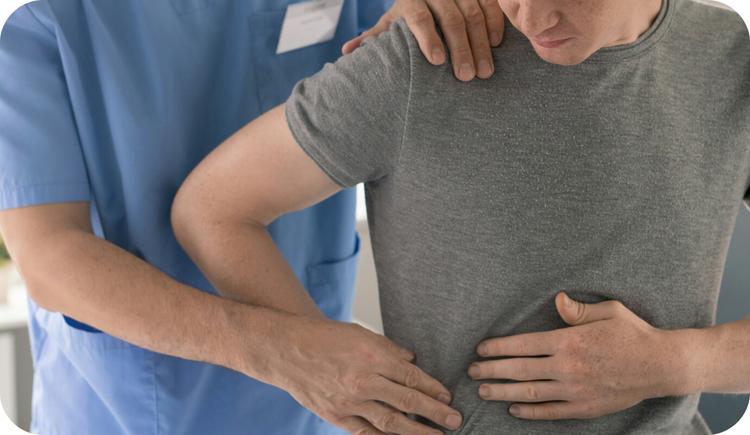
3 HIPAA Compliance Errors Therapists May Be Making
Curious about how therapists can stay HIPAA-compliant and avoid HIPAA compliance errors? Just over three years ago a Department of … Continued


Bipolar Psychosis
Bipolar psychosis, or bipolar with psychotic features, is common among those diagnosed with bipolar disorder, which is why it’s crucial … Continued
Can a Therapist Do Telehealth Across State Lines?
Modern society is incredibly mobile. Our therapy clients may cross state lines to travel for work, visit family, go away … Continued

How to Talk About Mental Health and Social Media
Most therapists intuitively understand the negative link between mental health and social media use—perhaps personally, as well as professionally. Personally, … Continued

What Are the 5 Stages of Psychosis?
In this article, we will be going over the 5 stages of psychosis—in addition to the various psychosis symptoms to … Continued
What Is Bipolar Disorder?
Formerly called manic-depressive illness or manic depression, bipolar disorder is a treatable mental health condition marked by extreme shifts between … Continued

How to Cope With Loneliness
Nineteen years ago, on a morning in May, I sat alone at my kitchen table, surveying my sunny Brooklyn walk-up. … Continued
More Stories