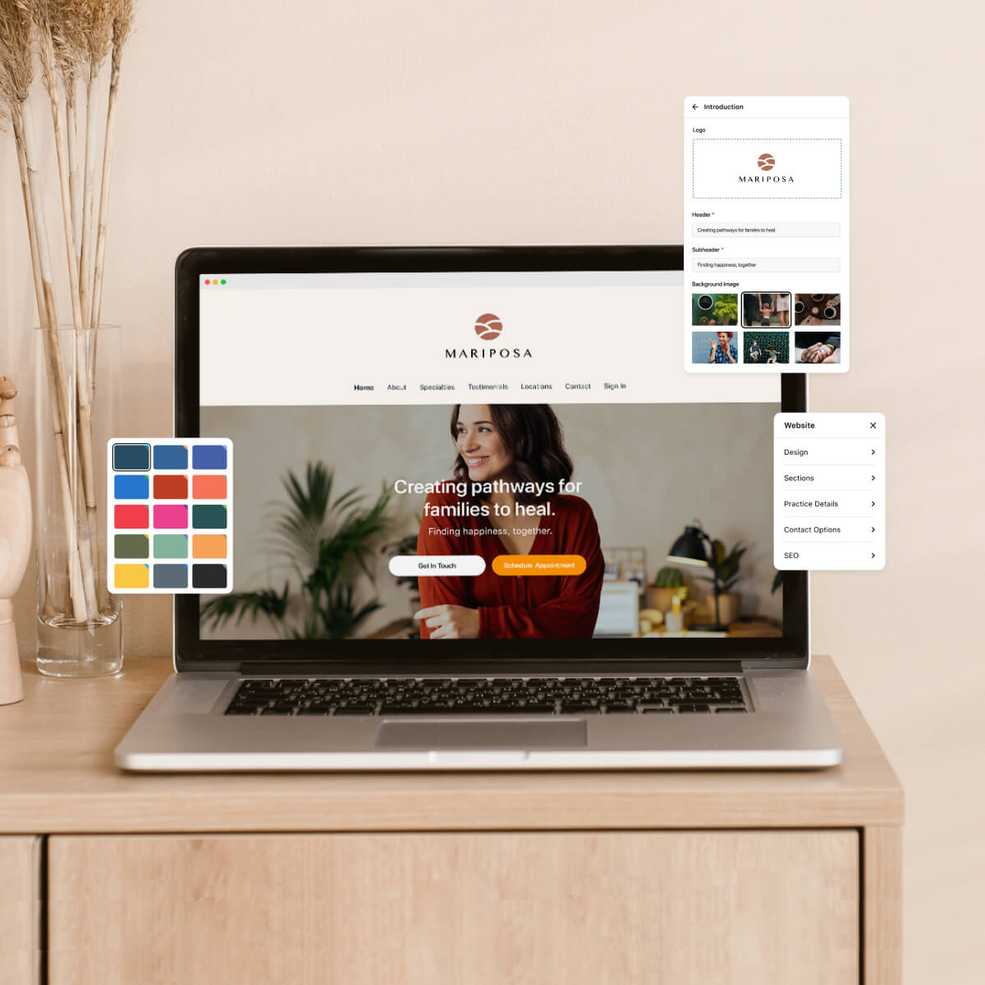
It’s time to meet your new website
Ditch the expensive web developer, avoid the complicated website builder, and upgrade to The Professional Website by SimplePractice. This new feature is free for all customers on the Professional plan until July 2021, then it’s only $15/month.
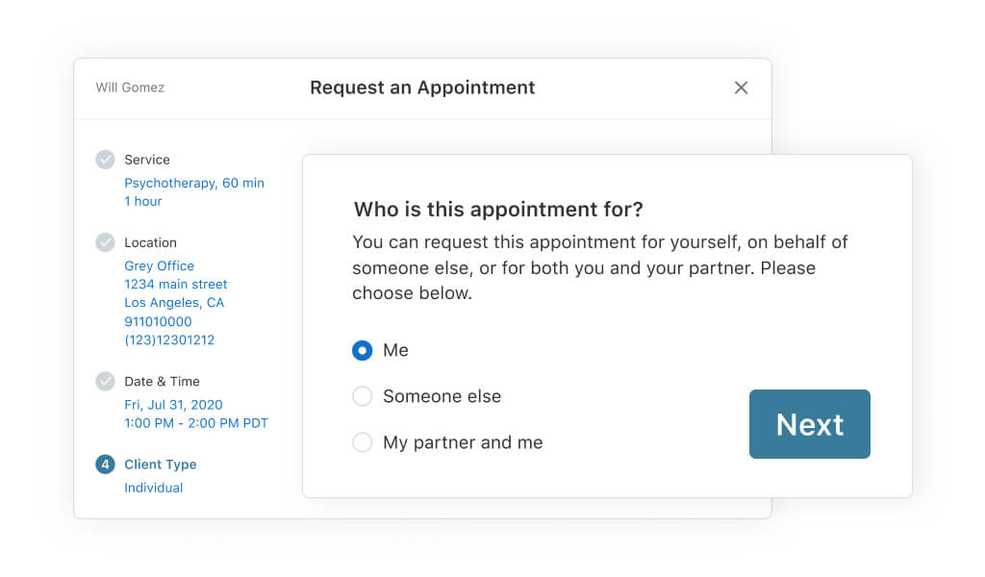
A better Online Booking experience for minors and couples
Working with new minor and couple clients just got easier. When an individual requests their first appointment, you can choose to let them identify if they are booking an appointment as a parent or guardian for a minor client, a couple, or a caretaker.
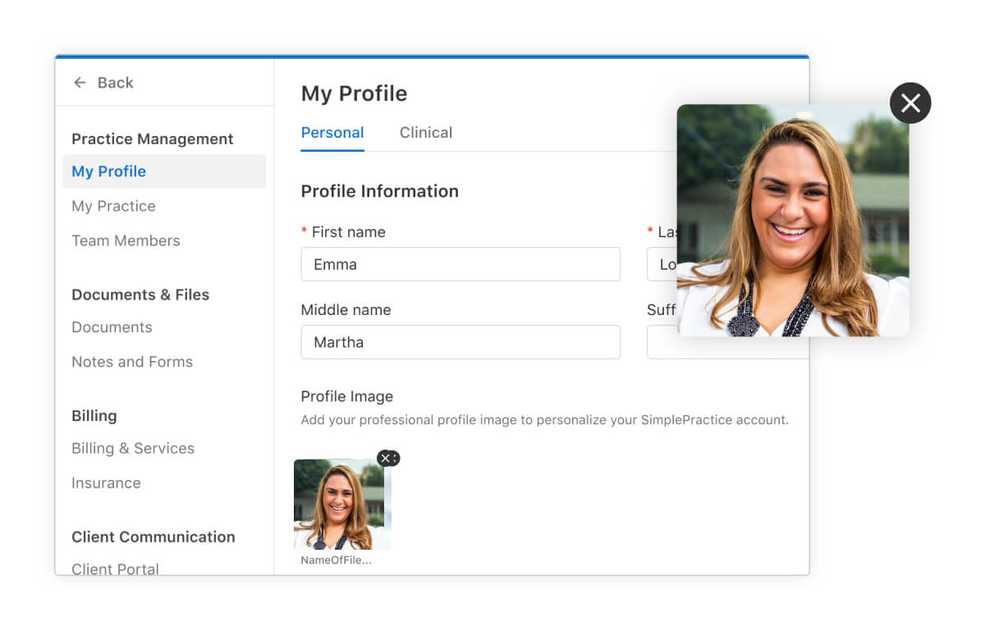
Add a personal touch with a profile photo
To add your photo, go to Settings > My Profile, and upload your very own headshot. Once you’ve uploaded and saved your new profile photo, it will show in the top navigation bar of your account.
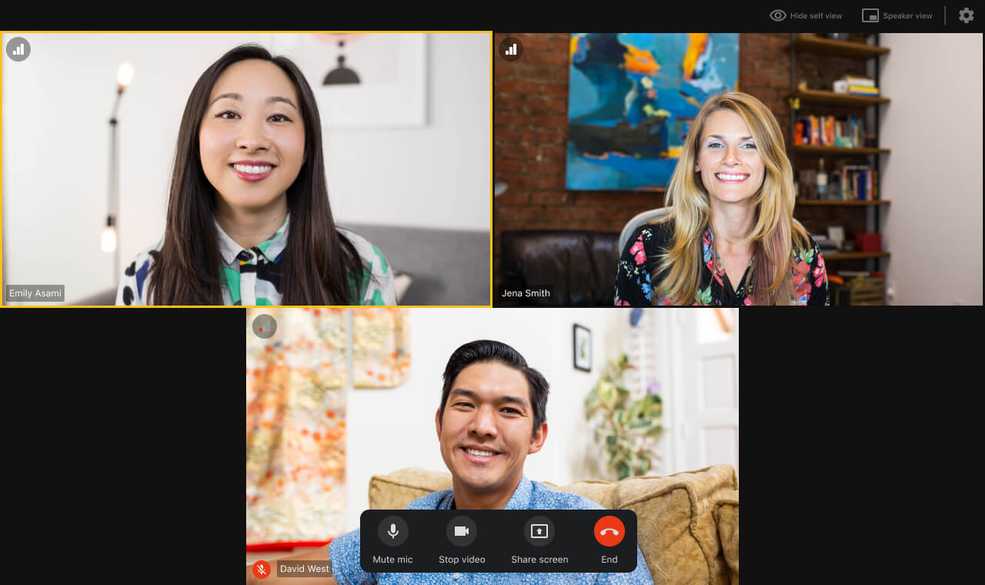
New viewing options in Telehealth
Telehealth now has more customizable viewing options while you’re on a call, so you can put your focus where it’s needed most. Now, you can hide your self view so your whole screen is dedicated to your client, and you can pin anyone, regardless of who’s speaking. You can also switch easily between Speaker and Grid View while you’re on the call.
SimplePractice is HITRUST CSF® certified
HITRUST is the only certification that aligns 100% with HIPAA and includes security controls for CCPA compliance, an increasingly important distinction in the healthcare space. SimplePractice is the first and only electronic health record (EHR) platform available on the market for private practitioners to achieve HITRUST CSF certification, the highest security standards available in its category.

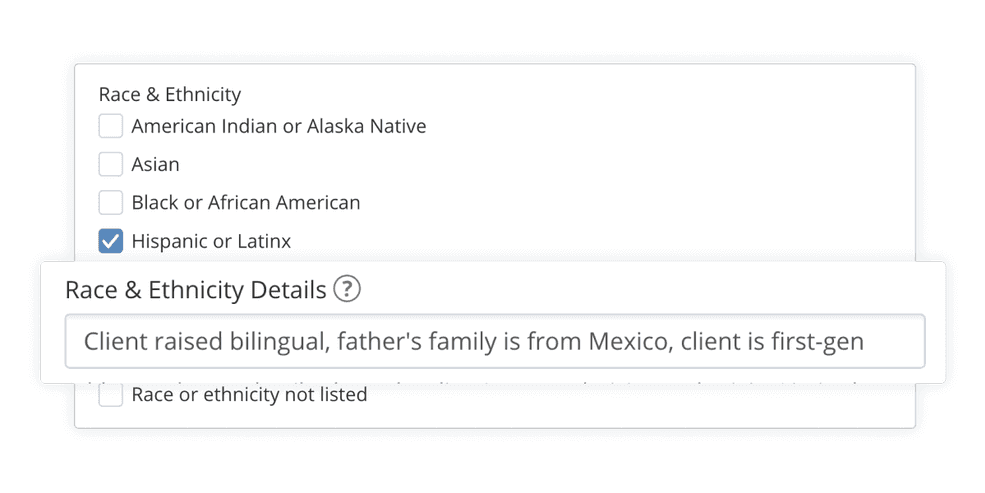
More inclusive Race & Ethnicity options
Race and ethnicity is no longer separated into two different drop-downs. We’ve now grouped race and ethnicity together to be one field in the Client Info settings, drawing upon the 2020 United States Census to create a more inclusive and accurate selection of options to choose from. This section also includes a free text field for you to add any relevant details about your client’s background—like their country of origin or tribal affiliation.
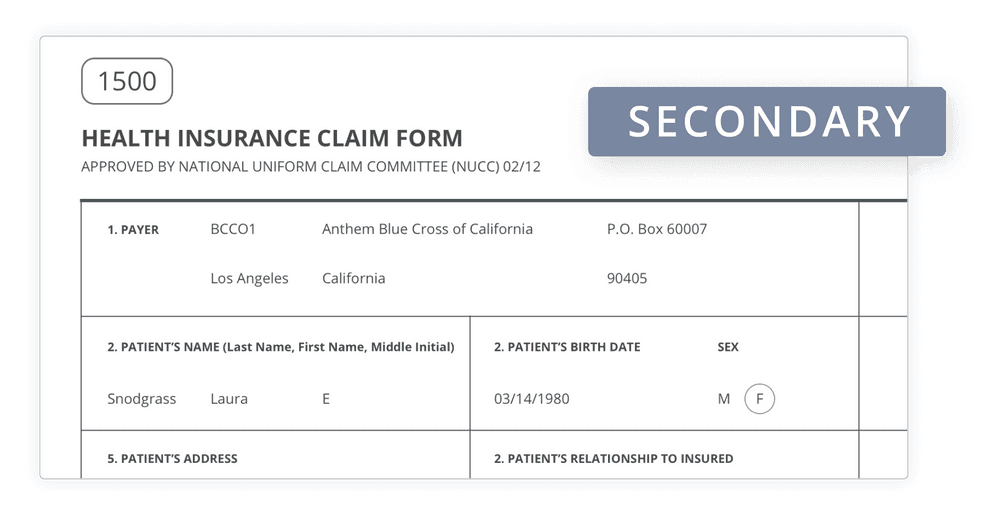
File secondary insurance claims
This update auto-populates the Payment Report (ERA) data from the primary claim onto the secondary claim, so now you can electronically file both with just a few clicks. If you received a Payment Report (ERA) from the primary claim, all you need to do is click “Create Secondary Claim” and “Submit.”
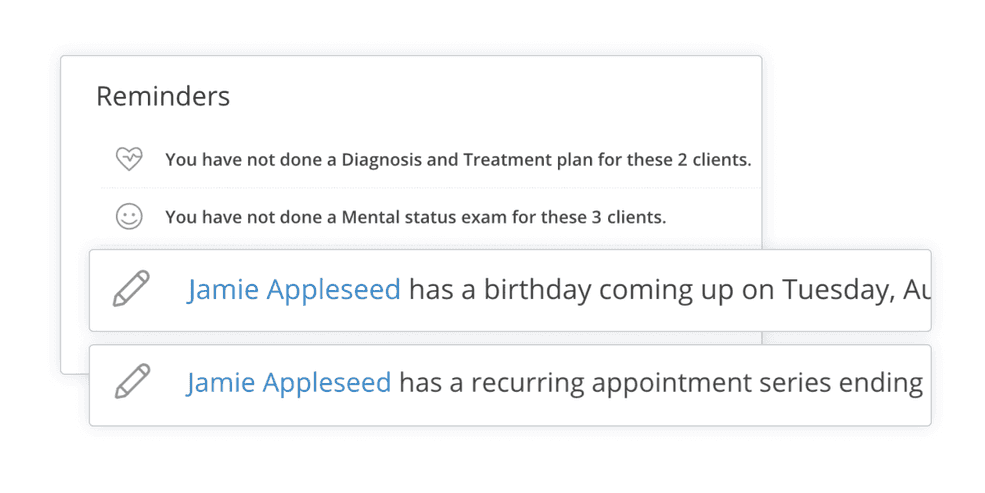
New reminders added
You'll now receive a reminder to wish your client a happy birthday and when a recurring appointment series is about to end. In addition, MSE/Tx reminders have been updated so that reminders only show up after an appointment.
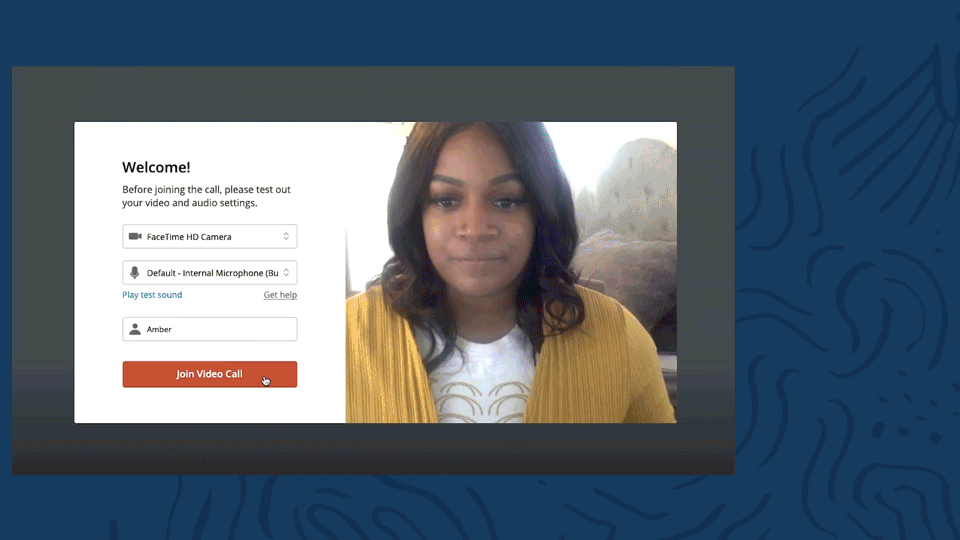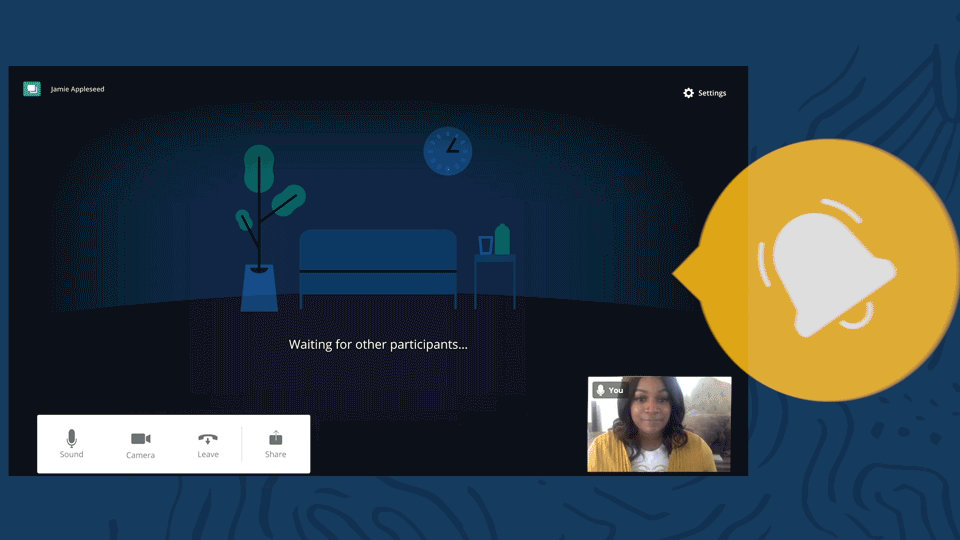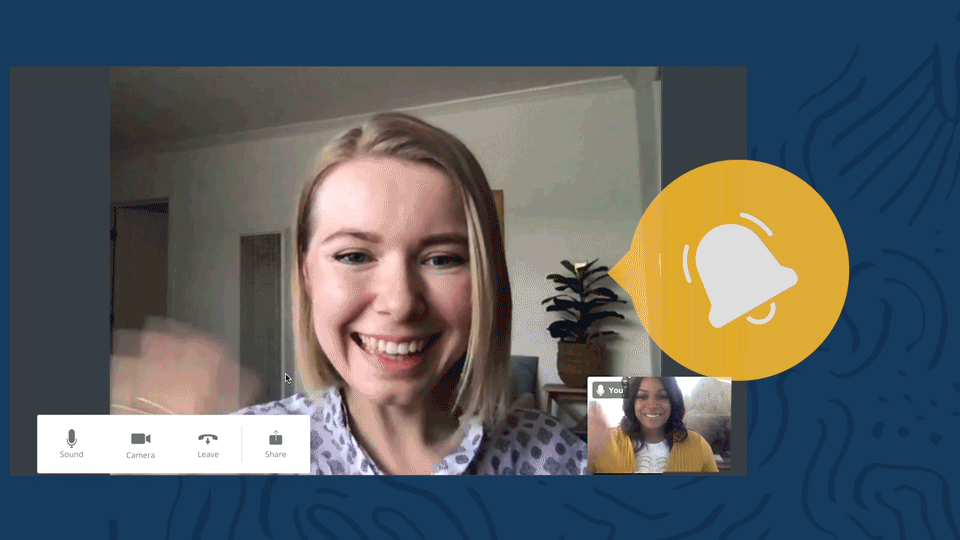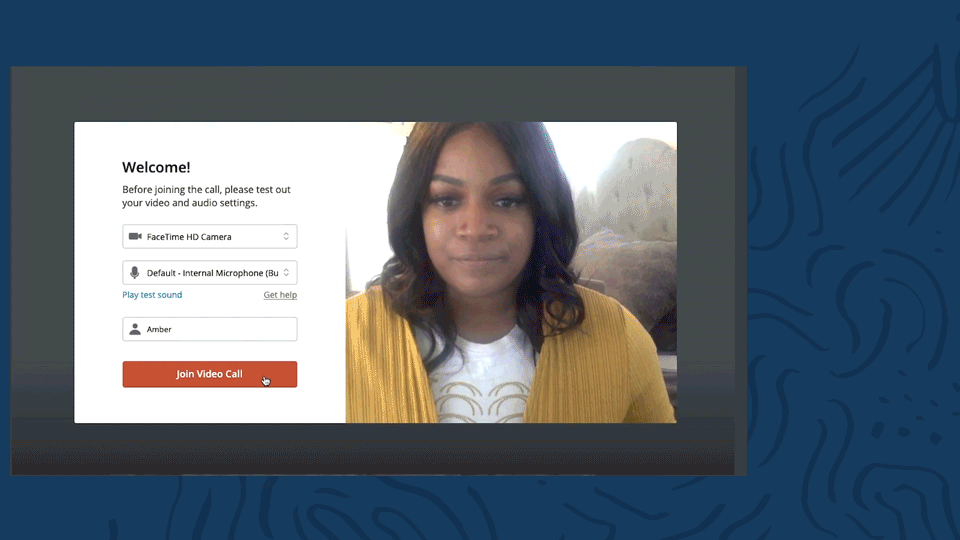
Telehealth sound notification
Whenever a client joins the video appointment, they’ll be introduced with a delightful “ding”. There will also be a sound notification letting you know when a client leaves the video appointment.
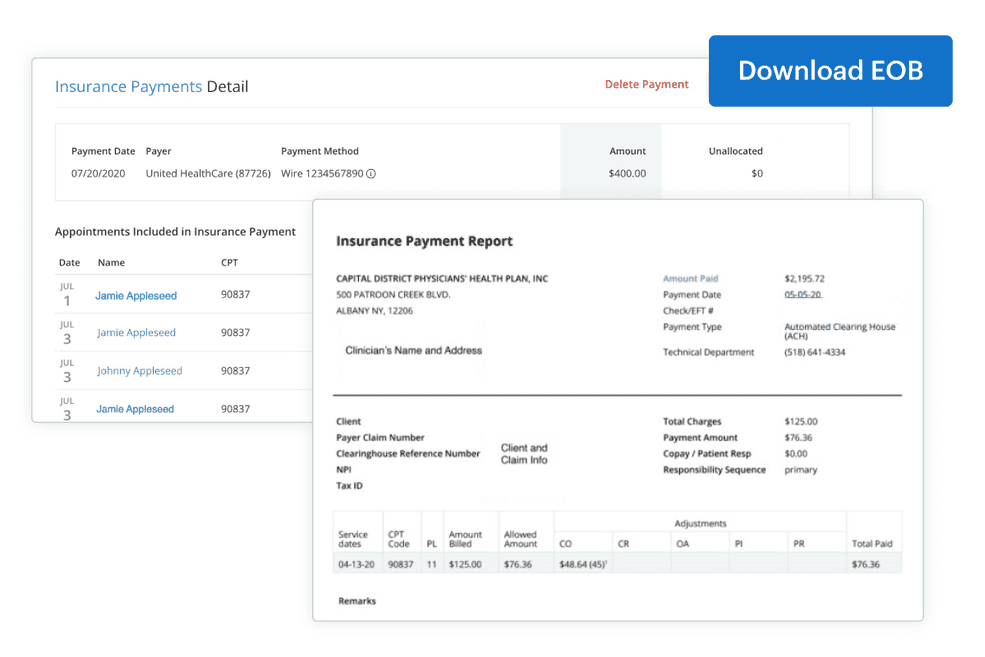
Downloadable Explanation of Benefits (EOBs)
View everything on one, convenient EOB that you can download straight from SimplePractice. You can quickly determine where any unallocated amounts from insurance payments belong. Plus, no more logging into each of the separate insurance companies’ portals to get the information you need.
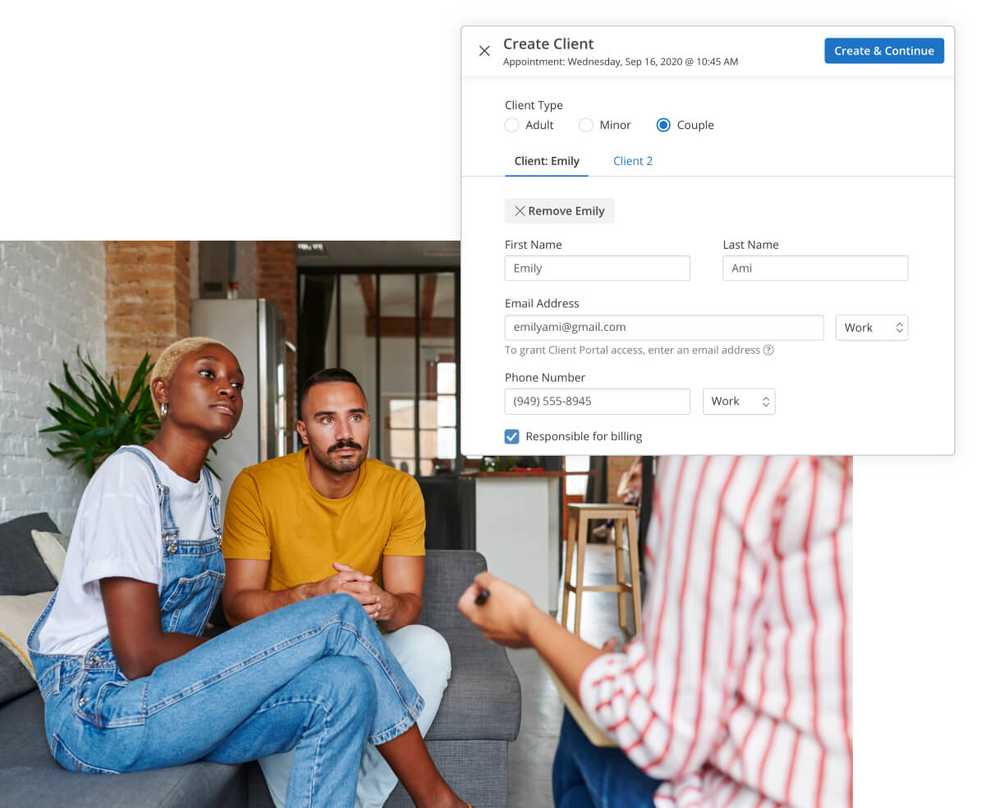
Client management for couples
Client Management for Couples simplifies how you work with couples by creating a single, unified profile for a couple client that’s independent of their individual profiles. This ensures intake paperwork is sent to both individuals, couples’ information is managed and stored on one joint profile, and Telehealth appointment links are sent to both individuals.
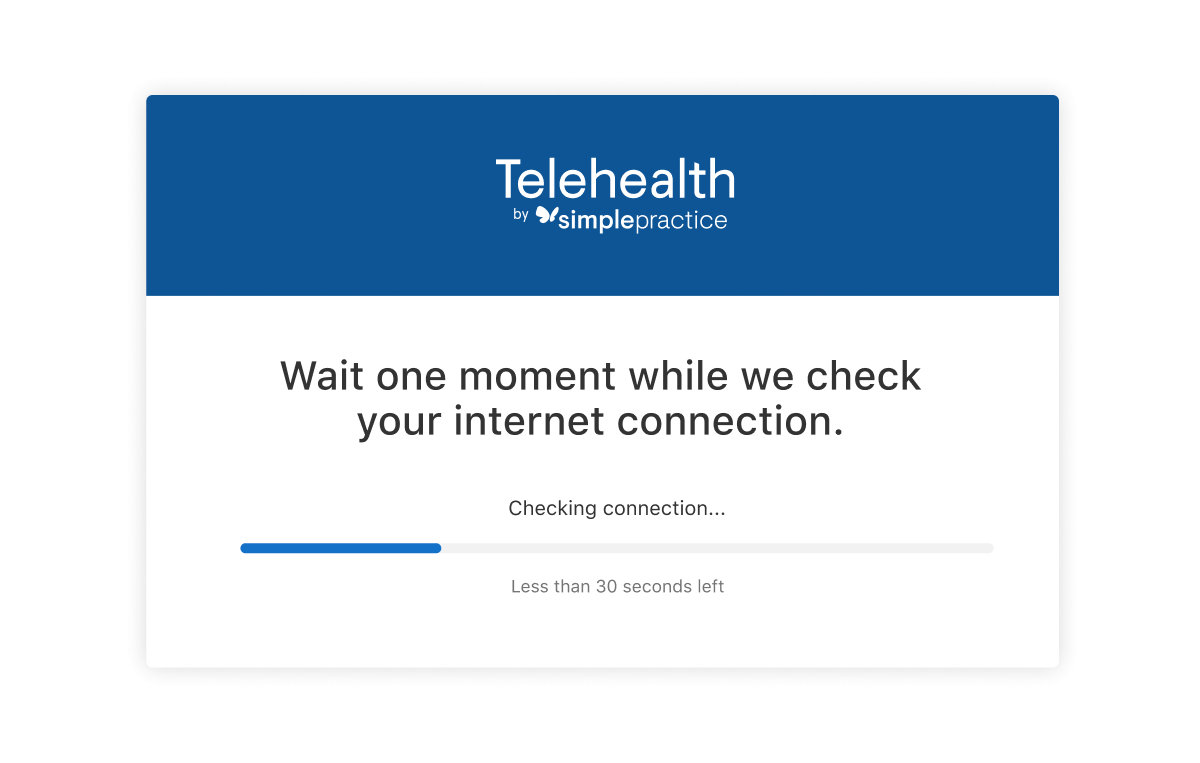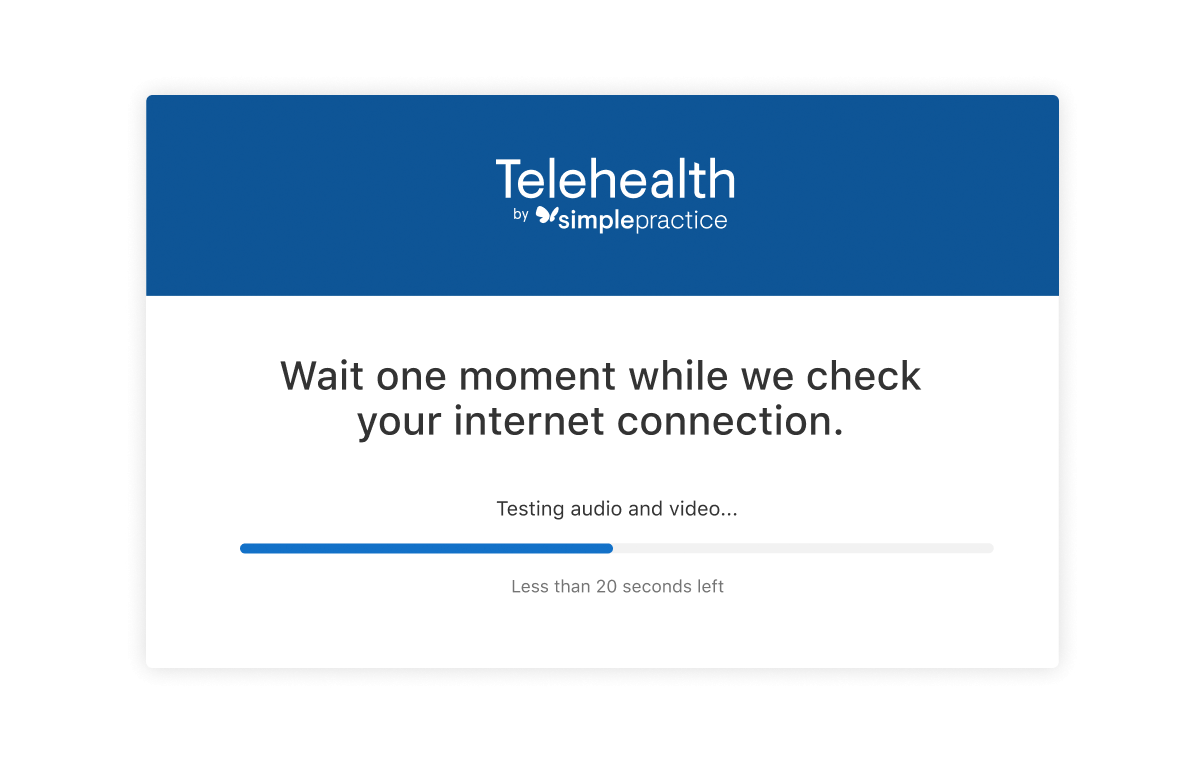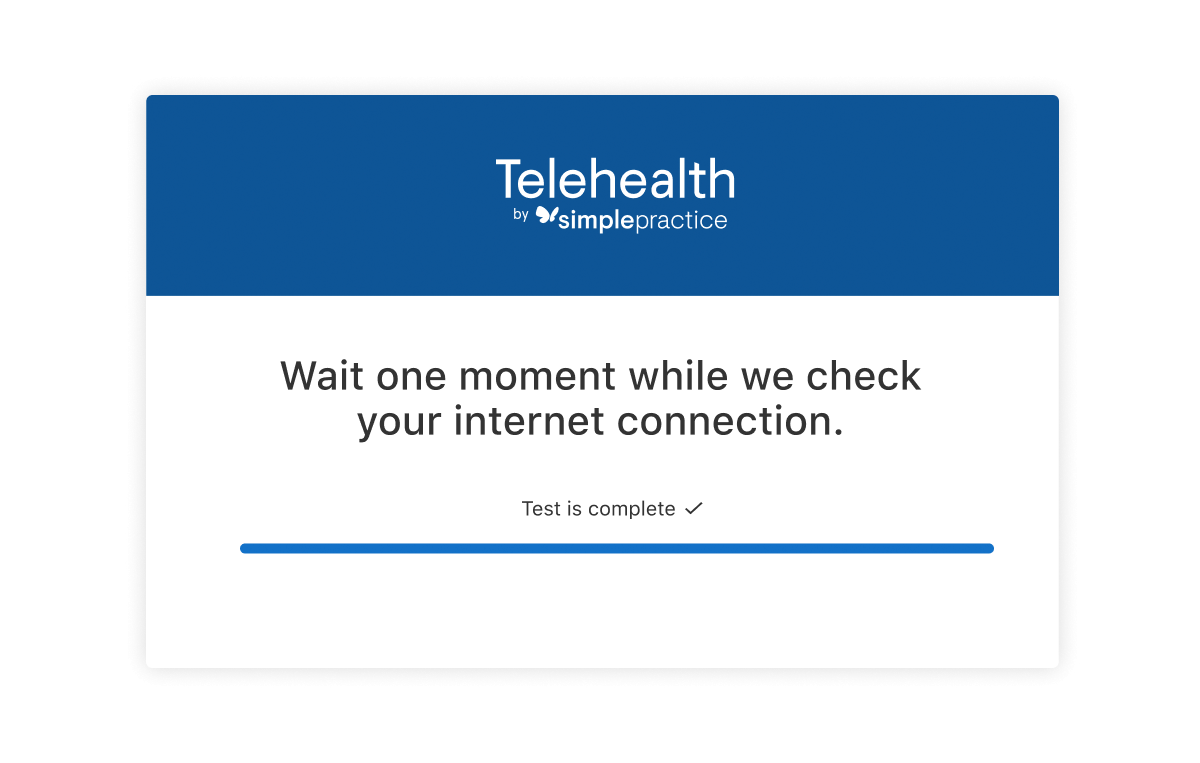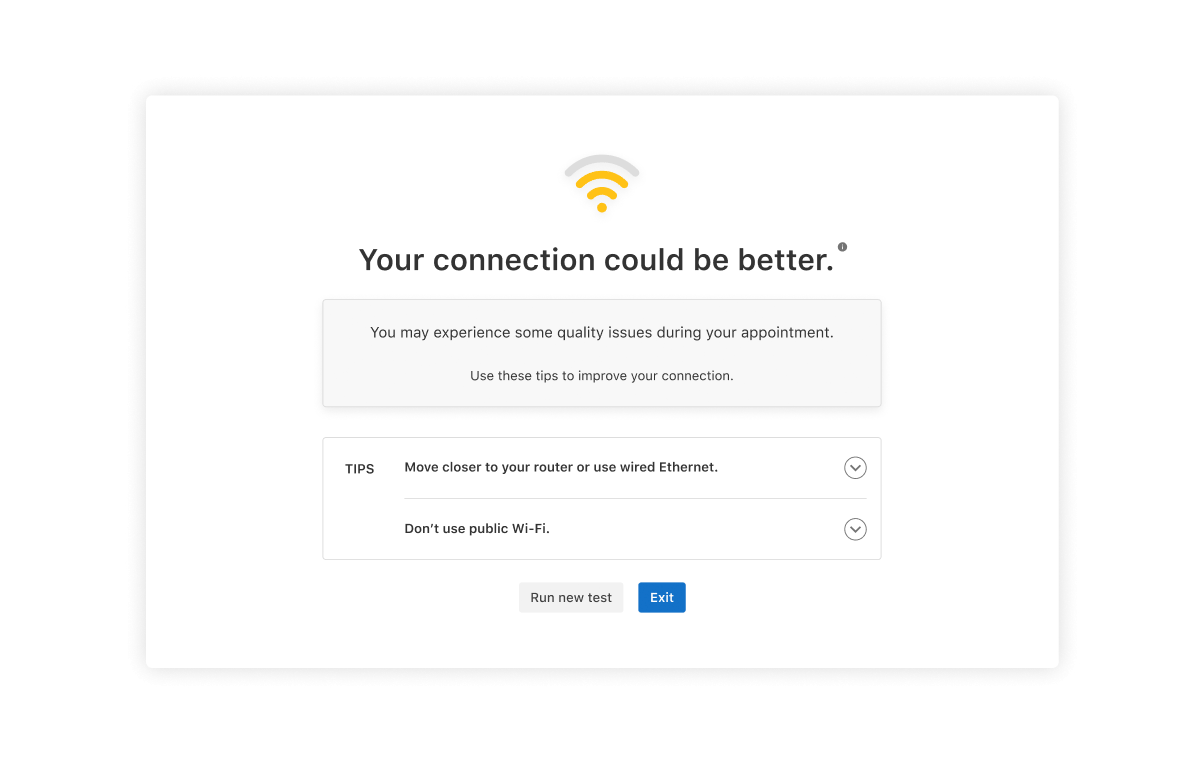
Telehealth internet quality check
Proactively assess the strength of your internet connection prior to joining a Telehealth appointment. If it’s less than excellent, you’ll receive actionable tips to help you problem solve in real-time. Both you and your client will be able to use this.
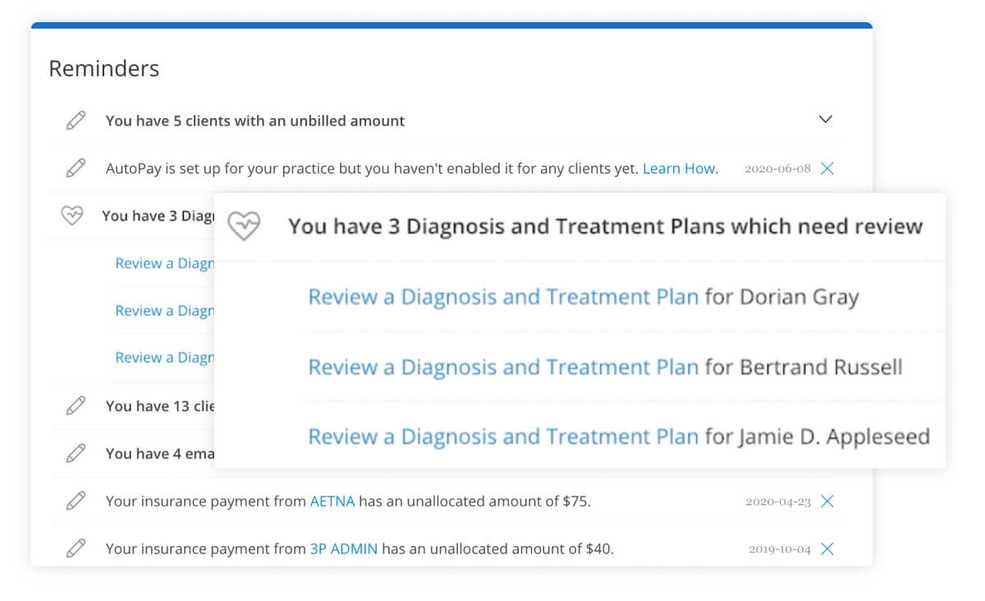
Treatment plan reminders
When creating or editing a client’s treatment plan, you can set a reminder to review the plan anywhere from 7, to 90, to 365 days later. This way, you won’t have to go through every single one of your clients to make sure their treatment plans meet insurance payer requirements.
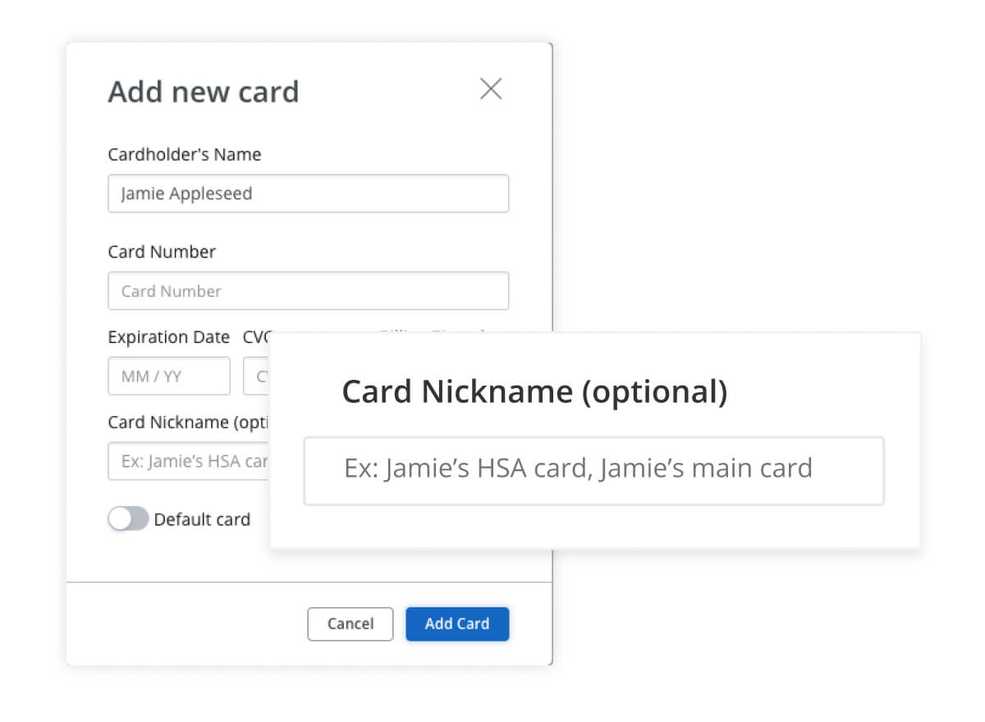
Add a nickname to a client’s credit card
Quickly distinguish between multiple credit cards by adding a Card Nickname to each. Navigate to Client Overview > Edit Details > Billing and Insurance > Credit & Debit Cards to edit an existing card.
Create assessments for your clients
Add an Assessment to your client's file that is not tied to an appointment. Similar to Progress Notes and Intake Forms, you’ll be able to create your own Assessment templates using our Template Builder or by selecting a template from our Template Library as an Assessment under your My Notes & Forms settings. The ability to create your own Assessment template is only available to customers on our Professional Plan.
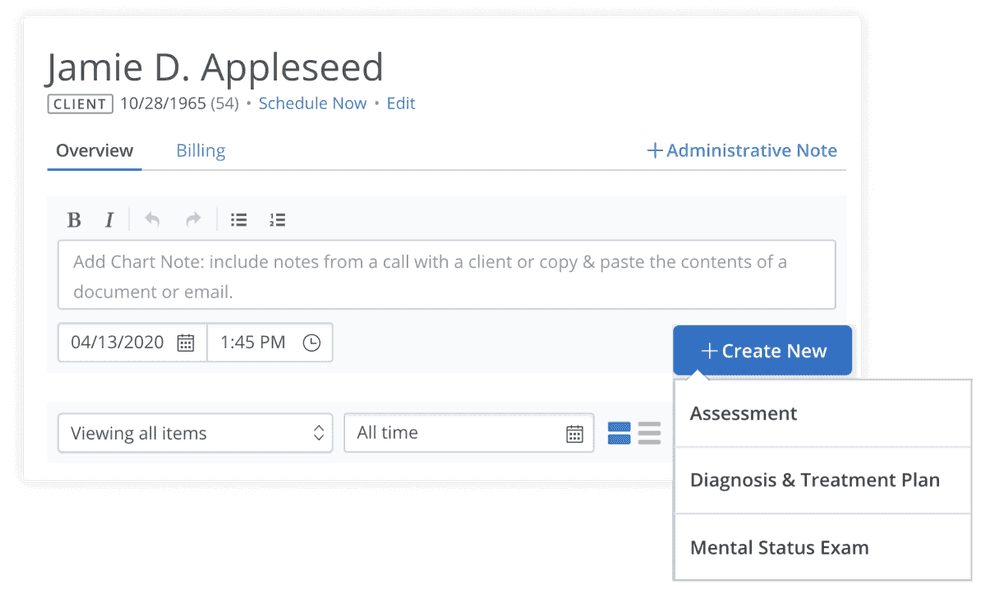
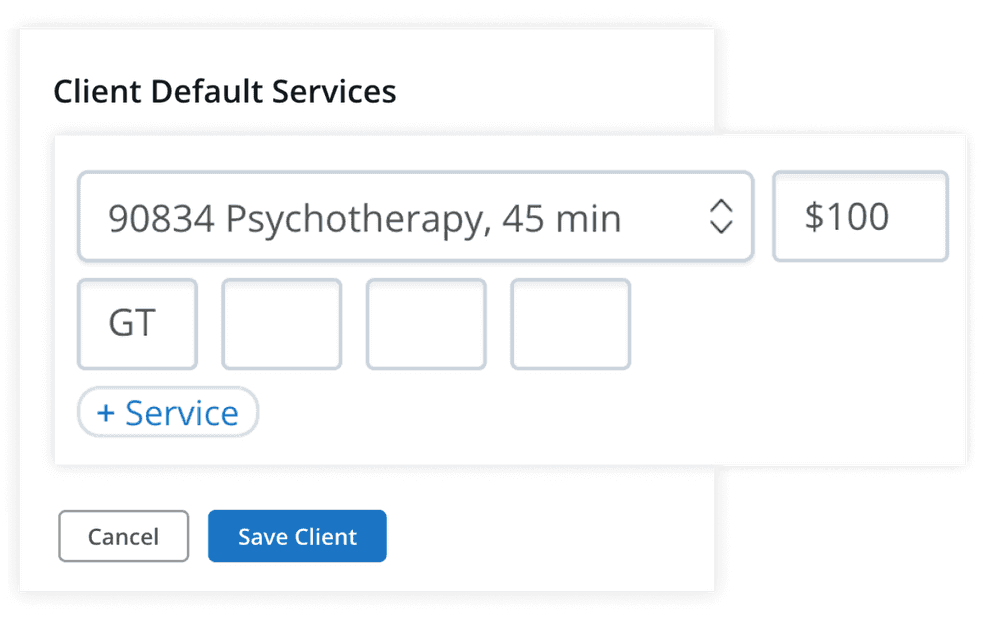
Add insurance modifiers to insurance claims automatically
You can now enable Modifiers under Billing and Services so you can automatically add modifiers to superbills and insurance claims on a client-by-client basis. Once Modifiers are enabled, you’ll can add modifiers from the calendar by clicking a specific appointment or by setting a default service code and modifier for a client on their Billing and Insurance Settings page so it applies to all of their appointments moving forward.
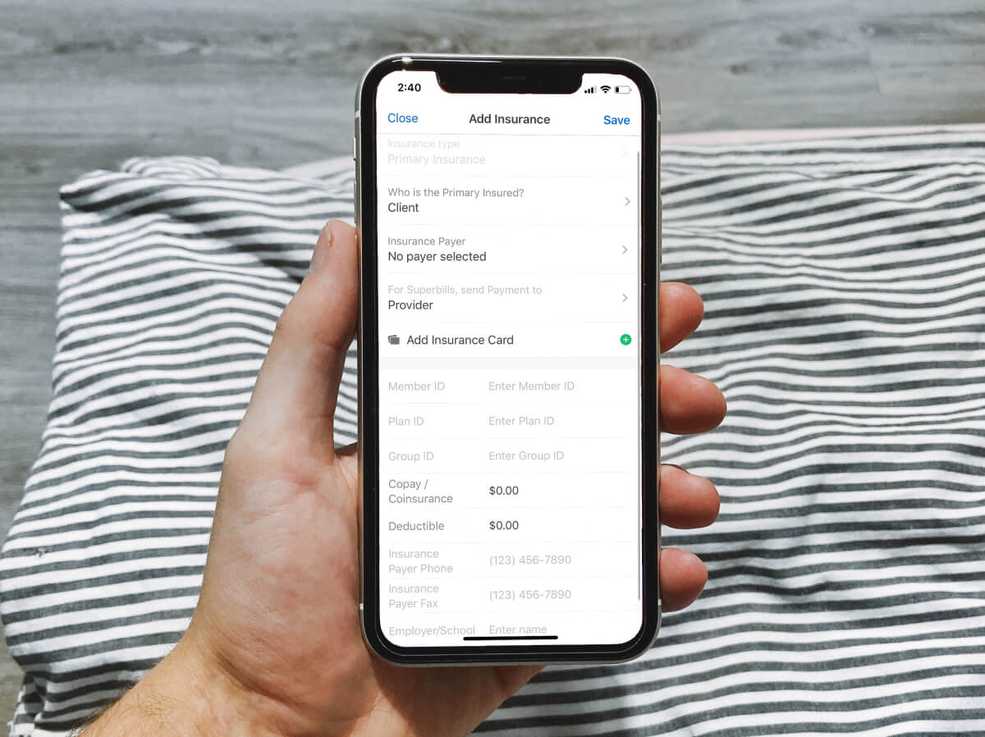
Manage client insurance information from the mobile app
Securely take a photo, upload, and store your client’s insurance card directly from the SimplePractice mobile app. There’s no need for a separate scanner, HIPAA-compliant software, or computer—you can quickly get the information you need from your client, all from the palm of your hand.
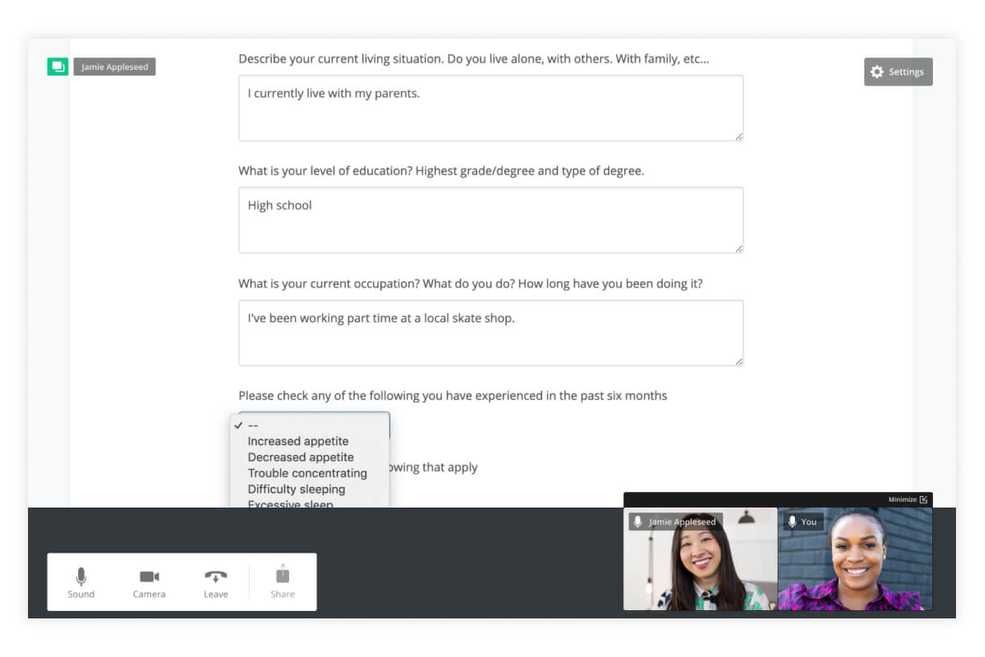
Share your screen during a Telehealth session
Screen sharing is the ability to share the images on one computer screen to another person’s screen. This allows you and your client to view the same worksheets or other documents during the session, which encourages clients to participate (so important for those younger clients!) and helps them stay engaged with the session.
Enable third parties to view and pay outstanding balances
If you have a client whose services are paid for by a third party, you now have the flexibility to grant the third party access to the Client Portal. This will allow the third party contact to view and pay outstanding balances for the client through the Client Portal.
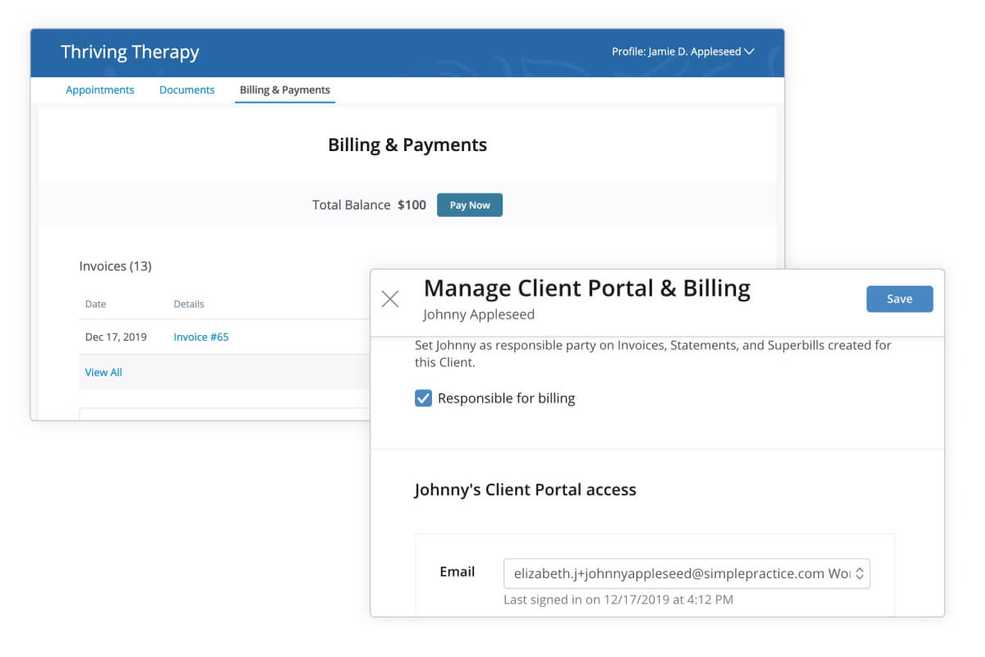
Client management for minors
For those of you who work with a minor client that has divorced parents, you’ll be able to give Client Portal access to and collect Consent Documents from both parents. If you’re working with a teenage client, you’ll be able to give them Client Portal access as well as their parents. If you see multiple children from the same family, parents will be able to access information for the whole family in one place.
