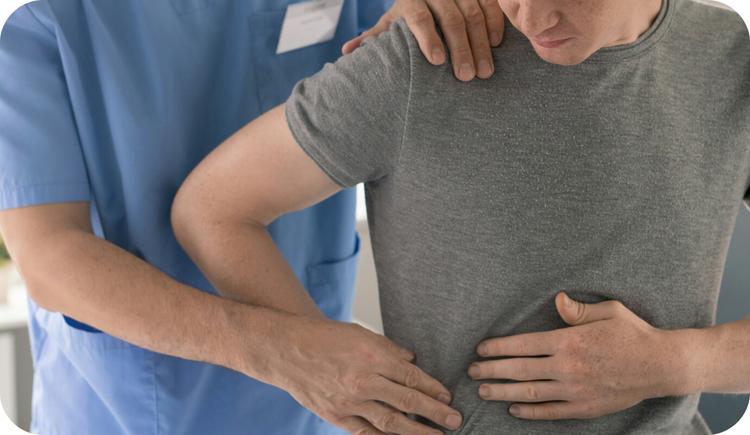
Long Range Occupational Goals
Long range occupational goals, or long-term occupational therapy goals, are created by occupational therapists (OTs) to capture what they would … Continued


How to Talk About Mental Health and Social Media
Most therapists intuitively understand the negative link between mental health and social media use—perhaps personally, as well as professionally. Personally, … Continued

What Are the 5 Stages of Psychosis?
In this article, we will be going over the 5 stages of psychosis—in addition to the various psychosis symptoms to … Continued
What Is Bipolar Disorder?
Formerly called manic-depressive illness or manic depression, bipolar disorder is a treatable mental health condition marked by extreme shifts between … Continued

How to Cope With Loneliness
Nineteen years ago, on a morning in May, I sat alone at my kitchen table, surveying my sunny Brooklyn walk-up. … Continued

How to Combat Empathetic Distress, the Shadow Side of Empathy
If you’re wondering “What is empathetic distress?” or “How does a therapist’s empathetic concern become empathetic distress?” read on for … Continued

How to Feel Good About Earning Money in Private Practice
Like all helping professionals, speech-language pathologists (aka SLPs) have invested in advanced degrees and in countless continuing education courses and … Continued
More Stories






